
President's Message: 'Leading' the Way

Marian L. Fitzgibbon, PhD, SBM President
Marian L. Fitzgibbon, PhD, SBM president
New initiatives at the Society of Behavioral Medicine (SBM) might be best summed up with one word: lead. With your needs in mind, SBM is developing a leadership training program that will help advance mid-career behavioral scientists into the next stage of their careers. We are also exploring options for partnerships that would allow members to lead the digital health industry in a direction that is more evidence-based.
Guiding Mid-Career Scientists
Plans are rapidly moving forward for a new SBM leadership institute for mid-career behavioral medicine scientists. Creating this institute is one of my presidential initiatives, and it means a great deal to me. Early career decisions are critical in helping formulate a solid career trajectory. However, too often we overlook mid-career people, who are at a pivotal point in their careers, when guidance and mentoring would help them make the crucial decisions regarding leadership opportunities and important next steps that will impact the many years ahead.
As such, this institute will focus on two domains: leadership skills and self-knowledge. In a recent survey, SBM members indicated they were most interested in the following specific topics:
- learning skills to become an effective leader and/or mentor;
- assessing and planning for career ladder/trajectory opportunities;
- understanding personal attitudes and behaviors that impact leadership effectiveness;
- conflict resolution; and
- negotiating skills regarding salaries and promotions.
We plan to pilot the program in conjunction with next year's Annual Meeting. Approximately 24 participants will meet March 29-30 (just before the Annual Meeting) for an intensive two-day training, supplemented by prior readings and self-assessment. Participants will engage in skill-building exercises, meet with coaches and mentors, and identify a leadership project to be completed during the subsequent year and presented at the 2017 Annual Meeting.
Stay tuned for details on how to apply!
Strategically Bridging the Gap between Industry and Evidence-Based Science
Digital health industry representatives are increasingly asking SBM members for help developing products that are evidence-based and, therefore, effective. As you and I know, while some apps and other digital health products reflect an evidence base, many do not. Evidence-based products can help improve users' health and build rich data banks of keen interest to behavioral medicine researchers.
SBM recently partnered with the University of Pittsburgh Katz Business School to determine how we can connect our members with industry. Sue Cohen, PhD, will use SBM as a case study in two of her classes; students will be tasked with creating a business plan for how SBM might leverage members' behavioral medicine expertise into an industry consulting enterprise. SBM leaders will make sure any resulting actions are carefully thought out and align with SBM's core values and ethics.
Again, stay tuned for more details!
As you can see, exciting things are happening at SBM! I hope these new endeavors will truly help our members lead the way and improve health.
All my best,
Marian L. Fitzgibbon, PhD
President
Society of Behavioral Medicine
Board Notes: New Council/Committee Reports and a Website Upgrade

Monica Baskin, PhD
Monica L. Baskin, PhD, Board of Directors member delegate
During the July meeting of the Society of Behavioral Medicine (SBM) Board of Directors, board members took steps to better track council and committee activities. They also approved an SBM website upgrade that will make the site more user-friendly for mobile device users.
Governance Update
Sara Knight, PhD, leader of SBM's Governance Working Group, discussed the group's recommendation that there be stronger alignment between the roles of councils/committees and SBM's strategic directions, to improve efficiency and sustainability of our efforts. Councils and committees would identify at least one strategic area that complements their ongoing charge. In addition, the working group encouraged the board to regularly review the short- and long-term outcomes of council and committee activities to better inform strategic directions and initiatives.
Based on the above recommendations, reports to the board from councils, committees, member delegates, and the president have been created or redesigned. New templates for the reports now include sections for desired outcomes, progress toward accomplishing the desired outcomes, and analysis of activities. Dr. Knight expressed to the board that the findings and recommendations from the governance review come not from any pre-existing problem or issue, but from a desire to strengthen SBM's organizational processes and ensure data-driven strategic decisions. The new reports will be given a trial run for the board's November meeting.
Website Upgrade
SBM staff member Lindsay Bullock presented a recommendation from SBM's Website/Social Media Team. SBM continues to grow its official presence on a number of social media platforms (e.g., Facebook, Twitter, and LinkedIn), which has resulted in increased "real-time" interaction among SBM members; however, limited focus has been placed on the organization's website in recent years, especially when it comes to meeting the needs of the increasing number of persons who access the site using mobile devices.
The Website/Social Media Team therefore recommended upgrading SBM's website to a "responsive" site that would be more user-friendly for mobile devise users. A responsive website automatically resizes itself based on a user's device. The upgrade would take approximately 30 days and cost approximately $2,500. The board saw the huge value in this upgrade with minimal investment and high expected return, and approved this request. Stay tuned for a new and improved website that you will be able to manipulate with any number of devices.
SBM's Journals Moving to Online Delivery
Alan M. Delamater, PhD, Publications and Communications Council chair
The Society of Behavioral Medicine's (SBM's) two journals are going green. Starting in 2016, Annals of Behavioral Medicine and Translational Behavioral Medicine: Practice, Policy, Research will switch to online delivery. Instead of getting hefty issues delivered in the mail, SBM members will receive electronic copies via email.
This switch is part of SBM's efforts to be environmentally responsible. Electronic copies will reduce the waste that pours into landfills. If you've been recycling the journals instead of throwing them away, electronic copies will make you even greener by skipping the paper usage altogether.
The switch to electronic copies will also save SBM money, making the society more viable and allowing it to invest in other critical areas like the special interest groups, health policy work, and annual meeting programming.
Beginning with the first 2016 issues of Annals of Behavioral Medicine in February and Translational Behavioral Medicine in March, SBM members will receive an emailed table of contents each time a new journal issue publishes. The email will include links to each article so that reading-or saving PDF copies-is only a click away.
Members will continue to have access to full journal archives via the "Members Only" portion of the SBM website.
If you like to save the printed journals or love the feel of one in your hands, don't worry-you can continue receiving print copies in the mail. Just email your request to info@sbm.org.
Thank you for your understanding and for supporting SBM as it moves into a greener, more sustainable 21st Century.
2016 SBM Call for Awards and Fellow Applications

New 2015 fellows pose with SBM then-President Lisa M. Klesges, PhD. Fellows are (left to right) Jennifer L. Huberty, PhD; Youngmee Kim, PhD; and Alexander J. Rothman, PhD. (Not pictured: John P. Allegrante, PhD; and Joan S. Tucker, PhD)
The Society of Behavioral Medicine (SBM) will soon be accepting applications for its 2016 achievement awards and fellow nominations. The call for applications opens October 12 and closes November 18 at 11:59 p.m. EST. For more detailed information about the awards and fellow nominations—including how to apply or nominate someone—please visit SBM's official call for awards and call for fellows Web pages. Awards recipients and fellows will be announced at SBM's 37th Annual Meeting & Scientific Sessions being held March 30 to April 2, 2016, in Washington, DC.
Call for Awards
Nominations for awards must come from current SBM members in good standing. Self-nominations are allowed.
