Editor's Note
 William J. Sieber, PhD
William J. Sieber, PhD
How do you obtain/apply for a leadership position in SBM?
- SBM leaders have an open door policy----feel free to reach out to any committee, council, or SIG chair and ask how you can be involved. If you join a committee, council, or SIG, my advice is to be an active participant. This means not just attending calls but volunteering to take on projects. Having been in numerous roles, I have observed that volunteers who participate in meaningful ways and go above and beyond just showing up are the ones who end up getting nominated for leadership roles.
As a graduate student or postdoc, how do you establish mentorships, either formally or informally? Do you have strategies for those of us who are more introverted? What are you looking for in a mentee?
- It is important to approach mentorship as a two-way street. This is especially the case for informal mentorship---faculty have to prioritize their primary mentees---adding new mentees stretches their time. Consider what you can offer to help make that commitment work for them. For example, could you offer to analyze some data or draft manuscripts? As much as I would love to take on every person who approaches me, I only have so much time. If someone offers to help out on projects though, it creates time for me to put into mentoring them. When somebody approaches me only asking for my help but not offering to contribute to my lab in any way, it is far more difficult for me to take them. It is also a red flag from a team science perspective---good team players are always thinking about how they can contribute to the team mission, not just how the team can help move their personal mission forward. I always ask prospective mentees what they are hoping for in a position. I get concerned if they share a long list of things they hope to get with no mention of how they would like to contribute.
- Establishing mentors is a key activity at every career stage, and there are several methods to establish formal and informal mentors during graduate school and as a post-doctoral fellow. There are several mentoring opportunities available through the Society of Behavioral Medicine, including:
- Participating in in-person mentoring opportunities at the annual meeting, such as “Meet the Professors” and other mentoring sessions offered by the Special Interest Groups (SIGs).
- Online opportunities, including the career development and training webinar series or contacting an SBM consultant.
- For introverted individuals, some good strategies to establish strong mentoring relationships could include seeking out 1:1 time with potential mentors to have conversations. As introverts often prefer time to process ideas in advance of discussion, it is useful to incorporate this into how you work with your mentor. For example, let your primary mentor know that you tend to be introverted, and offer advice on how you could work best together. For example, you might note that introverts often need time to reflect on new information before forming an opinion, and you could note this means you may need to digest their advice in between mentor visits before determining the best course of action. In addition, trying to engage with potential mentors in a more informal setting may be useful, such as the group mentoring opportunities offered at the annual SBM meeting.
- Our council members also discussed some of the following characteristics we are looking for in a mentee: enthusiastic, organized and able to follow through with tasks, not afraid to ask questions, curious, able to manage stress well, and emotional maturity.
If you could go back and tell yourself as a postdoc (or graduate student) one piece of wisdom you wish you knew then, what would you say?
- It’s all going to work out.
- This is a great question – the ETCD council has previously discussed how it is key to “keep the long game in mind”, as one’s career spans a long trajectory and the short-term challenges should not keep you from losing sight of your overarching progress and goals. In addition, in the ETCD Corner article in the Spring issue of Outlook we posed a similar question to several members of SBM’s consultation program, and these are some of the quotes that they provided:
- “Do a few things well”
- “Get a good mentor and nurture that relationship”
- "Take a deep breath" - this is a paraphrase of an experience I had with my graduate advisor after I went to her in a panic about a dissertation data collection issue. Challenges are common in academia and it's important to remember to take a deep breath and focus rather than constantly react from event to event
- "Breathe and persist" — keeping calm and carrying on are the keys to maintaining your momentum in your career
- “Do what you love to do with people that you enjoy working alongside.” Both parts of the advice are valuable since working with a great team inspires so much more creativity in the area that you are passionate about and can make you excited to go into work every day.
How do you establish independence as a very early-career researcher (e.g., postdoc) while working primarily on projects and datasets that you do not own?
- I would suggest getting mentorship on writing your own grant. I got my start with a K award and it was invaluable for making that transition. Small seed grants can be useful too. Any independent researcher will need their own funding. Getting mentorship on grant writing is a must for a post doc if you want to have an independently funded research career. It may be the last opportunity to get intense mentorship on this skill.
- It is indeed very common to be working on projects and data sets that you do not own when you are early in your career, and it is helpful to work with your mentor to identify a unique research question that you can ask and answer with secondary data that will provide pilot data for your own grants that will fund you to pursue this independent area of research. Another opportunity is to compete for a small seed grant to add on a key measure to an existing project that would allow you to obtain critical pilot data. One mechanism for this is to apply for an SBM Distinguished Student Award for Excellence in Research.
Thank you to SBM President Sherry Pagoto and the ETCD Council for their answers to Outlook readers’ questions.
-- William J. Sieber, PhD
President's Message: Let's Chat
Sherry Pagoto, PhD, SBM President
 Sherry Pagoto, PhD
Sherry Pagoto, PhD
SBM President
As part of my presidential theme Leading the Narrative I launched a series of Twitter chats on emerging topics in behavioral medicine. If you are new to the concept of a Twitter chat, it refers to a scheduled public conversation on Twitter that lasts for one hour. Each chat has a topic that is framed around 5 questions. The 5 questions are released in tweets one at a time, spaced out by several minutes to allow time for each to be discussed. A hashtag (#behavioralmedchat) is used in all chat tweets so that participants can view all the chat tweets in chronological order in a newsfeed. Anyone with a Twitter account can participate by responding to the chat questions or by commenting on other participant’s responses. I host the chats and invite a special guest each month to share their wisdom on the topic.
We have held 4 chats so far on topics including health policy advocacy, social determinants of health, advancing obesity research, and social media for science communication. Click the links for transcripts of each chat. Our guests have included a cancer advocate, an emergency room doctor, an obesity doctor, and a dean of public health. Collectively, these chats have attracted 450 participants and content has reached nearly 13 million Twitter accounts.
To extend our reach and avoid producing an echo chamber, I typically invite to each chat an expert guest that is not a member of SBM since they can bring us a unique perspective and a unique audience. This leads to interesting connections. In one of our chats, an organization called Prevent Cancer participated, learned of SBM, and reached out to partner with us. In another chat, we were able to gather ideas from leaders in other professional organizations to inform how we can better engage patient voices in our annual meeting. If you participated in a chat and it led to a research collaboration, idea, or some other outcome, I’d love to hear about it!
Twitter chats are great for professional networking, idea generation, to hear new perspectives, to share our science with new audiences, and to discuss an issue in a forum with a diverse set of voices. Chat participants have included SBM members, nonprofit organizations, physicians and other healthcare professionals from a wide range of specialties, industry professionals, and members of the public. It is rare to get a chance, for example, to discuss how to move the science of obesity forward with all these voices at the table. Social media gives us this opportunity.
To get the most out of the chats, I recommend reviewing the 5 questions in advance and drafting up some responses, including links to your relevant work, so that you are ready to go when the chat starts. By pre-planning your responses, you will have more time to interact during the chat. All Twitter chat questions are posted here. Be sure to check back frequently as new chats will be appearing in the coming months.
