

SBM's 2009 Annual Meeting & Scientific Sessions
Behavioral Medicine: From Evidence to Practice and Policy
April 22-25, 2009
Palais des Congres de Montreal - Montreal, Canada
July 21-September 12, 2008
Abstracts Accepted

Bonnie Spring, PhD
PRESIDENT'S MESSAGE
On Doing It All
It is a great honor to serve as your President and a genuine pleasure to work with our talented membership. The Society of Behavioral Medicine celebrates its 30th birthday in 2009. We are old enough to have learned a thing or two, yet energetic and idealistic enough to act as a force for good. As SBM approaches this next developmental milestone, it behooves us to reflect on its history and future aspirations. In this column, I will offer my perspective. Let me also extend an open invitation to share yours.
Past
The NIH Roadmap has ushered in an exciting era of translation between research and practice. I am fond of a model of the roadmap published by Westfall, Mold and Fagnan (2007) and reprinted below. I like this particular depiction because it reminds me of SBM's history. Since I began attending annual meetings, the membership's modal research focus has rotated through each major element of Westfall et al's translational cycle. In late 1970s and early 1980s, our founding figures built a strong basic science foundation for the field. The prevailing emphasis at annual meetings was on biopsychosocial mechanisms that underlay behavior and disease.
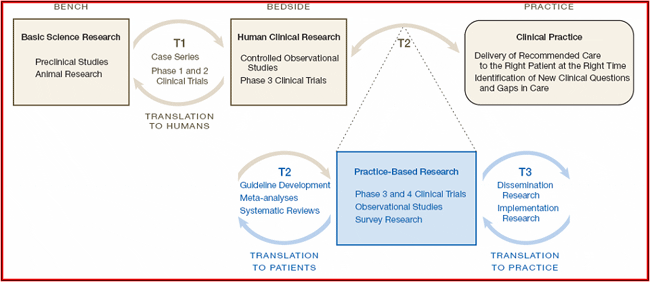
Westfall, JM, Mold, J, & Fagnan, L (2007) Practice-Based Research: “Blue Highways” on the NIH Roadmap. JAMA, 297: 403-406. Copyright© 2007 American Medical Association. All rights reserved.
In the later 1980s and early 1990s, a strong T1 translational interest began to emerge. Conference attendees were treated to new research that established parallel biobehavioral processes across animal and human studies. The Trans-Institute NIH Behavioral Medicine study section of the mid- to late 1990s pressed forward the T1 translational curve. Reviewing both basic research and applied clinical trials, the Review Group evolved a shared point of view. A core premise was that the intervention trials of greatest lasting value would be those that lay bare a theoretical understanding of biopsychosocial mechanisms.
By 2000, the T1 interest in early phase intervention development had given way to an emphasis on more formalized phase III trials, first of efficacy and then of effectiveness. Many of us had easily transferred the methods of basic science experimentation to intervention development. Now we scrambled to learn a new science of clinical trials methodology. Basic science presentations at the annual meeting became fewer in number. Emphasis shifted subtly to which interventions work and how to learn them.
Also around the turn of the century, a strong interest in public health models gathered momentum at SBM. On the one hand, our membership rejoiced that many intensive behavioral medicine interventions show strong efficacy. On the other hand, we grappled with the realization that penetration into the population at greatest need of intervention remains modest. There arose great concern about extending behavioral medicine's reach to have broader population impact, especially among the underserved. A productive outcome was full-scale embrace of ecological models that endorse intervening synergistically at multiple levels (individual, interpersonal, organizational, community, and public policy) in order to magnify and sustain healthful change.
Release of the Institute of Medicine's report on health care quality (IOM, 2001) was a sentinel event that marked the beginning of the current decade. As the report aptly stated, "Between the health care we have and the care we could have lies not just a gap, but a chasm (p.1)." To address the translational gap, SBM formed two standing committees: Evidence Based Behavioral Medicine (EBBM) and Health Policy. Dividing up the ecological space, EBBM focused chiefly on interventions targeted at the individual and interpersonal levels, whereas Health Policy emphasized intervention at the community and public policy levels. Both Committees took steps towards T2 translation. EBBM endorsed comprehensive, transparent reporting of clinical trials and increased engagement in research synthesis. Health Policy crafted policy briefs that give legislators a pithy, user-friendly overview of evidence and action recommendations for such pressing health problems as childhood obesity.