- Distinguished Scientist Award
Selection for this award is based on the nominee's total career and great scholarly achievements (i.e., made a series of distinguished empirical contributions or contributed substantially to the development of new theories or methods). - Research to Practice Award
Selection for this award is based on the nominee's contributions and exemplary work in translating or extending behavioral medicine from research into practical application, dissemination, or implementation. - Jessie Gruman Award for Health Engagement
This award recognizes the nominee's pivotal and extensive contributions to research, practice, and/or policies that have advanced the understanding of patient engagement. - Early Career Investigator Award
This award recognizes the total career achievements and review of a representative published paper. - Outstanding Dissertation Award
Selection for this award is based on the success and excellence of a student/trainee member's defense of his or her dissertation. - Distinguished Student Awards
These awards will be given to students who demonstrate outstanding academic and professional potential in the field of behavioral medicine. Students may apply for the following awards:- Excellence in Research
- Excellence in Service Delivery
- Travel Scholarship
- Distinguished Research and Clinical Mentor Awards
Selection for these awards are focused on individuals and their outstanding service as mentors in clinical or research settings. - Excellence in Behavioral Medicine Training Program Award
This award recognizes a research- and/or clinically-focused training program. The training program can occur in any discipline and programs with an interdisciplinary approach will also be considered.
A Special Word about the Jessie Gruman Award
This is the third year SBM will be offering the Jessie Gruman Award for Health Engagement. Jessie Gruman, PhD, was an SBM fellow and prior to her passing in 2014 her colleagues created SBM's Jessie Gruman Award for Health Engagement to annually recognize an individual or organization that has made a pivotal contribution to research, practices, and policies that have advanced the understanding of patient engagement. Dr. Gruman authored several significant books on patients and their engagement, and she created useful tools and guidelines for patients. In 1992, she founded the Center for Advancing Health, a nonpartisan, Washington-based research institute that strengthened the evidence for patient engagement. Dr. Gruman served as the organization's president until her death.
The Jessie Gruman Award for Health Engagement carries on Dr. Gruman's legacy through continual recognition of individuals and organizations working toward the advancement of patient engagement. Recipients of the award are invited to deliver a master lecture in Dr. Gruman's honor during the subsequent annual meeting. At the upcoming 2016 Annual Meeting, 2015 Jessie Gruman Award recipient Michael G. Goldstein, MD, will be delivering his master lecture.
Call for Fellows
SBM fellows demonstrate the society's commitment to advancing the science and practice of behavioral medicine. Fellows serve as role models, offering guidance and support to student/trainee members. The selection of new fellows ensures the continual life and direction of SBM. To apply for fellow status a full member must be in good standing with the society for three consecutive years prior to applying and should have received his or her highest academic degree at least 10 years prior. For more information please review the fellow criteria document.
It's That Time of Year! Watch Your Mailbox for SBM Membership Renewal Info
Lorna Haughton McNeill, MPH, PhD, Membership Council chair
 It's hard to believe, but 2016 is almost here. The Society of Behavioral Medicine (SBM) will open 2016 membership renewals and new member sign ups this month.
It's hard to believe, but 2016 is almost here. The Society of Behavioral Medicine (SBM) will open 2016 membership renewals and new member sign ups this month.
Easy, one-page renewal forms are on their way to your mailbox right now. You'll also be able to renew online.
Renewing your membership means you'll be able to register for SBM's upcoming 2016 Annual Meeting at a discounted rate, saving hundreds of dollars! Renewing also means you'll also be eligible to receive one of SBM's 2016 achievement awards (the call for award applications opened October 12).
Other member benefits include access to job postings and funding opportunities; membership in one or more of SBM's behavioral medicine special interest groups; and subscriptions to SBM's two journals (Annals of Behavioral Medicine and Translational Behavioral Medicine).
Don't delay! Renew early to ensure your member benefits do not lapse. Your renewal also shows support for important SBM activities, like fighting for increased National Institutes of Health funding and focusing decision-makers' attention on behavioral medicine research to ensure health policies and digital health products are truly evidence-based.
I recall much conversation from the 2015 Annual Meeting about SBM being members' "professional home." I must say that's true for me. SBM is very much my professional home, and I hope it continues to be yours! I'm also looking forward to seeing everyone in Washington, DC, at the 2016 meeting!
New TBM Editor Suzanne Miller Hopes Partnerships with Nonprofits and Legislators Can Increase Articles' Real-World Impact

Suzanne M. Miller, PhD
Lindsay Bullock, SBM senior media and member communications manager
Incoming Translational Behavioral Medicine (TBM) Editor-in-Chief Suzanne Miller, PhD, has a dream that someday, someone like the New Jersey commissioner of health will visit the TBM website and comment on a TBM blog post about a newly published TBM paper.
Never mind that TBM doesn't currently have a blog and that the New Jersey commissioner of health has probably never heard of the journal. Where some might see roadblocks, Dr. Miller sees potential.
She's driven by one overarching goal for TBM: She wants to expand its impact. She wants more decision makers and health care providers to use TBM's evidence-based research to improve health care policies and practices.
"We really need to disseminate our findings so that they do not stay on our shelf and in the journal," Dr. Miller says.
She's quick to note she'll be building on the work already done by TBM founding Editor-in-Chief Bonnie Spring, PhD. Under Dr. Spring's leadership, TBM articles have been downloaded more than 70,000 times and the journal has been indexed in 15 archive services.
When Dr. Miller takes over from Dr. Spring in a few months, she'll work to make sure TBM's impact continues to grow.
One of her key strategies will be partnering with nonprofit health organizations. As a hypothetical, Dr. Miller describes a possible relationship with HealthWell, a nonprofit that provides cost assistance for the underinsured (she sits on its board). If a TBM article found lung cancer patients could live longer by spending time outdoors, the article editor could create a bulleted list of what oncologists might tell patients and then HealthWell could send the list to its network of 48,000 providers. HealthWell could even hold a press conference about the article to draw additional attention. HealthWell might also survey its 20,000+ patient network about article findings; results could be published online in real time.
Dr. Miller says she's already talked with HealthWell officials about such possibilities. They're excited by the idea of disseminating helpful findings, which would give greater visibility to co-payment assistance organizations like theirs.
Article findings could similarly be shared with state legislators who craft health policies, Dr. Miller adds. She's already done work like that as a founding board member of the New Jersey Health Care Quality Institute. Miller and the other founders were honored this year in a joint legislative resolution from the New Jersey Senate and General Assembly.
"I sit on a number of health policy boards designed to help improve the quality, safety, and health effectiveness of health care. I noticed on these boards, I'm generally the only health psychologist. Other members tend to be public health people, policymakers, insurers, payers, providers, and lawyers. Rarely is the psychological approach represented," she says. "On those boards, I can help speak to that as one person. But I thought the journal was an incredibly unique vehicle for potentially doing that on a very broad and impactful scale."
Dr. Miller will look for associate editors that can help strengthen policy and nonprofit relationships. She'd also like to beef up the TBM website so it includes blogs and is more interactive-someone better tell the New Jersey health commissioner to get ready.
About Suzanne Miller
Dr. Miller is an SBM fellow with a PhD in clinical psychology. She was drawn to the field while studying at McGill University. Her honors advisor, Ronald Melzack, was doing pioneering research on the psychological aspects of pain, particularly in phantom limbs.
"He was looking at pain not just in a simple self-report way but in a way that bridged brain processes with how pain was expressed, felt, and tolerated," Dr. Miller says.