Our upcoming chats will cover topics such as immigrant health, open science, social media research ethics, data visualization, and more! If you have an idea for a chat topic, please share it with me. If you would like to participate or learn more about the nuts and bolts of participation, check out the instructions at this link or watch this video. If the only barrier to participating is uncertainty on how to participate, reach out and I can help! I hope to be chatting with you soon.
Board Notes – Translating Research to Policy
Margaret Schneider, PhD, Society of Behavioral Medicine (SBM) Member delegate
 Margaret Schneider, PhD
Margaret Schneider, PhD
The theme for the SBM Annual Meeting 2019 is Leading the Narrative, and the SBM Board has been working to do just that by leveraging our members’ research, expertise, and reputation to influence not just health care practice but also policy. Thus far in 2018, SBM has released four Policy Briefs: 1) Retain School Meal Standards and Healthy School Lunches (link), 2) Support Oral Cancer Early-Detection Examinations (link), 3) Help Address the Opioid Crisis by Increasing Funding for Medication-Assisted-Treatment (link) and 4) Retain and Enhance Efforts to Increase Broadband Internet Availability for Health Care Access in Rural Areas (link). Under the direction of Chair Joanna Buscemi, the SBM Health Policy Committee guides members through the process of creating these brief, targeted and impact-oriented missives, which aim to inform and influence policymakers about the critical impact that behavior has on health and concrete steps that they can take to impact population health. For example, here are the recommendations from the Statement on the Opioid Crisis:
RECOMMENDATIONS
- Policymakers Must Increase the Availability of and Insurance Coverage for the Behavioral Component of Medication-Assisted-Treatment for Opioid Use Disorders
- Increase Medicaid funding so individuals can receive treatment when they need it but can’t afford it.
- Declare the opioid epidemic a national emergency and not just a public health emergency. This would provide immediate access to billions of dollars in federal monies for treatment programs.
If you have an idea for a Policy Brief, please reach out to Joanna at jbuscem2@depaul.edu.
In addition to the Policy Briefs, the SBM Board also regularly voices support in favor of or in opposition to specific public policies by releasing or signing on to position statements, often in response to issues prominent in the news. In June of this year, we signed on to a letter drafted by the Children’s Defense Fund, opposing the U.S. Immigration policy of forcibly separating children from parents among migrant, refugee, and asylum-seeking families.
Recognizing the power inherent in linking our voices to like-minded organizations, the SBM Board also recently voted to join a Coalition of Behavioral Science Organizations (CBSO) that aligns with our society’s mission. SBM has joined five other behavioral science organizations to advance society’s use of behavioral science knowledge and methods. In addition to SBM, the coalition includes the Association for Behavioral Analysis International, the Association for Contextual Behavior Science, the Association for Positive Behavior Support, the Evolution Institute, and the National Prevention Science Coalition. The coalition has developed a joint value statement that is directly relevant to SBM’s mission to foster nurturance and well-being in families, individuals, communities, and populations. SBM members are encouraged to review this shared value statement and direct questions or comments to SBM’s coalition representative and Past-President Dawn K. Wilson, PhD.
If you are looking for an even more immediate way to engage with other behavioral scientists and share your thoughts and opinions, consider participating in the new Twitter Chats hosted by SBM President Sherry Pagoto. In August, Dr. Esther Choo, an emergency room physician at Oregon Health and Sciences University, joined Dr. Pagoto in moderating a Twitter Chat on “How Academics Can Use Social Media to Advocate for Science and Policy”. To see information from prior Twitter Chats or to view future topics, click here. If you are looking for ways to translate your research to policy, SBM is ready to help!
Emerging Strategies for Promoting Health Decision Making
Alexander Young M.A. & Randi M. Williams, MPH, Health Decision Making SIG
There are many types of health decisions that one may consider ‘easy’ such as allowing blood pressure to be taken; however, other medical decisions like cancer screenings or developing a plan for managing type 2 diabetes may be more challenging. The many choices providers and patients navigate can often be difficult. So how do patients and providers navigate health decisions in a comprehensive manner while supporting a ‘good medical decision’?
Health Decision Strategies
There are many strategies for health decision promotion depending on the type of decision and the setting in which the decision is made. In general, health decisions should be made with a specific goal in mind. An example of this might be taking blood pressure medication to reduce blood pressure and stroke risk. When goals are present it allows the patient to see the end goal in a way that may be motivating and provide a better understanding of why the decision is important. One strategy to use, especially for serious health decisions may be the shared decision-making model or SDM. This type of approach allows a meaningful interaction between provider and patient. SDM has been shown to assist disadvantaged groups in making informed health decisions when their content is tailored and written in an easy and plain language. One way to enhance SDM is through the use of decision aids. Other techniques such as motivational can be used to complement SDM for promoting optimal, patient-centered care.
Patient Decision Aids
Decision aids are helpful at providing patients with information about treatment or screening options, as well as the potential risks, benefits, and costs associated with each option. We often find these decision aids in our primary care provider’s or specialist’ office during a visit or online, but how often do we pay attention to the design, color, and overall construction of these aids? Color and message framing are important factors in the construction of decision aids. Patient decision aids allow for more informed choices when it comes to making health decisions in conjunction with physician information. Patients are not always aware they have a voice regarding healthcare and that health choices are ultimately in the hands of the patient.
Health Decisions in Primary Care
There are many uses of SDM and the integration of decision aids. A model of applying health decision aids in primary care has been developed to increase their effectiveness and potential action in the primary care setting. The use of decision aids with an SDM model may be advantageous in the primary care setting as many treatment options are discussed in this context including medication management, cancer screening, specialty care for chronic conditions like diabetes, and behavioral health consultant services.
Other strategies to support decision making include use of patient navigators and decision coaches, values clarification methods, and interprofessional collaborations. For more information about health decision making, visit the Health Decision Making SIG page.
Integrating Health Policy Curriculum into the Classroom: An interview with Dr. Amber Emanuel
SBM’s Health Policy Committee
 Amber Emanuel, PhD
Amber Emanuel, PhD
A significant limitation of behavioral science training is that few programs offer dedicated coursework in the training of health policy, advocacy, and research to policy translation. The Health Policy Committee (HPC) is pleased to introduce Dr. Amber Emanuel who is a Lecturer in the Department of Health Education and Behavior at the University of Florida. Dr. Emanuel teaches a Community Health course for undergraduate students. Over the past 2 years, she has successfully incorporated health policy curriculum into this course. We recently spoke with her about her experience teaching health policy and advocacy approaches to her students.
What made you initially interested in adding policy training to your course?
My course already mentioned different health policies but it felt disjointed and students largely didn’t seem interested. At the SBM conference in 2017, I attended a symposium about policy and realized that I could do better at integrating and teaching my students about why policy matters and how to advocate for evidence-based health policies.
What policy training have you integrated into your course syllabus?