Crossing the boundary between individual and population outreach in such a manner was sheer cutting edge brilliance on SBM's part. Few institutions have tried to harmonize individual clinical and public health approaches, especially across the multiple disciplines that comprise SBM. Although abundantly worthwhile, the task is challenging. Misunderstandings abound. They are a natural part of the process of recognizing differences, understanding and respecting them, and moving forward.
Present
We often describe SBM as a "big tent." The citizenry in our tent hails from 17 different primary professions and claims topical interests represented by 15 SIGs. Our heterogeneity generates exciting cross-talk that draws members to annual meetings. Maintaining SBM's balanced portfolio of interests and approaches is vitally important. Diversity in discipline, specialty, and approach is a large part of what invigorates the Society.
Our members' engagement in all phases of Westfall et al's (2007) translational cycle conveys particular richness. No phase is optional: discontinuing any step jeopardizes the entire enterprise of behavioral medicine research and practice. Of late, we are especially keen to undertake T3 translation, whereby we disseminate, implement, and adapt (but do not enervate) effective treatments to new contexts. We aspire also to grow more adroit at the reciprocal translation processes of practice-based research. But we cannot amputate the vital pipeline of basic research and new treatment development. Doing so would eventually consign us to a dark age of stagnant science and outmoded treatment. In a nutshell, we need to do it all because we are interdependent. Our game is not a zero sum one. We succeed not by crowding out our neighbor, but rather by making the tent, the funding pot, and the job market big enough to support us all.
Our 2007 annual meeting featured a debate on the question: what kind of evidence is most needed to advance behavioral medicine? My answer is: many different kinds. According to the philosophy of evidence-based practice, the kind of evidence best suited to answer a question depends upon the type of question being asked. Trying to use the same research design to answer every important practical question would be like trying to function as a carpenter using only one tool. To answer prognostic questions about risk or protective factors or developmental course, we need observational cohort studies. To learn whether a new treatment improves outcomes compared to an alternative treatment, a well-conducted randomized controlled trial (RCT) is ideal. But it will not always be feasible to conduct an RCT, and well-implemented quasi-experimental studies may offer more compelling insight than a poorly conducted RCT. It is particularly hard to conduct RCTs to test policy interventions. Just try to imagine the state legislature that would agree to have its policies randomly assigned! To answer some questions, an RCT is at best inefficient and at worst inappropriate. For example, when trying to gauge a treatment's acceptability to an unfamiliar population, initial qualitative methods are much more informative.
Importantly, we cannot wait for the perfect evidence before taking action to address urgent public health problems. Following the evidence-based practice process, we and those affected by the decision, need to select an initial action course based upon the best evidence available, integrated with consideration of contextual characteristics and resources. Having chosen an initial intervention, the equally important next steps are to collect and analyze context-specific data on processes and outcome, and then adjust course based on the new practice-based evidence (Council on Evidence-Based Behavioral Practice, 2008).
Future
At its post-conference strategic planning meeting in San Diego, SBM's Board discussed several new initiatives. Their intent is to increase the Society's engagement in translational activities and its impact on practice and policy. A further aim is to enhance the infusion of new talent into SBM leadership by creating additional opportunities for members to interface with the Board. All SBM members received an invitation to participate in four new working groups, each of which evaluates a potential new undertaking for SBM. The first working group, headed by Paul Jacobsen, PhD, is considering whether SBM should undertake preparation of practice guidelines. The second group, chaired by Jeff Goodie, PhD, examines SBM's potential involvement in practice based research networks. The third, chaired by Barbara Resnick, PhD, CRNP, evaluates whether SBM wishes to undertake a new journal addressing the needs of behavioral medicine clinicians and public health practitioners. The fourth group, headed by Amanda Graham, PhD, examines where consumers currently turn to find information about evidence-based behavioral medicine practices and how SBM might engage with those resources.