She was fascinated by that research and later became interested in how people cope-not only with pain but also with everyday stresses. She eventually turned that into a long career of studying how cancer patients cope with diagnosis, make decisions about treatment, and cope with survival.
Dr. Miller founded the Department of Defense-funded Behavioral Center of Excellence in Breast Cancer and directed one of the country's first National Cancer Institute-funded behavioral core facilities. She is currently a professor of cancer prevention and control at Fox Chase Cancer Center/Temple University Health System, where she also serves as director of the Psychosocial and Bio-Behavioral Medicine Department.
Optimization of Behavioral Interventions SIG Talks with Bonnie Spring about her Study of Weight Loss Program Components

Bonnie Spring, PhD, ABPP
Kari Kugler, PhD, Optimization of Behavioral Interventions SIG co-chair
The Society of Behavioral Medicine's (SBM) new Optimization of Behavioral Interventions Special Interest Group (OBI SIG) recently interviewed Bonnie Spring, PhD, ABPP, director of the Center for Behavior and Health at Northwestern University's Feinberg School of Medicine.
The OBI SIG talked with Dr. Spring about her ongoing Opt-In research study, which aims to determine what combination of different weight loss program components is the most effective for overall weight loss.
OBI: You are halfway through your Opt-In study, which uses the multiphase optimization strategy (MOST). What made you decide to develop an optimized intervention?
Spring: It just made tremendous sense to me to go about developing an obesity treatment package from the ground up by balancing the efficacy and cost of different candidate treatment components. It has always bothered me that we tend to offer "kitchen sink" treatment packages as behavioral interventions because, most of all, we want our treatments to produce significant improvement. The problem is that this approach often leaves us with unwieldy, burdensome, very costly treatments that are difficult to scale up to reach more of the population. And despite the habit of saying we're going to conduct dismantling studies to streamline and prune back our bundled treatment packages, that research is rarely done. Because MOST uses data to drive decision making about the treatment design, it has always impressed me as a transparent means to progress toward evidence-based practice.
OBI: How difficult was it for you to understand the fundamental differences between a randomized clinical trial (RCT) and the experimental design you needed to optimize the intervention, in this case a factorial experiment?
Spring: My PhD is in personality and developmental psychology, and my doctoral training was in experimental psychopathology. The methodological tradition in these fields actually does involve the conduct of factorial experiments. I first encountered the RCT when seguing to health psychology by way of psychopharmacology. My first trials treating smoking or weight gain with drug or placebo felt very much like factorial experiments-with treatment set to on versus off. It wasn't until I discovered that patients tended to relapse whenever I withdrew drug treatment that I realized I needed to switch to behavioral treatments to achieve greater maintenance. RCTs involving behavioral interventions felt very strange to me because the intervention seemed to bundle different treatment components together rather than independently turning them on or off. I still try to perform factorial experiments when developing a behavioral treatment. I prefer not to bundle components together into a treatment package until after I've studied them as independent factors and learned their effects. So, the MOST factorial experiment approach feels very right-minded to me.
OBI: What are some considerations when it comes to the implementation of a factorial experiment? How has it been for your research staff to manage 32 experimental conditions?
Spring: Because of the complexity of having so many conditions, the staff follow an online set of prompts for the different experimental conditions. They do an excellent job of attaining treatment fidelity. Needing to be guided by the prompts makes intervention delivery a little more scripted than most interventions we do. On the other hand, I suspect that our interventionists are better able to maintain equipoise because it's more challenging for them to become attached to any single condition.
OBI: What advice would you give someone considering using MOST?
Spring: I would urge the person to specify their theoretical or conceptual model and to use it to delineate which treatment components to study. Relatedly, I would advise them to think through carefully which interactions are likely and conceptually meaningful so that the experimental design allows these to be interpretable.
OBI: How do you see MOST helping move science forward?
Spring: By helping us learn the cost-effectiveness of different intervention components for the average person and for different kinds of people, MOST can help us establish the science base needed to optimize treatments equitably to foster the health of the population.
How You Can Advocate for Health Policy Change
Joanna Buscemi, PhD, Health Policy Committee chair
Whether you are a clinician, researcher, or educator, you may have asked yourself at one point in time, "How can I use what I've learned from my work to have a greater impact on population-level health?" If you have had this thought but were unsure how to begin, the Society of Behavioral Medicine's (SBM's) Health Policy Committee (HPC) provides structured and guided opportunities for SBM members and SBM special interest groups (SIGs) to increase the impact of their work through the development and dissemination of health policy briefs.
I was recently appointed chair of the HPC. I was trained as a behavioral scientist and have always felt like I wanted to increase my involvement in advocacy and policy-related work, but wasn't sure exactly how. Through the HPC, I was able to develop several health policy briefs on issues that are important to me and to SBM members. My work on these briefs allowed me to learn how to communicate messages to policymakers and to network with experts in the field. Additionally, I have published each brief in Translational Behavioral Medicine (TBM), and have worked to disseminate the briefs widely through social media and partnering with other like-minded organizations.
Over the past year, the HPC has published the health policy briefs on SBM's website:
- Retain Healthy School Lunch Policies
- Integrating Peer Support in Prevention and Health Care Under the Affordable Care Act (ACA)
- Integrate Community Health Workers into the Patient-Centered Medical Home
In November, several members of SBM's board will visit Capitol Hill and will meet with legislative aides to discuss the importance of these and other upcoming policy briefs, and to get feedback from them on what legislators are interested in hearing from us.
The HPC encourages SIG chairs and other members to contact the HPC with concepts for briefs that are timely and in line with SBM's mission. Prior to last year's annual meeting, most of the ideas for the policy briefs were developed out of conversations between members of the HPC. Over the past several months, we have worked to encourage SBM members to come to us with ideas. It is part of my job to work as a liaison between the HPC and members to make sure that our briefs cover broad topic areas across behavioral medicine.
Additionally, the HPC has begun to adopt a model of partnering with other organizations during the development phase of the briefs to build professional collaborative relationships, and to increase the reach and dissemination of the briefs. For example, in a joint "call to action" regarding integrating peer support in prevention and health care under the Affordable Care Act, SBM partnered with the Center for Health Law & Policy Innovation at Harvard Law School, the National Council of La Raza, and Peers for Progress. Moving forward, we would like to continue to utilize this model that was expertly executed by SBM's Ed Fisher to increase the impact of these important statements. Sherri Sheinfeld-Gorin, PhD, the chair of SBM's Scientific and Professional Liaison Council (SPLC), has been working to develop relationships with like-minded organizations that may be interested in joining efforts to develop future policy briefs. The HPC has begun to partner with the SPLC to facilitate this new model.
I would like to thank the current members of the HPC: Ed Fisher, Marian Fitzgibbon, Laura Hayman, Judith Ockene, Ken Tercyak, Dawn Wilson, and Amy Yaroch.
For more information about the work of the HPC or to propose ideas for future briefs, please contact me at jbuscemi@uic.edu.