Now, I teach more policies throughout the semester to provide students with examples of existing or possible policies. We spend a week specifically talking about the details of writing policy briefs and how to advocate for health policies at different levels of government. Then, for part of their final project, students craft a policy brief and related infographic.
What were your students’ reactions to this training?
Students seem to like crafting the policy brief specifically because they can see how health research & advocating for a specific health policy can have a large impact. I hear a lot of “I can’t believe this isn’t a policy already!” which helps students to see how much of our existing health knowledge and research isn’t getting translated into policies. Also, the policy briefs and infographics themselves are substantive but stylish—we follow SBM’s formatting of their policy briefs (place link her to example/document?)---and students feel proud of how professional the final product is.
What are some examples of policy topics have that your students tackled?
They’ve been varied: implementing Traffic Light Nutrition labels nationwide, requiring a sexual education module for first year college students, allocating more funding for the mental health counseling center at our university, requiring elementary schools to teach about skin cancer and sunscreen, changing the texting while driving law to make it a primary enforcement violation, and funding school-based mindfulness programs.
Why do you think it is important to integrate policy advocacy into your courses?
It should be viewed as another skill set, just like statistical training. Advocacy requires skills—writing for a general audience, interacting with political leaders—and these skills are beneficial for all students.
What advice do you have for other professors/training programs in terms of how to restructure training to incorporate health policy topics into curriculum?
At either the graduate or undergraduate level, I would first suggest an entire semester-long seminar course on policy. If that’s not possible, start adding an additional policy question into existing assignments. We often ask students to think of individual-level interventions, but then also ask them to generate a realistic policy. To be able to generate a policy, students are demonstrating a deeper, multi-level understanding of the topic—a plus for both professors and students.
Opportunities Abound for SBM Members to Lead Integration Efforts Directed at Multi-Morbidities
Jerry M. Suls, PhD, Multi-Morbidities SIG Co-Chair
The Multi-Morbidities SIG was established to recognize and facilitate research, intervention and policy to face the challenge posed by the increasing prevalence of patients with multiple health conditions. Behavioral medicine has a significant role in advancing understanding of the biological and psychosocial pathways leading to multimorbidity, the contribution of positive and negative health behaviors, and to develop and test interventions for patients with multiple health conditions. Our hope is that SBM members and other SIG’s will consider efforts to collaborate to confront this tremendous challenge to public health. The question of multimorbidity touches on virtually all of the SIG’s, such as Cancer, Multiple Health Behavior Change, Aging, Women’s Health, Integrated Primary Care, Health Decision Making, Evidence-Based Behavioral Medicine, etc.
In some ways, European medical and behavioral medicine researchers and practitioners are ahead of US efforts. Earlier this year, three articles in Health Policy reported the findings of two European consortia established to help meet the needs of patients with multimorbidity. The findings of these European research consortia can provide insights to other health care systems that also are coping with the increasing numbers of patients with multiple medical conditions.
One of the consortia is the SELFIE research project (Sustainable intEgrated chronic care modeLs for multimorbidity delivery, FInancing and performancE), which strives to improve person-centered care for persons with multimorbidity. The Netherlands, Austria, Croatia, Germany, Hungary, Norway, Spain, and the UK make-up the consortium.
In a scoping review conducted by SELFIE, Struckmann et al. identified several integrated health programs in Europe (n =11) and the US (n =5).1 The majority adopted the Wagner Chronic Care Model or the Guided Care Model although the authors observed that neither model actually focuses on patients with multiple chronic conditions. SELFIE’s “take-home message” was the need to shift from disease-centered care to person-centered care. An element of the latter is the use of holistic assessment, which ascertains patient’s needs and preferences to determine which type of care is needed followed by prioritization of health problems where person preferences are taken into account. The review observes that the use of multidisciplinary team, that includes psychologists, is recommended. Other essential components of interdisciplinary care are self-management and use of an electronic information system.
A second SELFIE effort identified concepts for integrated care for multimorbidity. A framework is presented that encompasses micro, meso and macro levels and groups concepts into six key components, adapted from the World Health Organization’s key components of health systems: leadership and governance, health information systems, health financing, human resources for health, essential medical products and technologies, and service delivery.2
The other European consortium, ICARE4EU, seeks to increase and disseminate knowledge of European integrated care program addressing multimorbidity. Rijken et al. identified described and characterized innovative care practices for patients with multiple medical conditions in 24 countries.3 They found that practices that focus on a specific disease or a combination of specific diseases exhibit less integration in type, breadth and integration than practices that focus on any combination of diseases. Furthermore, those that focus on any disease combinations involve more disciplines (e.g., community nurses, psychologists, physiotherapists, etc.) that work in the same primary care practice as the general practitioners. These results reinforce the idea that the patient medical home concept works best when all the relevant health care professionals work in the same space rather than at a distance or only at specific times. Integrated Primary Care started by emphasizing the important role for health care psychologists in serving the mental health and substance use needs of patients. The two European consortia reinforce the idea that that psychologists in primary care also can make useful contributions with respect to multiple psychological and physical conditions and bridge the vertical silo’s created by specialty care.
We urge SBM members to think about how their area of concentration touches on the multimorbidity challenge and how their SIG can engage in meaningful ways with other SIGs. It is time for SBM members to reach out within the society, and also at the national and international level to establish consortia to assess guidelines and care policies for persons at risk or living with multiple health conditions.
References
- Strickmanm, V., Leijten, F., van Ginnekin, E., Kraus, M., Reiss, M., Spanger, A. ...(2018). Relevant models and elements of integrated care for multi-morbidity: Results of a scoping review. Health Policy, 122, 23-35.
- Leijten, R.M., Struckman, V., van Ginnekin, E., Czypionka, T., Kraus, M., Reiss, M…. (2018). The SELFIE framework for integrated care for multi-morbidity, Health Affairs, 122, 12-22.
- Rijken, M., Hujala, A., van Ginneken, E., Melchiorre, M.G., Groenewegen, P., & Schellevis, F. (2018). Managing multimorbidity: Profiles of integrated care approaches targeting people with multiple chronic conditions in Europe. Health Policy, 122, 44-52.
Career Mentorship Streamed Live to Your Laptop – SBM's Training and Career Development Webinar Series
Education, Training, and Career Development (ETCD) Council Corner
Amy G. Huebschmann, MD, MS (ETCD Council chair), Sydney G. O’Connor (Student Special Interest Group (SIG) Mentorship and Training Coordinator), Jocelyn E. Remmert, MS (Student SIG Chair), and Morgan S. Lee, PhD, MPH, CPH (Liaison between ETCD Council and Student SIG)
Welcome to the “ETCD Council corner” of Outlook! In each issue of Outlook, look to the ETCD Council corner for information related to our mission, which is to provide SBM members with opportunities and support to enhance their training and career development throughout all phases of their careers in behavioral medicine.
There is a new career development opportunity for SBM members that we want to share with you. The SBM Student SIG and the Education, Training and Career Development Council (ETCD) have developed a series of six career-development webinars in partnership with several special interest groups: Health Equity, Cancer, Physical Activity, Obesity and Eating Disorders, and Pain.