Also to increase the Society's engagement in policy and practice, SBM formally endorsed a clinical practice guideline: USPHS's Treating Tobacco Use and Dependence: 2008 Update, released on May 7, 2008. Based upon review of 8,700 research articles, the USPHS Tobacco guideline draws important new conclusions. For the first time, the guidelines panel found the evidence sufficient to conclude that the combination of counseling and medication is more effective than either alone. Many SBM members participated in crafting the 2008 guideline, either as panelists or reviewers. The ability to create, evaluate and endorse treatment guidelines represents the culmination of many years of hard work. The accomplishment reflects SBM members' increased experience in conducting systematic reviews and guidelines evaluation, as well as increased collaboration between the EBBM and Policy Committees. In its endorsement, SBM enjoys the excellent company of 57 other professional organizations, including the American Medical Association, American Cancer Society, American Lung Association, American Heart Association, and American Public Health Association.
To enhance its policy involvement further, SBM joined forces with two important organizations: COSSA and Partnership for Prevention. COSSA, a consortium of more than 100 professional associations, is an advocacy organization that promotes attention to and Federal funding for the social and behavioral sciences. Partnership for Prevention is a national membership organization dedicated to building evidence of sound disease prevention and health promotion policies and practices, and advocating their adoption by public and private sectors. An article about Partnership for Prevention, prepared by the Society and Professional Liaison Council, will appear in the next issue of Outlook.
We face exciting times. SBM's founding vision remains as astute today as it was 30 years ago. A small number of behavioral risk factors that are amenable to intervention now account for a third of the global chronic disease burden and half of all deaths from chronic disease (Ezzati & Lopez, 2004). The psychosocial needs associated with chronic diseases are becoming recognized (Institute of Medicine, 2008). SBM members are united in their commitment to understand and intervene upon biopsychosocial pathogens in a manner that improves public health. The journey ahead will be an adventure; I look forward to sharing it with you.
Best wishes for a joyful, restorative summer season.

Bonnie Spring, PhD
President, Society of Behavioral Medicine
References
Council on Training in Evidence-Based Behavioral Practice (March, 2008). White paper on Definition and Competencies for Evidence-Based Behavioral Practice. http://www.ebbp.org/documents/EBBP_Competencies_Mar2008_Web.pdf
Fiore, M.C. et al (2008) Treating tobacco use and dependence: 2008 Update. USPHS. http://www.surgeongeneral.gov/tobacco/
Institute of Medicine. (2001) Crossing the quality chasm a new health system for the 21st century. Washington, D.C.: National Academy Press
Institute of Medicine (2008) Cancer Care for the Whole Patient: Meeting Psychosocial Health Needs. Washington, DC: National Academies Press
Westfall, JM, Mold, J, & Fagnan, L (2007) Practice-Based Research: "Blue Highways" on the NIH Roadmap. JAMA, 297: 403-406
2008 Annual Meeting & Scientific Sessions One of the Best Attended!
Dear Colleagues,
Thanks to everyone who attended the 29th Annual Meeting & Scientific Sessions of the Society of Behavioral Medicine (SBM) at the Manchester Grand Hyatt in San Diego, California! We hope you enjoyed the meeting. We had over 1,400 abstracts submitted and over 1,300 attendees making this year's meeting one of the largest and most attended in the history of our Society! Keeping with the spirit of the mission of our society, the scientific sessions covered a broad range of topics within the field of behavioral medicine.
If you were unable to make it this year, there were a number of meeting highlights! The meeting kicked off with a full day of pre-conference workshops, seminars, and courses on a variety of topics geared toward both the scientist and practitioner, including meditation/yoga, NIH peer review, Bayesian modeling, behavioral medicine in clinical settings and behavior therapy. The Presidential Reception officially kicked off the meeting on Wednesday night and was hosted by SBM President, Dr. Peter Kaufmann. During the reception, we were honored to highlight student meritorious abstracts as well as submissions that received citations from the abstract reviewers. The meeting also featured a fascinating array of keynote speakers. Dr. Beverly Thorn packed the house in her engaging keynote address on translating research into practice. We got to hear many of the personal stories about some of the wonderful patients she works with in Pineapple, Alabama. Dr. James Sallis presented the Distinguished Scientist Master Lecture, where he discussed his Active Living Research program and had all of us dancing during this year's physical activity break, and Dr. Edward McAuley reminded us, in a very exciting lecture, of the quality of life benefits of physical activity. Dr. Gregory Miller presented cutting edge research in the fields of epigenetics and psychoneuroimmunology and showed how early life SES and adversity can be embedded in physiology and subsequently impact health outcomes. A special and riveting invited lecture was given by Jessie Gruman who shared how her own personal experiences as well as those of others who have received devastating diagnoses inspired her to write a book for the general public on how to cope with a devastating diagnosis. Then, Dr. Clarion Johnson flew us around the globe as he described his experiences battling occupational health issues in corporate medicine for the international company, Exxon Mobil. In addition to the exciting lineup of Keynote and Master speakers, we had a series of stimulating symposiums and paper presentations covering topics such as basic science to implementation, aging, biological mechanisms in health and chronic disease, health promotion in diabetes, and psychosocial interventions for chronic disease management, among others. Many of our symposiums and paper sessions were standing room only!