Promoting Shared Decision Making in Lung Cancer Screening
Sarah E. Lillie, PhD, MPH, Health Decision Making SIG co-chair and Outlook liaison; Margaret M. Byrne, PhD, Health Decision Making SIG member; Lisa Carter-Harris, PhD, Health Decision Making SIG member; and Jamie L. Studts, PhD, Health Decision Making SIG member
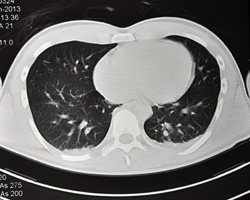
Lung cancer is the second most common cancer and the leading cause of cancer mortality in the United States, with an estimated 158,000 deaths predicted in 2015.1 Prevention (smoking cessation) is the most effective strategy for reducing the burden of lung cancer. Lung cancer screening also has the potential to reduce lung cancer mortality. The largest lung cancer screening randomized trial to date, the National Lung Screening Trial (NLST), recently compared annual low-dose computed tomography (LDCT) with chest X-ray for three years. The trial found a significant benefit for LDCT, with a 20% relative reduction in lung cancer mortality (absolute reduction 62 lung cancer deaths/100,000) and 6.7% relative reduction in all-cause mortality (absolute reduction 74 deaths/100,000).2 For those undergoing LDCT, the number needed to screen to prevent one lung cancer death was 320, a number considered by most to be cost-effective and consistent with, if not better than, other established cancer screening modalities. While LDCT-based lung cancer screening has the potential to decrease mortality from lung cancer, it also has potential harms. These harms include false-positive results, significant incidental findings, adverse psychological effects, overdiagnosis, and radiation exposure.3 With an increased appreciation of both the benefits and potential harms of medical intervention, this topic is of broad interest to Society of Behavioral Medicine (SBM) members.
The United States Preventive Services Task Force (USPSTF) recently incorporated the NLST results into revised guidelines and issued a Grade B recommendation for annual LDCT for high-risk adults aged 55-80 who are current smokers or former smokers who have quit within the past 15 years, with a 30 pack-year smoking history.4 This guideline joins an increasing number of professional organizations that promote shared decision making. Additionally, the Centers for Medicare & Medicaid Services (CMS) issued a national coverage determination for Medicare coverage of lung cancer screening with LDCT.5 While the USPSTF has advocated for the implementation of shared decision making for preventative health services for over a decade, this landmark determination by CMS is considered the first of its kind to require that shared decision making occur, and be documented, before providing reimbursement for lung cancer screening. Further, CMS has indicated that health care providers will be reimbursed for offering shared decision making consultations regarding lung cancer screening. This innovative shared decision making policy, and the reality in which it occurs, are just a few of the reasons members of the SBM Health Decision Making Special Interest Group (HDM SIG) are drawn to this fascinating topic.
To consider this notable policy stance, the HDM SIG has organized a midday meeting for the upcoming SBM Annual Meeting. This meeting will focus on policy use to promote shared decision making in lung cancer screening. An interdisciplinary panel will discuss the development of the USPSTF lung cancer screening guidelines, benefits and potential harms of lung cancer screening, the CMS policy, and implementation of lung cancer screening decision aids. The session will include ample time for what organizers anticipate to be a lively discussion. HDM SIG members look forward to seeing you in Washington, DC!
References
- American Cancer Society. Cancer Facts & Figures 2015. Atlanta: American Cancer Society; 2015.
- The National Lung Screening Trial Research Team. Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med. 2011;365(5):395-409.
- Bach PB, Mirkin JN, Oliver TK, et al. Benefits and harms of CT screening for lung cancer: a systematic review. JAMA. 2012;307(22):2418-29.
- Moyer VA; U.S. Preventive Services Task Force. Screening for lung cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2014;160(5):330-8. Recommendation statement available at: http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/lung-cancer-screening
- The Centers for Medicare & Medicaid Services. Decision Memo for Screening for Lung Cancer with Low Dose Computed Tomography (LDCT) (CAG-00439N). Available at: http://www.cms.gov/ medicare-coverage-database/details/nca-decision-memo.aspx?NCAId=274.
Complementary and Integrative Medicine in Older Adults
Katarina Friberg Felsted, Complementary and Integrative Medicine Special Interest Group member
Complementary and integrative medicine (CIM) is popular in the United States, especially-perhaps surprisingly-among older adults. Over a quarter of older adults (27%) utilize it in some form (Arcury, Suerken, Grzywacz, Bell, Lang, & Quandt, 2006). As life expectancy increases and older adults are faced with cumulative comorbidities and disabilities, their satisfaction with typical and customary medicine often wanes (Getz, 2011). Older adults often turn to alternative therapies to seek relief, either in conjunction with or instead of more traditional offerings (Cassileth, Gubili, & Yeung, 2009). CIM therapies tend to be less invasive than traditional medicine and have fewer side effects (Orzech, 2007).
As this trend in interest and use continues, more scientific research is being conducted. Structural support is building nationally: for example, the National Institutes of Health's National Center for Complementary and Integrative Health. Support is also building organizationally: for example, the Society of Behavioral Medicine's (SBM's) CIM Special Interest Group (SIG). Many academic and professional journals are also advancing the science of CIM. As this body of research grows, it intersects with another growing trend: team science. The scientific community is seeing an increase of interdisciplinary, multidisciplinary, and transdisciplinary collaboration. Within SBM, there are over 20 SIGs, and the increase in team science translates into cross-SIG opportunities.
CIM offers treatment and relief for issues and illnesses that are often the most common in an older adult population. Fatigue, cancer symptoms, chronic pain, mood disturbances, and the like are often addressed using effective complementary and alternative therapies. Studies along this vein encourage interaction between many of SBM's SIGs. Much attention is being paid to mind body therapies in older adults, such as yoga and mindfulness. These studies are encouraging in their findings, showing improvements in such varied arenas from decreased insulin levels to relief of bronchial asthmatic episodes (Kooperman & Ackerman, 2005). Additional chronic conditions and their symptoms are being treated with these modalities, including depression, anxiety, chronic fatigue syndrome, and symptoms of cardiovascular disease, type 2 diabetes, and rheumatoid arthritis (Merkes, 2010). Pertinent cross-SIG collaborations could appropriately be developed between the CIM SIG and the Cancer, Health Decision Making, and Multi-Morbidities SIGs. Often, researchers are finding that conditions that were assumed to be purely physiological in nature may also have some psychological etiology, and application of mind-body therapies is producing positive results. One such area is urinary incontinence. Previously believed to be a bladder problem, recent research is highlighting the likelihood that incontinence is caused, at least in part, by an abnormal psychological reaction referred to as catastrophizing (Baker, Costa, and Nygaard, 2012).
Catastrophizing is imagining the worst possible outcome and assuming that the negative outcome will actually be a catastrophe (Bailey, 2013). Irritable bowel syndrome has also been found to have substantial psychological components (Zernicke, Campbell, Blustein, Fung, Johnson, Bacon, & Carlson, 2013).
Mindfulness-based stress reduction, pioneered by Jon Kabat-Zinn in the late 1970s, is showing relief of both symptoms and bother when used to treat urinary urge incontinence in middle aged women (Baker, Costa, & Nygaard, 2012). For example, a recent trial found that an eight week course of mindfulness-based stress reduction significantly reduced urinary urge incontinence episodes in younger and middle aged adults, and this was still the case at the one year follow-up (Baker, Costa, Guarino, & Nygaard, 2014). Older adults are often marginalized in scientific research, and CIM is yet another instance where studies involving them as the target population could advance science considerably if they would be included. A study of mindfulness-based stress reduction as a treatment for urinary urge incontinence could be moved into the older adult population to see if results hold. In the future, complementary and integrative modalities may prove to be increasingly important to a variety of health issues in older adults. This area of research further encourages cross-SIG opportunities between the CIM SIG and Aging, Spirituality and Health, and Women's Health SIGs.