The objective of this series is to foster opportunities to discuss and promote effective training, mentorship, and career development for students, postdocs, and early career professionals. We worked with SIGs to design webinars to address topics that our members have identified as high-priority career development areas, such as career transitions, developing competitive grants, and opportunities to develop leadership skills. We asked SIGs to consider targeting members at a specific career stage, and we sought to include an array of topics for a broad range of learners: current graduate students, post-docs, early faculty, and mid-career faculty. Below are the topics and dates. Mark your calendar now, and keep an eye out for upcoming emails regarding registration!
| Webinar Date |
Hosting SIG |
Topic |
| 9/20/18 |
Health Equity |
Transition from Postdoc to Junior Faculty |
| 10/18/18 |
Health Decision Making |
How to Create a Mentorship Team |
| 10/25/18 |
Cancer |
Choosing the Right Postdoc |
| 11/29/18 |
Physical Activity |
Navigating Mid-Career Transitions |
| 1/10/19 |
Obesity and Eating Disorders |
How to Write a Successful Specific Aims Page |
| 3/21/19 |
Pain |
Leadership Skills for Psychologists |
Please note that all webinars are on Thursdays, at 1.p.m. ET/12 p.m. CT/11 a.m. MT/10 a.m. PT. These webinars are part of the ongoing SBM Behavior Change Grand Rounds series—you can view the upcoming schedule for other webinars here: https://www.sbm.org/training/webinars
We look forward to the valuable information in these webinars and hope you’ll join us! The ETCD Council plans to continue to collaborate with the Student SIG to offer panel discussions on topics relevant to students at SBM 2019 and in future years. We welcome input from students and other early-career members regarding the types of topics we should address. Please e-mail Andrew Schmidt at aschmidt@sbm.org if you have a suggestion for us.
OBBI SIG Interview: Sara Hoffman Shares Her Takeaways from a NIH Optimization Training Course
Sara M. St. George, PhD, Optimization of Behavioral and Biobehavioral Interventions SIG Co-Chair
 Sara Hoffman, MS
Sara Hoffman, MS
The Society of Behavioral Medicine’s (SBM) Optimization of Behavioral and Biobehavioral Interventions Special Interest Group (OBBI SIG) recently interviewed Sara Hoffman, MS, clinical psychology doctoral candidate at Northwestern University Feinberg School of Medicine. Ms. Hoffman attended a five-day training in May 2018 sponsored by the Office of Behavioral and Social Science Research (OBSSR) and National Institute on Drug Abuse (NIDA) on optimization of behavioral and biobehavioral interventions.
![[The flow chart begins with an information input/output box; the list inside reads: “Theory. Scientific literature. Clinical experience. Data analysis results. Other.†Then proceed to an action box with Step 1 “Establishment of theoretical model.†Next is an action box: Step 2 “Identification of set of intervention components to be examined.†Next is an action box: Step 3A “Experimentation to examine individual intervention components. Step 3A leads to Step 3B. An alternate path leads to the information input/output box “Centralized database.†The information input/output box “Centralized database†is outside of the main steps of the flow chart. The information input/output box “Centralized database†in turn leads to an action box also outside of the main flow chart steps. The action box reads “Exploratory data analyses.†The arrow from this action box returns to the very beginning of the chart with the information input/output box: “Theory. Scientific literature. Clinical experience. Data analysis results. Other.†From Step 3A, proceed to Step 3B, the action box “Refinement via experimentations and other methods.†This action is optional. Step 3B is followed by Step 4. Step 3B also has an alternate path to the information input/output box “Centralized database.†Step 4 is an action box “Assembly of beta intervention.†Step 4 leads to a decision point: “Is beta intervention expected to be effective?â€. If the answer is no, then return to Step 1 “Establishment of theoretical model.†If the answer is yes, then proceed to Step 5. Step 5 is an action box “Confirmation of effectiveness of beta intervention via RCT [randomized controlled trial]â€. Step 5 has two arrows. One leads to the information input/output box “Centralized database.†The other arrow from Step 5 leads to a decision point: “Is beta intervention effective?â€. If the answer to this question is no, then return to Step 1 “Establishment of theoretical model.†If the answer is yes, proceed to Step 6. Step 6 is a product “Release of new intervention.†This is the end of the flow chart.]](http://www.sbm.org/UserFiles/image/fall2018_most-figure.jpg) What were some of the most memorable things you learned or gained from attending the training?
What were some of the most memorable things you learned or gained from attending the training?
The importance of conceptual models and how these function within the preparation phase of the multiphase optimization strategy (MOST; see Figure 1). We did group work throughout the week, developing a conceptual model for a possible intervention, and this was the most challenging but beneficial aspect of training for me. We also had access to Linda Collins’s new book (available now through Springer!), which was a great resource and something I use to guide decision-making. Importantly, I gained a network of potential collaborators from across the world who are similarly passionate about optimized interventions. I can’t say enough about the quality of this training.
What were common questions or misconceptions about optimization that came up during the training?
Specific to factorial experiments in the MOST optimization phase, many questions involved breaking down the analysis and re-framing the discussion of results as not examining experimental conditions (as in RCTs), but rather investigating the effects of components across all conditions. One of the best parts of our question-and-answer time was that everyone bought in to MOST principles, allowing more time for questions about the actual implementation of optimization designs in the ‘real world.’ It was so cool to see a group of people excited about this way of thinking, and wondering how they could apply these principles in their own labs! Also, something Dr. Almirall said was so important that I had to tweet about it, since it’s a common misconception: there is no such thing as a “MOST design” - MOST is a framework or way of thinking.
How do you plan on applying the concepts you learned to your own current or future work?
My mentor, Bonnie Spring, and Linda Collins recently finished a clinical trial to develop a technology-supported weight loss intervention using a full factorial optimization design within MOST. This training was essential in solidifying my understanding of the decision-making process to transition from the optimization phase to the evaluation phase of MOST. My dissertation will also use data from this study to examine the role of demographic similarity between our participants and their support “Buddies” on weight loss success. As a future clinical health psychologist/behavioral scientist focused on the social influences on health behavior change, I will inevitably use the MOST framework to understand how particular components of social support contribute to an individual’s success in making health changes.
For background information on optimization of behavioral and biobehavioral interventions, visit The Penn State Methodology Center.
Efficiency in Interdisciplinary Chronic Pain Management: A Trans-Disciplinary Model for Integrated Care Plans
Kelly M. Wawrzyniak, PsyD, Director of Behavioral Medicine and Clinical Research Development, Boston PainCare, Waltham, MA
SBM Pain SIG member
I have been fortunate to work at a chronic pain center incepted a decade ago by six anesthesiologists on a mission to create an interdisciplinary pain center that is financially sustainable and approaches pain management differently. While interventional procedures continue to be the most profitable service, these go directly to paying for full time behavioral medicine and functional restoration staff that are historically operating at a financial loss to the employer. Keys to sustaining this model are the efficiency of clinician time and treatments, and having coordinated and integrated care across disciplines.