This year we combined the awards ceremony, Presidential Address, and the SBM Business meeting in the hopes that we could expose more SBM members to the workings of the Business meeting. A list of our award winners appears below. Although a "business meeting" may not sound exciting, it is an opportunity for members to become familiar and involved with the organization of SBM.
One really fun feature of the meeting this year was the between-session physical activity breaks, which allowed attendees to stretch out and even practice some dance moves. Even if you are not a dancer, at the very least this provided an opportunity for great camera phone shots of your colleagues "getting down" for use in your next departmental slide presentation!
We hope that you enjoyed the Annual Meeting and that you plan to attend next year in Montreal, Quebec, a new location for SBM that we believe everybody will really enjoy. We welcome feedback about how to improve future meetings, so please feel free to contact the Program Committee with your comments and suggestions. The 2009 Annual Meeting Program Chair is Dr. Sherry Pagoto and Program Co-Chair is Dr. Michael Diefenbach.
Frank J. Penedo, PhD
2008 Program Chair
Sherry Pagoto, PhD
2008 Program Co-chair
Award Winners
Distinguished Research Mentor
Michael Andrykowski, PhD
Distinguished Scientist
Tracy Orleans, PhD

Distinguished Service (pictured L to R)
Jasjit S. Ahluwalia, MD, MPH, MS (not pictured)
Linda C. Baumann, PhD, APRN, BC, FAAN (not pictured)
Edwin Fisher, PhD
Rick Seidel, PhD
Peter G. Kaufmann, PhD (President 2007-2008, making awards)
Frank Penedo, PhD
Marc Gellman, PhD
David Wood
Early Career Investigator
Guadalupe Ayala, PhD, MPH
LifeScan Diabetes Award
Vicki Helgeson, PhD
Young Scholar Travel Award for Women and Cancer Research
Jada Hamilton
Gareth Lloyd
Valerie Tremblay
Distinguished Student Awards
Travel Scholarship: Hannah Faye Chua, PhD
Outstanding Dissertation: Michelle Segar, PhD
Excellence in Research: Lucia Leone
SBM Forms New Publications Committee
At its Fall 2007 meeting, SBM's Board of Directors approved a plan to create a new Publications Committee to serve as the advisory and oversight board for Annals of Behavioral Medicine. This decision placed SBM among the ranks of a growing number of scientific organizations that have formed publications committees to oversee their peer-reviewed journals. The committee's main mission is to foster the growth and development of Annals, and to ensure that it meets the highest standards of contemporary scientific publishing. The committee will also be involved in the selection of a new Editor-in-Chief in 2010, to replace Dr. Alan Christensen when his term ends.
The Publications Committee is part of SBM's Publications and Communications Council and is chaired by Kenneth Freedland, PhD, Professor of Psychiatry at Washington University School of Medicine in St. Louis. Susan Czajkowski, PhD, Program Officer in the Clinical Applications and Prevention Branch of the Division of Prevention and Population Sciences at the National Heart Lung and Blood Institute, is an ex officio member of the committee in her capacity as the Secretary/Treasurer of SBM.
In January 2008, a call for nominations for members-at-large of the committee was distributed to the entire membership of SBM. Nearly 50 members responded to the call, reflecting a high level of interest in Annals and in committee service to SBM. The applications were carefully reviewed to identify candidates who were highly qualified to serve on this committee. Relevant editorial experience, such as journal editorships, membership on other publications committees, and membership on editorial boards, was the primary criterion. Secondary criteria such as academic rank and numbers of peer-reviewed publications, were also considered. Profession and area of research were tertiary criteria, in order to promote diversity among committee members.