Research Recruitment Strategies for Women in the Reproductive Period
Jennifer Matthews; Maja Pedersen; and Jennifer Huberty, PhD, Women's Health SIG co-chair

The Women's Health Special Interest Group had a panel discussion at the Society for Behavioral Medicine (SBM) 2015 Annual Meeting. Experts in the field of women's health shared experiences and ideas on recruiting women in the reproductive period into research studies (Panel discussants: Jennifer Huberty, PhD, Arizona State University; Jenn Leiferman, PhD, University of Colorado Denver; and Danielle Downs, PhD, The Pennsylvania State University). Here are a few highlights from the discussion, focused on relationship building and communication.
Building Partnerships
Creating positive relationships across a community can open doors and spark connections that result in meaningful partnerships for recruitment. Being willing to introduce yourself to others, ask new acquaintances out to coffee or lunch, or have the courage to "cold-call" key individuals may be an important step to gain access to specific populations.
Organizations/locations for potential partnerships:
- Mother-baby forums (search for local forums in your geographic area)
- Community centers, such as health and fitness or social centers
- Health clinics offering reproductive health care
- Retail stores catering to mothers, babies, and children
Communicating Positive Impact
Before initiating a potential partnership or collaboration, reflect on how the research can positively impact the individuals/organizations with whom you might partner. This can also include incentives provided to participants. Throughout your communication with a potential partner, be sure to emphasize this prospective impact.
Questions to reflect on before communicating with a potential partner/collaborator:
- How might you address the needs of the potential partner/collaborator through your research?
- What aspects of the research process or outcomes might directly benefit the members, patients, or employees of this organization?
- How might the organization as a whole benefit from this partnership?
Leveraging Linkages
Create a link rooted in common interests between private entities (such as health care providers or small business owners), public organizations (such as public non-profit organizations or the local health department), and community members (such as representatives from local coalitions or members of the target population). Creating a panel of community leaders as an advisory group for your research can help to develop a well-received recruitment plan, and can spread the word about your research.
Finding community panel members:
- Look and listen for names of individuals who are mentioned frequently in the targeted community; you are looking for someone who is well connected and respected
- Look for health care providers who will "champion" your research-it is worth the time to find a provider who is interested and engaged in your cause
- Include gatekeepers, particularly passionate peer-leader figures
Once you have found the linkages, leverage panel members' connections to helpful coalitions or volunteer groups that might be willing to contribute time or man/woman-power to your research, perhaps by spreading recruitment materials or sharing a blurb about your research at a social event.
Another resource can be women from your previous studies; asking questions about how to recruit their peers and engaging them in recruitment via word of mouth can be powerful tools.
Recent Advances in Multiple Health Behavior Change
Jayson J. Spas, PhD, MS, LMFT, Multiple Health Behavior Change SIG co-chair; and Lori A. J. Scott-Sheldon, PhD, Multiple Health Behavior Change SIG chair
Multiple health behavior change (MHBC) is increasingly recognized as critical to reducing modifiable risk behaviors that often occur in clusters and are associated with chronic diseases (Prochaska et al., 2008; Spring et al., 2012). Growing evidence demonstrates that interventions targeting multiple co-occurring health risk behaviors, rather than a single health risk behavior one at a time, may have a greater impact preventing chronic illness and ultimately improving public health (Prochaska, 2008). The National Institutes of Health's (NIH's) report on the science of behavior change (2009) identified the simultaneous change in multiple health risk behaviors as a top priority. Understanding the why, how, and under what circumstances of changing multiple health behaviors will be critical for guiding research and practice toward an integrative model of multiple behavior change.
MHBC is grounded in the ever-growing demands for more rigorous evaluation of intervention efficacy, effectiveness, and cost-efficiency. Toward that end, there have been several advances in MHBC including the recent move to link treatment outcomes from separate behaviors to behavior pairs when evaluating intervention efficacy on multiple health behavior risks. This shift is innovative for several reasons. First, it challenges the separate behavior paradigm that dominates current methodology to establish intervention efficacy and effectiveness. Second, it provides a novel approach to help advance the knowledge-base and scientific evaluation of the underlying mechanisms and interrelationships of behavioral interventions for MHBC. Third, it provides an alternative analytic approach that may reveal synergistic effects that are currently undetected by the dominant separate behavior paradigm and its analytic approaches. One example is using stage-based, interactive, and computer-tailored interventions from the Transtheoretical Model (TTM) when investigating smoking, diet, and several other behavioral risks. Recent research found that individuals exposed to an intervention who progressed to a healthy criterion on one behavior were more likely to progress to a healthy criterion on a second behavior compared to those participants in the same intervention who did not move to a healthy criterion on the first behavior (Paiva et al., 2012). This phenomenon is defined as coaction and it refers to the extent to which change on one behavior is associated with change on a second behavior at the same follow-up time point.
Presently, MHBC is in its nascent stages and many important questions remain unanswered including: How does change in one behavior affect change in another behavior? Are there synergistic effects to simultaneous intervention? How does MHBC vary by different behavior pairs? Are there differences when addictive behaviors (e.g., smoking, alcohol use) are paired together with energy balance behaviors (e.g., exercise, diet) and preventive care behaviors (e.g., screenings)? These unanswered questions and the recent advances in MHBC make this an especially exciting time for MHBC research. Taken together, not only can MHBC help the NIH achieve its mission of turning discovery into health, but it can help translate behavioral interventions from "bench to bedside to public health" in order to help extend healthy life and reduce the burdens of illness and disability.
References
Paiva AL, Prochaska JO, Yoin H, Redding C, Rossi JS, Blissmer B, Robbins M, Velicer WF, Lipschitz J, Amoyal N, Babbin S, Blaney C, Sillice M, Fernandez A, McGee H, Horiuchi S (2012): Treated individuals who progress to action or maintenance for one behavior are more likely to make similar progress on another behavior: Coaction results of a pooled data analysis of three trials. Preventive Medicine, 54 (5), 331-334.
Prochaska, J.O. (2008). Multiple health behavior research represents the future of preventive medicine. Preventive Medicine, 46, 281-285.
Spring, B., Moller, A. C., & Coons, M. J. (2012). Multiple health behaviours: Overview and implications. Journal of Public Health, 34 (Suppl 1), i3-i10.
Ryan Rhodes Talks about Theory: Past, Present, and Future
Theories and Techniques of Behavior Change Interventions Special Interest Group Chairs David M. Williams, PhD, Arlen C. Moller, PhD, Heather L. Gainforth, PhD, and Dejan Magoc, PhD

Ryan Rhodes, PhD
In anticipation of the Theories and Techniques of Behavior Change Interventions Special Interest Group (TTBCI SIG) Society of Behavioral Medicine (SBM) 2016 Annual Meeting debate on the utility of social cognitive theories, we interviewed debate participant and theory expert Ryan Rhodes, PhD, to ask him about his views on the role of theory in behavioral medicine research.