To this end, the medical director at Boston PainCare, David DiBenedetto, MD, has outlined the “GOTT” approach–an acronym for goals, obstacles, treatments, timeline. These terms are not new to the behavioral medicine clinician, and commonly discussed when using a Cognitive-Behavioral approach to psychotherapy. The order of these terms is crucial, such that we begin not with the patient’s symptom complaints, but rather with identifying realistic, objective goals of treatment (e.g., walk a mile, return to work 2 days/week). These are essentially SMART goals (i.e., specific, meaningful, adaptive, realistic, time-bound) and are generated through each clinician discussing goals with the patient in each evaluation. We then discuss the obstacles to the patient meeting their goals at this time (e.g. pain, depression). We next identify treatments that will effectively target the obstacles and, finally, identify a timeline for which we will re-evaluate progress and discuss any revision to the care plan. Of course not all patients with chronic pain are interested in a functional goal-focused approach to their care, some preferring a pain palliation focus. However, explicitly outlining this approach with patients at the outset allows for more open discussion to invite patients to try a new approach after perhaps decades of medical care focused on pain reduction.
Figure 1. GOTT Approach to Developing a Plan of Care for Patients with Chronic Pain
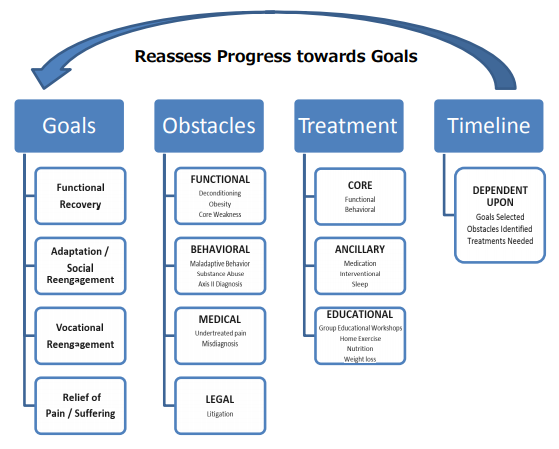
The GOTT framework leads to efficiency in a few ways. First, it focuses each clinician’s evaluation and clinical interview. Second, team meetings have more efficient and focused discussion. Third, it re-focuses treatment recommendations on functional goals as the outcomes, rather than only symptom reduction. Fourth, GOTT framework is discussed with patients, leading to clear expectations and timelines at the outset, and more engagement with them in evaluating the effectiveness of treatment. Last, this approach is reflected in the medical records with functional goals stated front and center on the chart summary page, right alongside other top-line information (e.g., allergies, controlled medications). This placement is a poignant reminder of the philosophy of care and the focus of the clinical work. During case reviews or re-evaluations this display will often prompt the clinicians to ask "are the current treatments meeting these goals?" and "are these goals still meaningful and realistic?" Although each clinician’s treatment plan is different in terms of the specific sub-goals and interventions, all disciplines should be working toward the overarching functional goals for that patient.
Ultimately, the efficiencies of this model have proven beneficial in cost containment at our center, a topic especially relevant with the shift away from fee for service payment models to ACOs and value-based care. The GOTT model has been effective at providing a more efficient use of the increased time and resources required when providing integrated, interdisciplinary care for chronic pain. This model is one that may easily apply to integrated care teams across settings (e.g., academic hospitals, Veterans Administration clinics) and across clinical conditions (e.g., diabetes, cardiac conditions). This may also be a model that facilitates a multi-disciplinary team move toward an integrated, interdisciplinary team through both the shared framework and the efficiencies that allow for increased time collaborating across providers.
SBM Award Winner Will Help Children Affected by Puerto Rico Hurricane
 Freddie Pastrana Rivera
Freddie Pastrana Rivera
The Society of Behavioral Medicine (SBM) is proud to announce its winner of the 2018 Health and Behavior International Collaborative Award: SBM member Mr. Freddie Pastrana Rivera!
Mr. Pastrana Rivera is currently a psychology intern at the Medical University of South Carolina (MUSC), and he plans to use the award during his postdoctoral fellowship year at MUSC to enhance his skills in innovative, field-based trauma research, while also training for multidisciplinary collaborative partnerships with health professionals in Puerto Rico, and providing school-based training to underserved, Spanish-speaking communities.
Mr. Pastrana Rivera plans to accomplish these goals by helping those affected by Hurricane Maria, which devastated the nation of Puerto Rico after making landfall on September 20, 2017. The hurricane left millions of citizens without access to power, clean water, or reliable communication for months. More recently, school-based health personnel on the island have reported significant concerns about the mental health of Puerto Rican youth. This is alarming, considering that for a number of children, exposure to such a catastrophic event can increase the risk for mental health, behavioral, and somatic problems.
With the $3,000 award, Mr. Pastrana Rivera will partner with a faculty mentor in Puerto Rico and provide training to local health personnel by teaching them how to identify trauma-related symptoms in students, as well as how to refer them to appropriate evidence-based mental health services. With Mr. Pastrana Rivera’s help, hopefully the children of Puerto Rico will get the personalized mental health care they need and deserve.
Well done, Mr. Pastrana Rivera!
The Health and Behavior International Collaborative Award is jointly sponsored by SBM, the International Society of Behavioral Medicine (ISBM), the Society for Health Psychology (SfHP), and the American Psychosomatic Society (APS). Each organization officially sponsors one award winner. Applicants are limited to trainees and early-career professionals, who use the award to visit to an international laboratory or research group where they will pursue a specific program development project in the areas of health research, clinical behavioral health, behavioral medicine, or health promotion.
Congratulations to all the other Health and Behavior International Collaborative Award winners:
- SBM member Joshua Wiley, PhD of Monash University Australia (APS winner)
- SBM member Fabiana Brito Silva, PhD, MS, BSN of the University of Nebraska Medical Center (ISBM winner)
- SBM member Jessica Latack, PhD of Weill Cornell Medical Center/New York Presbyterian Hospital (SfhP winner).
Look for applications for the 2019 award next spring!
Trauma, violence, and health: Why We Formed the Violence and Trauma SIG
Sheela Raja, PhD; Elissa Lee, OTS; Pamela Behrman, PhD; and Rose Constantino, PhD, MN, JD
Violence, Trauma, and Toxic Stress are Common. As illustrated by the following statistics, violence and trauma are extremely prevalent in the United States. Approximately one in five women report a history of adult sexual trauma.1 One in four girls and one in twenty boys experience childhood sexual abuse2 and five children die from child abuse-related injuries every day.3 One of four women and one in seven men have experienced severe physical violence in an intimate relationship.4 Approximately one in ten seniors report elder abuse in the form of sexual, emotional, or physical abuse, or financial control.5 Seven percent of the population has been exposed to combat in a war zone, either as a part of military service or as a refugee/immigrant.6 Finally, the Centers for Disease Control estimate that approximately 12,000 Americans die by firearm related homicides a year, and an additional 24,000 die from firearm related suicides. From the epidemic gun violence (e.g., mass shootings, daily community violence, and police-involved shootings), the #MeToo movement, and the forced separation of refugee families seeking asylum, trauma is in our news and in our culture.