Five new members-at-large of the Publications Committee were confirmed by the Board of Directors at the March 2008 meeting in San Diego: Sherri Sheinfeld Gorin, PhD, Associate Professor of Health and Behavior Studies at Columbia University in New York; René Martin, PhD, RN, Associate Professor of Nursing at the University of Iowa in Iowa City; Lynn Rew, EdD, RN, AHN-BC, FAAN, Denton & Louise Cooley and Family Centennial Professor in Nursing at the University of Texas at Austin School of Nursing; Tim Smith, PhD, Professor and Director of Clinical Training, Department of Psychology, University of Utah, Salt Lake City; and Lydia Temoshok, PhD, Professor of Medicine and Director, Behavioral Medicine Program, Institute of Human Virology, University of Maryland School of Medicine, Baltimore.
The committee is currently developing its initial policies and procedures, and will start to phase in its oversight functions during Dr. Christensen's final year as Editor. Dr. Christensen is also serving as an advisor to the committee during its start-up phase.
Submitted by Kenneth Freedland, PhD, Chair of Publications Council
Why I am a Member of SBM
Two words - Contagious Collegiality!
Unlike many graduate school applicants I consider each year, I was not born with a yearning for my career field! Through my own graduate training program, I was infused with enthusiasm for Behavioral Medicine and began to appreciate the benefits of SBM membership. I also admired the energy in my department leading up to the SBM meeting. Students and faculty prepared presentations, seeking feedback from peers. Being part of this effort helped develop my professional identity.
Contagious collegiality is how I describe the multidisciplinary mix of friends and colleagues from diverse backgrounds who convene at the annual meeting. Trainees discover a wealth of cutting edge topics and perspectives. As a professional I have also come to value the many opportunities to contribute to SBM's growth that extend far beyond the Annual Meeting.
Submitted by Jeff Kibler, PhD
Outlook Newsletter Welcomes New Team of Assistant Editors
We are pleased to announce the addition of 13 new Assistant Editors to the Outlook team. The Assistant Editors represent many of SBM's active and growing Special Interest Groups and have been tasked with providing SIG-related content for each of the Outlook issues. Be sure to check out three articles coordinated by the Assistant Editors in this issue: 1) Limited Dollars Raise Tough Questions: Is Funding for Physical Activity Research a Case of Either/Or?; 2) Spotlight on the Spirituality and Health SIG; and 3) Terminology Primer and Exciting New Directions from the Behavioral Informatics SIG. If you have SIG-related content that you would like considered for an upcoming issue of Outlook, please contact the SIG Assistant Editor listed below.
| SPECIAL INTEREST GROUP | LIAISON | CONTACT INFORMATION |
| Aging | James Hall, PhD | University of North Texas Health Science Center Fort Worth, TX jhall@hsc.unt.edu |
| Behavioral Informatics | Beth Bock, PhD | Brown Medical School / The Miriam Hospital Providence, RI bbock@lifespan.org |
| Mary Gregerson, PhD | Family Therapy Institute of Alexandria Alexandria, VA Oltowne@aol.com |
|
| Cancer | Maria Kangas, PhD | Macquarie University New South Wales Australia maria.kangas@mq.edu.au |
| Child and Family Health | Willa Doswell, PhD | University of Pittsburgh Pittsburgh, PA wdo100@pitt.edu |
| Complementary and Alternative Medicine | Suzanne Danhauer, PhD | Wake Forest University Health Sciences Winston-Salem, NC danhauer@wfubmc.edu |
| Ethnic and Multicultural Health | Michelle Martin, PhD | University of Alabama at Birmingham Birmingham, AL mmartin@dopm.uab.edu |
| Integrated Primary Care | William Sieber, PhD | University of California, San Diego La Jolla, CA bsieber@ucsd.edu |
| Obesity and Eating Disorders | Daniel Rodriguez, PhD | University of Pennsylvania Philadelphia, PA drodrig2@mail.med.upenn.edu |
| Physical Activity | David Marquez, PhD, MS | University of Illinois at Chicago Chicago, IL marquezd@uic.edu |
| Spirituality and Health | Karen Kim, PhD | University of Arkansas for Medical Sciences khk@uams.edu |
| Student | Yasmin Asvat, BS | University of South Florida and Moffitt Cancer Center yasvat@gmail.com |
| Women's Health | Leanne Mauriello, PhD | Pro-change Behavior Systems West Kingston, RI lmauriello@prochange.com |
The Spirituality and Health SIG submitted the following description of the Spirituality and Health Institute at Santa Clara University as an example of how faculty from a variety of institutions and disciplines may come together with common interests with little expense to collaborate and discuss ideas that might result in productive projects. For a small amount of money to fund lunch, colleagues can brainstorm together as well as benefit from each other's expertise and wisdom. We hope that this article encourages others to consider how they could use this model to help enhance their research and practice through transdisciplinary and trans-institutional collaborations.