Dr. Rhodes is an SBM fellow, a senior scientist of the Canadian Cancer Society, and professor and director of the Behavioural Medicine Laboratory at the University of Victoria.
TTBCI: How did you become interested in testing and refining health behavior theories as a primary aim of your research?
Dr. Rhodes: "I have always been interested in why people do what they do, particularly individual differences: Why does one person find something exciting and fun, but another person has another interpretation? This led me to study personality traits early in my career and then to the affect domain, the convoluted relationship between perceived ability and motivation, nonconscious processes, and the intention-behavior relationship."
TTBCI: In a nutshell, what is your perspective on the social cognitive theories that are currently predominant in health behavior science?
Dr. Rhodes: "They are based heavily on rationalist perspectives of benefits versus barriers or expectancy/value. Clearly this is important and the benefits of health-related behaviors drive most of the reasons for intervention. However, the affective and built environment domains are not as well articulated in social-cognitive theories. So the rise of other models, such as the socioecological framework, self-determination theory, and dual-process models, addresses some of the weaknesses of traditional social cognitive theories."
TTBCI: What sort of research is needed to make health behavior theories more explanatory and more useful?
Dr. Rhodes: "I think the day of the observational design as a method to validate a theory is coming to an end. Experimental work represents the best practical test of a theory in terms of its deliverable parts and content as well as behavior change as the outcome. This shift from observational to experimental research will benefit theory testing of all types in the future. In fact, one could argue that the problem with social cognitive theories is that they have not been appropriately tested."
TTBCI: Can you name a few favorite papers that you think have made an important contribution to advancing theories and techniques of behavior change over the last decade?
Dr. Rhodes: "There are many excellent papers from several scientists that have challenged existing theory and tried to advance theory, from work in the affect domain to nonconscious dual process models. I think the mediation article by Baranowski, Anderson, and Carmack (1998, American Journal of Preventive Medicine, 15, 266-297) was very influential in summarizing the need for theories in interventions. Susan Michie's work has also been instrumental in linking theory to intervention techniques (e.g., Michie et al., 2013, Annals of Behavioral Medicine, 46, 81-95). Papers by Sniehotta, Presseau, and Araújo-Soares, and Head and Noar (2014, Health Psychology Review, 8, 1-7, 34-52) have definitely stirred the pot recently, which has created some excellent commentary on theory and health behavior change. Likewise, the rise of self-determination theory has helped bring affect to the forefront."
TTBCI: Is there a paper or chapter you're most proud of?
Dr. Rhodes: "Still working on it. But, some of the papers I may be most proud of so far are those that I feel passionate about, but have been difficult to publish through peer review, such as papers that challenge the motivational and ability confound in self-efficacy assessment (Rhodes & Courneya, 2003, Psychology & Health, 18, 79-91; Rhodes, & Blanchard, 2007, Journal of Applied Social Psychology, 37, 753-768). My review paper on personality traits and physical activity was a reflection of the reason I got into behavioral medicine research, and so was something I wanted to write for several years (Rhodes & Smith, 2006, British Journal of Sports Medicine, 40, 958-965). Also, my recent work on predictors of intention-behavior discordance (Rhodes & de Bruijn, 2013, Exercise and Sports Sciences Reviews, 41, 201-207; Rhodes & Yao, 2015, International Journal of Behavioral Nutrition and Physical Activity, 12, 1-15) and tackling the huge literature on correlates of sedentary behavior was a fun challenge (Rhodes, Temmel, & Mark, 2012, American Journal of Preventive Medicine, 42, e3-28)."
New Articles from Annals of Behavioral Medicine and Translational Behavioral Medicine
SBM's two journals, Annals of Behavioral Medicine and Translational Behavioral Medicine: Practice, Policy, Research (TBM), continuously publish online articles, many of which become available before issues are printed. Three recently published Annals and TBM online articles are listed below.
SBM members who have paid their 2015 membership dues are able to access the full text of all Annals and TBM online articles via the SBM website by following the steps below.
- Go to the Members Only section of the SBM website (https://www.sbm.org/membership/members).
- Log in with your username and password.
- Click on the Journals link (listed third in the list of member benefits).
- Click on the title of the journal which you would like to electronically access.
To check if you are a current SBM member, or if you are having trouble accessing the journals online, please contact the SBM national office at info@sbm.org or (414) 918-3156.
Annals of Behavioral Medicine
Re-examining the Contributions of Faith, Meaning, and Peace to Quality of Life: a Report from the American Cancer Society’s Studies of Cancer Survivors-II (SCS-II)
Authors: Andrea L. Canada , Patricia E. Murphy, George Fitchett, Kevin Stein
Abstract: Prior research on spirituality in cancer survivors has often failed to distinguish the specific contributions of faith, meaning, and peace, dimensions of spiritual well-being, to quality of life (QoL), and has misinterpreted mediation analyses with these indices. We hypothesized a model in which faith would have a significant indirect effect on survivors’ functional QoL, mediated through meaning and/or peace. Data were from the American Cancer Society’s Study of Cancer Survivors-II (N = 8405). Mediation analyses were conducted with the Functional Assessment of Chronic Illness Therapy–Spiritual Well-being Scale (FACIT-Sp) predicting the mental component summary (i.e., mental functioning) as well as the physical component summary (i.e., physical functioning) of the SF-36. The indirect effect of faith through meaning on mental functioning, 0.4303 (95 % CI, 0.3988, 0.4649), and the indirect effect of faith through meaning and peace on physical functioning, 0.1769 (95 % CI, 0.1505, 0.2045), were significant. The study findings suggest that faith makes a significant contribution to cancer survivors’ functional QoL. Should future longitudinal research replicate these findings, investigators may need to reconsider the role of faith in oncology QoL studies.
Longitudinal Care Improves Cessation in Smokers Who Do Not Initially Respond to Treatment by Increasing Cessation Self-Efficacy, Satisfaction, and Readiness to Quit: A Mediated Moderation Analysis
Authors: Rachel J. Burns , Alexander J. Rothman, Steven S. Fu, Bruce Lindgren, David M. Vock, Anne M. Joseph
Abstract: The Tobacco Longitudinal Care study was a randomized controlled trial for smoking cessation. It demonstrated that longitudinal care for smoking cessation, in which telephone-based counseling and nicotine replacement therapy were offered for 12 months, was more effective than the standard 8-week treatment. This study aims to identify for whom and how longitudinal care increased the likelihood of abstinence. Mediated moderation analyses were utilized across three time points. There was a trend towards smokers who did not respond to treatment (i.e., were still smoking) by 21 days being more likely to be abstinent at 6 months if they received longitudinal care rather than usual care. Similarly, those who did not respond to treatment by 3 months were more likely to be abstinent at 12 months if they received longitudinal care. At both time points, the likelihood of abstinence did not differ across treatment conditions among participants who responded to treatment (i.e., quit smoking). The effect on 6-month outcomes was mediated by satisfaction and readiness to quit. Cessation self-efficacy, satisfaction, and readiness to quit mediated the effect on 12-month outcomes. The effect of treatment condition on the likelihood of abstinence at 18 months was not moderated by response to treatment at 6 months. Smokers who did not respond to initial treatment benefited from longitudinal care. Differential effects of treatment condition were not observed among those who responded to early treatment. Conditional assignment to longitudinal care may be useful. Determining for whom and how interventions work over time will advance theory and practice.