Trauma Influences Mental Health, Physiology, and Behavioral Coping. Because many traumatic events involve violation of a person’s bodily integrity, they often have adverse influences on physical and mental health7,8 and attitudes toward medical care.9,10,11,12 The Adverse Childhood Events (ACE) study was a landmark project in trauma-informed care that documented the relationship between self-reported childhood trauma (e.g., child abuse, neglect, parental separation, and parental mental illness and substance abuse) and adult health.13 In addition to mental health and substance use, ACEs are related to our physical health. For example, people who experience more ACEs are at an increased risk of heart disease and liver disease. Further, six or more ACEs are related to up to twenty-year reductions in life expectancy.14 This may be due in part to the fact that repeated trauma and violence can change our physiology and influence the way we cope (e.g., smoking, overeating, substance use, or sexual risk taking). Compared to non-traumatized individuals, trauma survivors may report more sick and emergency room visits, but they may actually avoid seeking preventive medical care such as mammograms, cervical cancer screenings, and even dental cleanings.15,16,17,18 Survivors may feel anxious or “re-triggered” during these appointments.
Behavioral Interventions Need to Address Trauma and Support Resilience. The good news is that many people are able to live healthy, fulfilling lives, even after experiencing very difficult life events. One key finding is that social networks play a key role in healing—these networks can be a combination of friends, family, and professionals. No one heals alone. Behavioral interventions need to be designed to assess trauma, violence, and toxic stress. In addition, patients who do not respond to simple interventions may need more tailored, intensive interventions, where their trauma history is addressed. Trauma informed interventions can help people live healthy and meaningful lives.
The Violence and Trauma SIG has been active in many aspects of SBM. SIG members have contributed to SBM position statements opposing the forced separation of families at the US border and urging the restoration of CDC funding to study gun violence prevention. The SIG has also presented several sessions at SBM meetings on trauma-informed health, the neurobiology of stress, and the role of adverse childhood experiences on health. SIG members are actively collaborating on papers and projects focused on several topics, including how trauma influences opioid addiction, how racism and toxic stress influence health, how healthcare providers can accurately assess for a history of violence and trauma, and how behavioral medicine interventions can become more trauma-informed. The Violence and Trauma SIG welcomes your ideas!
References
- Black, M.C., Basile, K.C., Breiding, M.J., Smith, S.G., Walters, M.L., Merrick, M.T., Chen, J., & Stevens, M.R. (2011). The National Intimate Partner and Sexual Violence Survey (NISVS): 2010 Summary Report. Atlanta, GA: National Center for Injury Prevention and Control, Centers for Disease Control and Prevention.
- Finkelhor, D., Shattuck, A., Turner, H. A., & Hamby, S. L. (2014). The Lifetime Prevalence of Child Sexual Abuse and Sexual Assault Assessed in Late Adolescence. Journal of Adolescent Health, 55(3), 329-333. doi:10.1016/j.jadohealth.2013.12.026
- U.S. Department of Health and Human Services, Administration for Children and Families, Administration on Children, Youth and Families, Children’s Bureau. (2011). Child maltreatment 2010. Available from http://www.acf.hhs.gov/programs/cb/stats_research/index.htm#can
- Black, M.C., Basile, K.C., Breiding, M.J., Smith, S.G., Walters, M.L., Merrick, M.T., Chen, J., & Stevens, M.R. (2011). The National Intimate Partner and Sexual Violence Survey (NISVS): 2010 Summary Report. Atlanta, GA: National Center for Injury Prevention and Control, Centers for Disease Control and Prevention
- Hernandez, M., Acierno, R., & Muzzy, W. (2009). Race and Ethnicity Findings: The National Elder Mistreatment Study. PsycEXTRA Dataset. doi:10.1037/e517292011-482
- Kilpatrick, D. G., Resnick, H. S., Milanak, M. E., Miller, M. W., Keyes, K. M., & Friedman, M. J. (2013). National Estimates of Exposure to Traumatic Events and PTSD Prevalence UsingDSM-IVandDSM-5Criteria. Journal of Traumatic Stress, 26(5), 537-547. doi:10.1002/jts.21848
- Havig, K. (2008). The Health Care Experiences of Adult Survivors of Child Sexual Abuse. Trauma, Violence, & Abuse, 9(1), 19-33. doi:10.1177/1524838007309805
- Thoits, P. A. (2010). Stress and Health: Major Findings and Policy Implications. Journal of Health and Social Behavior, 51(1_suppl). doi:10.1177/0022146510383499
- Morse, D. S., Lafleur, R., Fogarty, C. T., Mittal, M., & Cerulli, C. (2012). "They Told Me To Leave": How Health Care Providers Address Intimate Partner Violence. The Journal of the American Board of Family Medicine, 25(3), 333-342. doi:10.3122/jabfm.2012.03.110193
- Ullman, S. E. (2010). Talking about sexual assault: Society’s response to survivors. Washington, DC: American Psychological Association.
- Spelman, J. F., Hunt, S. C., Seal, K. H., & Burgo-Black, A. L. (2012). Post Deployment Care for Returning Combat Veterans. Journal of General Internal Medicine, 27(9), 1200-1209. doi:10.1007/s11606-012-2061-1
- Jeffreys, M. R. (2016). Teaching cultural competence in nursing and health care: Inquiry, action, and innovation. New York: Springer Publishing Company.
- Felitti V.J, Anda, R.F., Nordenberg, D., Williamson, D.F., Spitz, A.M., Edwards V., Koss, M.P., et al. (1998). The Relationship of Adult Health Status to Childhood Abuse and Household Dysfunction. American Journal of Preventive Medicine, 14: 245-258.
- Brown, D.W., Anda, R.A., Tiemeier, H., Felitti, V.J., Edwards, V.J., Croft, J.B., Giles, W.H. (2009). Adverse Childhood Experiences and the Risk of Premature Mortality. American Journal of Preventive Medicine, 37: 389-396.
- Farley M., Golding J.M., Minkoff J.R. (2002). Is a history of trauma associated with a reduced likelihood of cervical cancer screening? Journal of Family Practice, 51(10):827-831.