Karen Hye-cheon Kim, PhD
Spirituality and Health SIG Assistant Editor to Outlook Newsletter
The Spirituality and Health Institute (SHI) at Santa Clara University:
Building Productive Collaborations on a Shoestring Budget
The Spirituality and Health Institute (SHI) at Santa Clara University was developed in 2002 by SBM fellows Thomas Plante and Carl Thoresen to provide a forum for quality multidisciplinary and multi-site collaborative research and practice in the area of spirituality and health broadly defined. With a modest grant from the Santa Clara University Ignatian Center, a small group of faculty from Santa Clara, Stanford, the University of California at Berkeley, and the Graduate Theological Union joined several community professionals from the Roman Catholic Diocese of San Jose and Hospice of the Valley. Faculty represent a variety of academic disciplines including psychology, public health, religious studies, English, engineering, philosophy, among others. While some of the faculty and community professionals are actively engaged in their spiritual and religious traditions and practices that represent Catholic, Protestant, Jewish, Buddhist and others, some are religiously unaffiliated. The group includes a number of SBM members in addition to Tom and Carl mentioned above such as Doug Oman, David Feldman, and Shauna Shapiro.
Grant money since 2002 has funded quarterly lunch meetings at the Santa Clara University faculty club. Collaborative projects and ideas are discussed without particular detailed agenda to allow freedom to follow the will and inspiration of the group. Interested members often collaborate in small subgroups and periodically bring in other professionals as desired for specific topics and projects. There are approximately 12 SHI members at any one time with guests from a variety of specialties also included as desired.
What is remarkable to me is that bringing thoughtful, motivated, talented, diverse, and interested people from multiple disciplines and institutions together with a common focus on spirituality and health research and practice can result in so many creative and productive projects with very little financial support. I jokingly refer to our numerous projects as being funded by "lunch money."
Recent projects have included hosting a spirituality and health pre conference event at Santa Clara University in association with the Society of Behavioral Medicine's national convention during March 2006. SBM members from across the country attending the San Francisco convention were bused to Santa Clara University (about an hour south from the convention site) for the pre conference day. Additionally, members of the SHI group presented a symposium at the American Psychological Association convention during the summer of 2007. Several of us will present at the APA convention in Boston this summer. The group also recently published an edited book in 2007 by Greenwood that was co-edited by Tom and Carl entitled, Spirit, Science, and Health: How the Spiritual Mind Fuels Physical Wellness. Finally, the group has published a large number of collaborative empirical research projects in recent years. These projects have focused on meditation practices and health outcomes, the development of and health benefits of compassion among other topics.
Our model and process could easily be incorporated at other university settings. All that is needed are motivated, interested, and diverse professionals who are focused on spirituality and health research and practice fueled by a little bit of lunch money.
Those interested in further information may wish to check our web site at http://www.scu.edu/ignatiancenter/spirithealth/index.cfm or contact me at tplante@scu.edu or (408) 554-4471.
Submitted by Thomas G. Plante, PhD, ABPP
Limited Dollars Raise Tough Questions: Is Funding for Physical Activity Research a Case of Either/Or?
As an active member of the Physical Activity (PA) Special Interest Group (SIG) and the PA SIG Assistant Editor of Outlook, Dr. David Marquez asked two funded, respected SBM researchers to take on this question. Drs. Claudio Nigg and Barbara Resnick were asked to write mock letters to a funding agency requesting that more funding be budgeted for physical activity research for youth or older adults, respectively. In a time of increasingly limited budgets for behavioral medicine research, funds are often allocated to address specific topics or to study certain subgroups of individuals. It is an unfortunate reality for researchers at the present time, and one that warrants thoughtful consideration. The purpose of this article is to encourage SBM members to think about where they stand on this issue, and to consider arguments from the opposing viewpoint. The take home message is that this is not a question of either/or: we clearly need to advocate for funding across the entire lifespan - young and old - to optimize what we know and to promote health among Americans of all ages.