Theory-Driven Longitudinal Study Exploring Indoor Tanning Initiation in Teens Using a Person-Centered Approach
Authors: Joel Hillhouse, Rob Turrisi, Michael J. Cleveland, Nichole M. Scaglione, Katie Baker, L. Carter Florence
Abstract: Younger indoor tanning initiation leads to greater melanoma risk due to more frequent and persistent behavior. Despite this, there are no published studies exploring the predictors of indoor tanning initiation in teen populations. This longitudinal study uses latent profile analysis to examine indoor tanning initiation in indoor tanning risk subgroups from a national sample of female adolescents. Latent profile analysis used indoor tanning beliefs and perceptions to identify indoor tanning initiation risk subgroups. The teens in each subgroup were reassessed on indoor tanning initiation after a year. Three subgroups were identified: a low risk, anti-tanning subgroup (18.6 %) characterized by low scores on positive indoor tanning belief scales and high scores on beliefs about indoor tanning dangers; a moderate risk aware social tanner subgroup (47.2 %) characterized by high scores on positive indoor tanning belief scales but also high scores on beliefs about indoor tanning dangers; and a high risk risky relaxation tanner subgroup (34.2 %) characterized by high scores on positive indoor tanning belief scales and low scores on beliefs about indoor tanning dangers. Teens in the aware social tanner and risky relaxation tanner subgroups were significantly more likely to initiate indoor tanning in the following year. These findings highlight the need to identify teens at risk for indoor tanning initiation and develop tailored interventions that will move them to the lowest risk subgroup. Subgroup correlates suggest parent and peer-based interventions may be successful.
Translational Behavioral Medicine
A review of diabetes prevention program translations: use of cultural adaptation and implementation research
Authors: Rachel G. Tabak, Kàimi A. Sinclair, Ana A. Baumann, Susan B. Racette, Anne Sebert Kuhlmann, Michelle D. Johnson-Jennings, Ross C. Brownson
Abstract: The Diabetes Prevention Program (DPP) has been shown to prevent type 2 diabetes through lifestyle modification. The purpose of this study was to describe the literature on DPP translation, synthesizing studies using cultural adaptation and implementation research. A systematic search was conducted. Original studies evaluating DPP implementation and/or cultural adaptation were included. Data about cultural adaptation, implementation outcomes, and translation strategies was abstracted. A total of 44 were included, of which 15 reported cultural adaptations and 38 explored implementation. Many studies shortened the program length and reported a group format. The most commonly reported cultural adaptation (13 of 15) was with content. At the individual level, the most frequently assessed implementation outcome (n = 30) was adoption. Feasibility was most common (n = 32) at the organization level. The DPP is being tested in a variety of settings and populations, using numerous translational strategies and cultural adaptations. Implementation research that identifies, evaluates, and reports efforts to translate the DPP into practice is crucial.
Intervention leads to improvements in the nutrient profile of snacks served in afterschool programs: a group randomized controlled trial
Authors: Michael W. Beets, Brie Turner-McGrievy, R. Glenn Weaver, Jennifer Huberty, Justin B. Moore, Dianne S. Ward, Darcy A. Freedman
Abstract: Widely adopted nutrition policies for afterschool programs (ASPs) focus on serving a fruit/vegetable daily and eliminating sugar-sweetened foods/beverages. The impact of these policies on the nutrient profile of snacks served is unclear. Evaluate changes in macro/micronutrient content of snacks served in ASPs. A 1-year group randomized controlled trial was conducted in 20 ASPs serving over 1700 elementary-age children. Intervention ASPs received a multistep adaptive framework intervention. Direct observation of snack served was collected and nutrient information determined using the USDA Nutrient Database, standardized to nutrients/100 kcal. By post-assessment, intervention ASPs reduced total kcal/snack served by 66 kcal (95CI −114 to −19 kcal) compared to control ASPs. Total fiber (+1.7 g/100 kcal), protein (+1.4 g/100 kcal), polyunsaturated fat (+1.2 g/100 kcal), phosphorous (+49.0 mg/100 kcal), potassium (+201.8 mg/100 kcal), and vitamin K (+21.5 μg/100 kcal) increased in intervention ASPs, while added sugars decreased (−5.0 g/100 kcal). Nutrition policies can lead to modest daily caloric reductions and improve select macro/micronutrients in snacks served. Long-term, these nutritional changes may contribute to healthy dietary habits.
Development and design of an intervention to improve physical activity in pregnant women using Text4baby
Authors: Jennifer Huberty, Lacey Rowedder, Eric Hekler, Marc Adams, Emily Hanigan, Darya McClain, Mary Balluff, Matt Buman, Jessica Bushar
Abstract: Text4baby is a free, mobile health information service for pregnant and post-partum women. This study aims to understand preferences of physical activity text messages (SMS), sequentially develop prototype SMS, and determine preferred dose of SMS to inform a future study utilizing Text4baby. This study had a user-centered design with three phases: (1) literature review and interviews with pregnant women for development of prototype SMS, (2) interviews with health care professionals and pregnant women for prototype SMS feedback, and (3) survey to determine preferred dose of SMS. Data from interviews identified knowledge and support as major themes. Prototypes were developed (N = 14) and informed 168 SMS. Pregnant women (N = 326) thought three SMS/week were about right (50.2 %) and preferred three SMS/week throughout pregnancy (71.9 %). There is a need for opportunities for behavioral scientists to incorporate evidence-based practices within scalable interventions. As such, this research will inform utilization of Text4baby to potentially improve physical activity participation.
Honors and Awards
Congratulations to the following Society of Behavioral Medicine (SBM) members who recently received awards or were otherwise honored. To have your honor or award featured in the next issue of Outlook, please email lbullock@sbm.org.
Rachel J. Burns, PhD
Dr. Burns is the recipient of a postdoctoral fellowship from the Canadian Institutes of Health Research. Fellowships provide support for highly qualified candidates in all areas of health research at the post-PhD degree or post-health professional degree stages to add to their experience by engaging in health research either in Canada or abroad.
Joanna Buscemi, PhD
Dr. Buscemi was awarded an American Psychological Association Achievement Award for Early Career Professionals in August 2015.
Marian L. Fitzgibbon, PhD
Dr. Fitzgibbon, the current SBM president, has been named director of the University of Illinois at Chicago's (UIC's) new Program for Child Health Research. The program will be housed within the Pediatrics Department in UIC's College of Medicine. The Program for Child Health Research will consist of faculty who conduct research that promotes the health of children, adolescents, young adults, and families. A particular focus will be on health disparities, including health outcomes for underserved and minority populations.
Craig M. Jenkins, PhD
Dr. Jenkins was recently awarded the Surgeon General of the Army's "A Proficiency" designation.
Ann Blair Kennedy, LMT, DrPH
Dr. Kennedy was a member of the American Massage Therapy Association's Governance Committee, which won the association's National Outstanding Group Award during its national convention in August in Pittsburgh, PA.