- Farley, M., Minkoff, J. R., & Barkan, H. (2001). Breast Cancer Screening and Trauma History. Women & Health, 34(2), 15-27. doi:10.1300/j013v34n02_02
- Farley, M., & Patsalides, B. M. (2001). Physical Symptoms, Posttraumatic Stress Disorder, and Healthcare Utilization of Women with and without Childhood Physical and Sexual Abuse. Psychological Reports,89(3), 595-606. doi:10.2466/pr0.2001.89.3.595
- Leeners, B., Stiller, R., Block, E., Görres, G., Imthurn, B., & Rath, W. (2007). Consequences of childhood sexual abuse experiences on dental care. Journal of Psychosomatic Research, 62(5), 581-588. doi:10.1016/j.jpsychores.2006.11.009
Nominations Open Soon for 2019 SBM Achievement Awards
Each year, SBM provides awards recognizing outstanding achievement and contribution to the field of behavioral medicine. Nominations for awards must be submitted by current SBM members in good standing. Join SBM or renew your membership. With the exception of the Distinguished Mentor Award, self-nominations are accepted. Recipients will be presented with their awards during the 2019 SBM Annual Meeting & Scientific Sessions.
Awards applications and supporting materials will be accepted in October; a call for applications and submission deadline will be announced on the SBM website. Only those nominations submitted via the online form before the deadline will be considered. SBM has a strong institutional commitment to diversity in all areas and encourages candidates from underrepresented groups to submit applications.
The following awards will be offered in 2019:
- Distinguished Scientist Award
- Research to Practice Award
- Jessie Gruman Award for Health Engagement
- Early Career Investigator Award
- Outstanding Dissertation Award
- Distinguished Student Awards
- Distinguished Mentor Award
- Excellence in Behavioral Medicine Training Program Award
Visit the Achievement Awards webpage for more information.
New Articles from Annals of Behavioral Medicine and Translational Behavioral Medicine
SBM's two journals, Annals of Behavioral Medicine and Translational Behavioral Medicine: Practice, Policy, Research (TBM), continuously publish online articles, many of which become available before issues are printed. Three recently published Annals and TBM online articles are listed below.
SBM members who have paid their 2018 membership dues are able to access the full text of all Annals and TBM online articles via the SBM website by following the steps below.
- Go to the Members Only section of the SBM website.
- Log in with your username and password.
- Click on the Journals link.
- Click on the title of the journal which you would like to electronically access.
To check if you are a current SBM member, or if you are having trouble accessing the journals online, please contact the SBM national office at info@sbm.org or (414) 918-3156.
Annals of Behavioral Medicine
Tegan Cruwys, Juliet R H Wakefield, Fabio Sani, Genevieve A Dingle, Jolanda Jetten
Background
Frequent attenders in primary care have complex physical and mental healthcare needs as well as low satisfaction with their health care. Interventions targeting mental health or psychoeducation have not been effective in reducing attendance. Here, we test the proposition that both frequent attendance and poor health are partly explained by unmet social needs (i.e., limited social group support networks).
Methods
Study 1 (N = 1,752) was a large, cross-sectional community sample of primary care attenders in Scotland. Study 2 (N = 79) was a longitudinal study of a group of young people undergoing a life transition (moving countries and commencing university) that increased their risk of frequent attendance. Study 3 (N = 46) was a pre–post intervention study examining whether disadvantaged adults who joined a social group subsequently had reduced frequency of primary care attendance.
Results
All three studies found that low social group connectedness was associated with a higher frequency of primary care attendance. This was not attributable to poorer health among those who were socially isolated. In Study 3, joining a social group led to reduced primary care attendance to the extent that participants experienced a (subjective) increase in their social group connectedness.
Conclusions
Unmet social needs among frequent attenders warrant closer consideration. Interventions that target social group connectedness show promise for reducing overutilization of primary care services.
Jeffrey D Wardell, Paul A Shuper, Sean B Rourke, Christian S Hendershot
Background
HIV-related stigma is associated with health consequences among people living with HIV, including increased risk for alcohol problems. Theory suggests that maladaptive coping may mediate the relationship between HIV-related stigma and alcohol outcomes, and these variables may be bidirectionally associated over time. However, no studies have examined the temporal relationships among these variables in people living with HIV.
Purpose
This study examined prospective bidirectional and mediated associations among HIV-related stigma, maladaptive coping, and alcohol use severity in patients enrolled in the Ontario HIV Treatment Network Cohort study.
Method
Patients receiving care for HIV (N = 1,520) at one of several clinics completed self-report measures annually. Data were analyzed in a four-wave, cross-lagged panel model.
Results
Greater HIV-related stigma at each wave consistently predicted increased maladaptive coping 1 year later. Similarly, maladaptive coping consistently predicted greater subsequent HIV-related stigma. Further, we observed some evidence that maladaptive coping mediated the prospective associations between HIV-related stigma and alcohol use severity in both directions (i.e., stigma to subsequent alcohol use severity and vice versa) although these associations were not observed across all waves.
Conclusion
Results suggest that HIV-related stigma and maladaptive coping are bidirectionally associated with one another over time. This study also provides some evidence that coping may be a relevant mediator of these associations, although findings were less consistent for mediated pathways. Future research should examine whether interventions addressing stigma and coping among people living with HIV may help to minimize health risks such as hazardous drinking.
Colleen A Cuthbert, Kathryn M King-Shier, J Dean Ruether, Dianne M Tapp, Kathryn Wytsma-Fisher, Tak S Fung, Nicole Culos-Reed
Background
Family caregivers to cancer patients are at risk for physical and psychological morbidity as a direct result of being in the caregiver role. Exercise as an intervention to support caregiver health and well-being has been tested in other caregiver populations; however, no randomized controlled trials testing the effects of an aerobic and resistance training program have been conducted where cancer caregivers only have participated.
Purpose
To examine the effects of a 12-week exercise program on quality of life (Short Form 36 v2), psychological outcomes, physical activity levels, and physical fitness in caregivers to cancer patients.
Methods
Seventy-seven caregivers were randomized to either an exercise intervention or wait-list control. Two participants in the exercise arm dropped out immediately after their baseline assessment. Outcome data for n = 77 participants were analyzed using intention-to-treat analysis with linear mixed models.
Results
Significant group by time interaction effects were detected for exercise on the mental health component score of quality of life, self-reported weekly exercise levels, and the six-minute walk test. Small to medium effect sizes were detected on several outcomes including physical health component of quality of life (d = 0.36), mental health component of quality of life (d = 0.74), depression (d = 0.41), anxiety (d = 0.35), physical activity levels (d = 0.80), and the six-minute walk test (d = 0.21).
Conclusions
The findings suggest that exercise may improve health and well-being and could be considered as an additional type of support offered to cancer caregivers.
Translational Behavioral Medicine
Amber Werbrouck, Eva Swinnen, Eric Kerckhofs, Ronald Buyl, David Beckwée, Liesbet De Wit
Abstract
Patient empowerment, a concept focused on patient-centeredness and patients autonomy, is a well-discussed topic in health literature. However, translating theory into practice is a challenge. The purpose of this study was to assess the effectiveness of interventions on patient empowerment and to identify and compare the modalities of these interventions. For this systematic review including meta-analysis, eligibility criteria were as follows: (i) adult participants with one or more chronic somatic diseases, (ii) “patient empowerment” was explicitly measured (i.e., outcome or measuring instrument), (iii) randomized controlled designs, and (iv) written in English, French, Dutch, or German. A systematic search strategy was applied in five online databases (last search: March 29, 2017). Thirty-two studies were included in this review, of which 23 studies could be included in the meta-analysis. Overall effect estimate was significant in favor of the intervention; however, heterogeneity was high. Subgroup analyses revealed that the effect estimate was higher in studies with interventions that comprised individual sessions. The most recurrent behavioral change technique identified in our review was “knowledge”, though this is not sufficient to empower. “Goal setting” and “action planning” were more likely to be applied in successful interventions. “Knowledge” could be combined with “goal setting” and “action planning” to empower. Thorough understanding of the concept of patient empowerment remains necessary. Future research should focus on somatic chronic diseases other than diabetes, a consensus definition for patient empowerment, and clinimetric properties of instruments.