Eric S. Kim, PhD
Dr. Kim was named one of the 30 top thinkers under 30 by Pacific Standard. For his research in positive psychological functioning and physical health, he was dubbed, "the positive psychologist who believes in associating with those who challenge you."
Qian Lu, PhD, MD
Dr. Lu has been awarded the 2015 American Psychological Association Division 38 Outstanding Contributions to Health Psychology by an Early Career Professional Award.
Suzanne M. Miller, PhD
The New Jersey Senate and General Assembly this year honored Dr. Miller and the other founders of the New Jersey Health Care Quality Institute for their work. The senate and general assembly issued a joint legislative resolution.
Joshua K. M. Nan, PhD
Dr. Nan presented his PhD research on using clay work for treating depression patients in June 2015 at the Post-Graduate Conference of the Faculty of Social Sciences, at The University of Hong Kong. He won a Best Poster Presentation Award.
Cynthia Thomson, PhD, RD
Dr. Thomson was recently honored at the Influential Health & Medical Leaders awards ceremony for medical researchers in Southern Arizona. Dr. Thomson was recognized for her comprehensive research program focused on diet, physical activity, and obesity in cancer survivors. She is currently the principal investigator of the largest national study in ovarian cancer and lifestyle behaviors. The LiVES (Lifestyle Intervention for oVarian cancer Enhanced Survival) study is designed to test the role of a healthy diet and physical activity on ovarian cancer survival.
Members in the News
The following Society of Behavioral Medicine (SBM) members and their research were recently featured in news articles or videos. To have your news spot featured in the next issue of Outlook, please email lbullock@sbm.org.
Joanna Buscemi, PhD
Dr. Buscemi was featured in a September 30 Chicago Tribune article about an elementary school that has added physical activity breaks to the school day. In the article, Buscemi endorses the breaks and explains research evidence (as outlined in a 2014 SBM health policy brief) shows that physical activity can improve students' academic achievement.
Jiun-Hau Huang, SM, ScD
Dr. Huang's research at National Taiwan University shows that female college students' intentions to use tampons were mostly influenced by positive attitudes and supportive subjective norms, moderated by sexual orientation and gender characteristic (butch/femme identity). His work was featured in August by several media outlets, including Central News Agency, UDN, NOW News, Liberty Times Net, and China Times.
Suzanne M. Miller, PhD, and Michael A. Diefenbach, PhD
Drs. Miller and Diefenbach are quoted in a September 21 Wall Street Journal article about a study analyzing how men and women approach prostate and breast cancer diagnoses and treatments in social media posts. The study found men are more analytical while women are more emotional. Drs. Miller and Diefenbach questioned the reliability of the study sample.
Joshua K. M. Nan, PhD, and Rainbow T.H. Ho, PhD
Drs. Nan and Ho were featured in a July 27 Hong Kong Economic Journal newspaper article addressing the World Health Organization's concern of the social factors affecting health. They advocated creative arts therapy (including art, music, dance/movement, and drama) as an essential social factor to promote well-being and as an alternative behavioral medicine therapy among mainstream treatments of mental illness.
Sherry L. Pagoto, PhD
Dr. Pagoto was featured in an August Allure magazine feature about the dangers of indoor tanning and the role colleges play. "Indoor tanning is the prime suspect behind the alarming rise in melanoma rates among young people," the article's sub-headline proclaims. "So why do so many colleges let their students tan for free right on or near campus?"
John M. Salsman, PhD, and Heather S. Jim, PhD
Drs. Salsman and Jim were featured in an August 10 Reuters Health article showcasing their studies about the impact of patient spirituality on cancer care. The article says, "Cancer patients who report more religiousness or spirituality may also experience fewer physical symptoms of cancer and treatment and more social connection, several new papers suggest. The new analyses reviewed previous studies of spirituality involving more than 44,000 cancer patients altogether. The studies varied in many ways, but religion and spirituality were associated with better health regardless of specific religion or set of spiritual beliefs."
Classified Advertising
Deadline and Rates
To advertise in the winter 2016 edition of Outlook, please supply ad copy to the SBM national office. Please contact the national office for additional information.
Contact:
Andrew Schmidt
Administrative Assistant
Society of Behavioral Medicine
555 East Wells Street, Suite 1100
Milwaukee, WI 53202-3823
Phone: (414) 918-3156
Fax: (414) 276-3349
Email: aschmidt@sbm.org
BOARD OF DIRECTORS
Officers
Marian L. Fitzgibbon, PhD
President
James F. Sallis Jr., PhD
President-Elect
Lisa M. Klesges, PhD
Past-President
Michael A. Diefenbach, PhD
Secretary/Treasurer
Monica L. Baskin, PhD
Member Delegate
Elliot J. Coups, PhD
Member Delegate
Amy L. Yaroch, PhD
Member Delegate
Council Chairs
Ellen Beckjord, PhD, MPH
Digital Health Council Chair
Nicole Zarrett, PhD
Education, Training, and Career Development Chair
Paul A. Estabrooks, PhD
Health Policy Chair
Lorna Haughton McNeill, MPH, PhD
Membership Chair
Alan M. Delamater, PhD
Publications and Communications Chair
Sherri Sheinfeld Gorin, PhD
Scientific and Professional Liaison Chair
Kristi D. Graves, PhD
Special Interest Groups Chair
Committee Chairs
Edwin B. Fisher, PhD
Awards Chair
Sherry L. Pagoto, PhD
Civic and Public Engagement Chair
Brent Van Dorsten, PhD
Development Chair
Ken Resnicow, PhD
Evidence-Based Behavioral Medicine Chair
Michael A. Diefenbach, PhD
Finance Chair
Joanna Buscemi, PhD
Health Policy Chair
Lisa M. Klesges, PhD
Nominating Chair
Kathleen Wolin, ScD
Program Chair
David X. Marquez, PhD
Program Co-Chair
Editors
Kevin S. Masters, PhD
Annals of Behavioral Medicine Editor
Bonnie Spring, PhD, ABPP
Translational Behavioral Medicine Editor
William J. Sieber, PhD
Outlook Editor
Rajani S. Sadasivam, PhD
Website Editor
Guidelines for Articles Submitted to Outlook
- Articles should be no longer than 500 words with up to 10 references.
- Please submit only original articles, not articles that have been previously published in another organization's newsletter or bulletin.
- The Outlook editor may edit articles to fit the format of the newsletter and may defer articles to another issue based on space limitations. The submitting author(s) will be informed prior to publication and will be sent a copy of any edited article for approval or withdrawal.
- Submitted articles may be reviewed by the Publications and Communications Committee chair and, potentially, additional Society of Behavioral Medicine (SBM) Board members to determine appropriateness for publication and/or length.
Please send Outlook correspondence to:
William J. Sieber, PhD
Editor
SBM Outlook
Email: bsieber@ucsd.edu
![]()
Society of Behavioral Medicine
555 East Wells Street, Suite 1100, Milwaukee, WI 53202-3823
Phone: (414) 918-3156 • Fax: (414) 276-3349 •
Email: info@sbm.org • www.sbm.org
Editor: William J. Sieber, PhD
Managing Editor: Lindsay Bullock
If you do not wish to be included in our mailing list, please forward this message to info@sbm.org.