Jun Ma, Megan A Lewis, Joshua M Smyth
Abstract
In this commentary, we propose a vision for “practice-based translational behavior change research,” which we define as clinical and public health practice-embedded research on the implementation, optimization, and fundamental mechanisms of behavioral interventions. This vision intends to be inclusive of important research elements for behavioral intervention development, testing, and implementation. We discuss important research gaps and conceptual and methodological advances in three key areas along the discovery (development) to delivery (implementation) continuum of evidence-based interventions to improve behavior and health that could help achieve our vision of practice-based translational behavior change research. We expect our proposed vision to be refined and evolve over time. Through highlighting critical gaps that can be addressed by integrating modern theoretical and methodological approaches across disciplines in behavioral medicine, we hope to inspire the development and funding of innovative research on more potent and implementable behavior change interventions for optimal population and individual health.
Caroline M Angel, Blayne P Smith, John M Pinter, Brandon B Young, Nicholas J Armstrong, Joseph P Quinn, Daniel F Brostek, David E Goodrich, Katherine D Hoerster, Michael S Erwin
Abstract
Military service assimilates individuals into a socially cohesive force to address dangerous and traumatic situations that have no counterpart in civilian life. Upon leaving active duty, many veterans experience a “reverse culture shock” when trying to reintegrate into civilian institutions and cultivate supportive social networks. Poor social reintegration is associated with greater morbidity and premature mortality in part due to adoption of risky health behaviors, social isolation, and inadequate engagement in health care services. Although institutions like the Veterans Health Administration (VA) do much to address the complex psychosocial and health care needs of veterans and their families with evidence-based care, only 61% of Operations Enduring and Iraqi Freedom (OEF/OIF) Veterans are enrolled in VA care and there are numerous perceived barriers to care for enrollees. To address this gap, a community-based nonprofit organization, Team Red, White & Blue (RWB), was created to help veterans establish health-enriching social connections with communities through the consistent provision of inclusive and locally tailored physical, social, and service activities. This article provides an overview of the development and refinement of a theory-based framework for veteran health called the Enrichment Equation, comprised of three core constructs: health, people, and purpose. By operationalizing programming activities and roles, we describe how theoretical components were translated into a social networking implementation package that enabled rapid national spread of Team RWB. We conclude with future opportunities to partner with researchers and other organizations to understand program impact, and to identify effective intervention components that could be adapted for similar vulnerable groups.
Honors and Awards
Congratulations to the following Society of Behavioral Medicine (SBM) members who recently received awards or were otherwise honored. To have your honor or award featured in the next issue of Outlook, please email aschmidt@sbm.org.
Jill E. Bormann, PhD, RN, FAAN
Dr. Bormann was invited as a keynote speaker to Augustana University's Sigma Theta Tau Honor Society’s spring meeting.
Craig M. Jenkins, PhD
Dr. Jenkins recently accepted the Society of Military Psychology's Julius E. Uhlaner Award on behalf of the Office of the Command Psychologist, US Army Recruiting Command (USAREC).
Kevin S. Masters, PhD
Dr. Masters was recently awarded the Cynthia D. Belar Award for Excellence in Education and Training in Health Psychology from the Society for Health Psychology.
Serina A. Neumann, PhD
Dr. Neumann has been appointed to the newly-created position of Eastern Virginia Medical School Wellness Officer.
Amelie G. Ramirez, PhD
Dr. Ramirez has recently been named a Susan G. Komen Scholar and an "Icon in Healthcare" from CentroMed.
Members in the News
The following Society of Behavioral Medicine (SBM) members and their research were recently featured in news articles, videos, or journals. To have your news spot featured in the next issue of Outlook, please email aschmidt@sbm.org.
Jill E. Bormann, PhD, RN, FAAN
South Dakota Public Radio interviewed Dr. Bormann for their "In the Moment" series.
Susan D. Brown, PhD
Kaiser Permanente featured a profile of Dr. Brown in their research spotlight publication.
Lorraine Dean, ScD
Dr. Dean was featured in an article on HealthCare Analytics News on race and socioeconomic factors in breast cancer studies.
Katherine S. Hall, PhD
Dr. Hall is quoted in an AARP article on physical activity and changes in physical fitness across the lifespan.
Amanda E. Staiano, PhD, MPP
Dr. Staiano was featured in a WWL-TV story on Pennington Biomedical Research Center's PCORI grant-funded childhood obesity study.






![[The flow chart begins with an information input/output box; the list inside reads: “Theory. Scientific literature. Clinical experience. Data analysis results. Other.†Then proceed to an action box with Step 1 “Establishment of theoretical model.†Next is an action box: Step 2 “Identification of set of intervention components to be examined.†Next is an action box: Step 3A “Experimentation to examine individual intervention components. Step 3A leads to Step 3B. An alternate path leads to the information input/output box “Centralized database.†The information input/output box “Centralized database†is outside of the main steps of the flow chart. The information input/output box “Centralized database†in turn leads to an action box also outside of the main flow chart steps. The action box reads “Exploratory data analyses.†The arrow from this action box returns to the very beginning of the chart with the information input/output box: “Theory. Scientific literature. Clinical experience. Data analysis results. Other.†From Step 3A, proceed to Step 3B, the action box “Refinement via experimentations and other methods.†This action is optional. Step 3B is followed by Step 4. Step 3B also has an alternate path to the information input/output box “Centralized database.†Step 4 is an action box “Assembly of beta intervention.†Step 4 leads to a decision point: “Is beta intervention expected to be effective?â€. If the answer is no, then return to Step 1 “Establishment of theoretical model.†If the answer is yes, then proceed to Step 5. Step 5 is an action box “Confirmation of effectiveness of beta intervention via RCT [randomized controlled trial]â€. Step 5 has two arrows. One leads to the information input/output box “Centralized database.†The other arrow from Step 5 leads to a decision point: “Is beta intervention effective?â€. If the answer to this question is no, then return to Step 1 “Establishment of theoretical model.†If the answer is yes, proceed to Step 6. Step 6 is a product “Release of new intervention.†This is the end of the flow chart.]](http://www.sbm.org/UserFiles/image/fall2018_most-figure.jpg) What were some of the most memorable things you learned or gained from attending the training?
What were some of the most memorable things you learned or gained from attending the training?