Disclaimer: These mock letters to a funding agency were written to have researchers critically think about funding decisions. They are not letters that will be sent to a funding agency, nor are they meant to suggest that the authors think funding should be cut from any areas of research. Rather, both authors fully support funding for research across the lifespan. For this article, however, they were asked to take a specific side of an argument.
Dear Funder,
As the baby boomers retire in the next 15 years, a lot of attention will be drawn to this age group. They will have significant clout and will impact the political and private agenda, as they have the resources to influence these systems. However, there is a group that does not have this luxury and will not have the same resources to argue their cause. That group is our youth.
For example, Jenny, a 5-year old girl starts kindergarten already overweight. She spends about 3-4 hours each day with her handheld computer game or watching TV, snacking on chips and eating fast food or frozen dinners. The school system she is in has a focus on math, reading, and writing, and has relegated PE, health, art, and music to only once per week. Her parents have to work to afford housing and to pay off the car and university loans, and do not have time to cook fresh meals or prepare healthy snacks, let alone go outside to play for half an hour with her. Thus, the family eats out a lot at fast-food restaurants or puts frozen meals in the microwave. Jenny is actually quite common in our cities, towns, and villages across the USA. She has very little chance of growing up healthy unless more attention and resources are directed towards the health of our youth.
Today's youth will be the first generation to experience poorer health and not live as long as their parents. Unhealthy children become unhealthy adolescents and unhealthy adolescents become unhealthy adults. For example, only 30 years ago early onset diabetes meant getting diabetes around 30-40 years old. Today, as many as one in four children are overweight (95% of weight for their height) entering Kindergarten. Relatedly, we now have overweight children with diabetes who have to worry about the complications such as limb amputations and blindness in their 20s.
Increasing funding commitment to health research addressing youth will have positive impacts on a broad range of issues including:
- Chronic disease (cancer, diabetes, obesity, cardiovascular disease, etc.)
- Infectious disease (tuberculosis, SARS, Dengue fever, HIV/STD etc.)
- Prenatal and infant health (genetics, low birth weight, SIDS, etc.)
- Pro-social development (conflict resolution, bullying, cooperation, etc.)
- Optimal development (gene-environment interactions, physiology, psychology, etc.)
- Academic achievement (optimizing performance, focus, concentration, etc.)
- Leadership development
- Multi-generational involvement for health (caregiving, caretaking, family building, etc.)
- Health technologies (objective and subjective assessment, intervention, etc.)
More importantly, the health care system costs are increasing at an alarming rate. By 2050 the costs will actually be larger than the gross domestic product of the U.S. Essentially the health care system as we know it will either undergo a drastic change or collapse within the foreseeable future. Therefore, the children of today will have poorer health and a broken health care system to take care of them.
I urge you to consider this as we investigate how to ensure that children and youth adopt and maintain healthy behaviors and lifestyles so they will not have to rely on a broken health care system. We must focus our resources and attention on our future - and our future is our children.
I trust you will make the right choices.
Sincerely,
Claudio Nigg, PhD
Department of Public Health Sciences
John A. Burns School of Medicine
University of Hawaii at Manoa
Dear Funder,
We are currently in a time period in which careful consideration must be given to the allocation of financial resources. I am, however, requesting that you consider the distribution of an increased percentage of funds to the National Institute of Aging (NIA) this year compared to the resources that were received in the 2007-2008 funding period. The NIA, as you well know, was established in 1974 and is one of the 27 Institutes and Centers of the National Institute of Health. NIA was developed to provide leadership in aging research, training, health information dissemination, and other programs relevant to aging and older people. Subsequent amendments to the initial legislation designated the NIA as the primary federal agency on Alzheimer's disease research. In 1974, the establishment of NIA was innovative and important. Today, however, the existence and viability of NIA is critical. It is estimated that in the next 25 years there will be 70 million Americans reaching retirement and the impact this will have on our economic, health care, and social systems must be addressed. Individuals are spending more years of life in older age and thus must learn how to optimize life with the subsequent changes that occur. Despite some evidence that the prevalence of disability among older adults is declining, the majority of older individuals have at least one chronic illness and a large percentage can expect to have impairments in abilities to perform basic and more advanced activities of daily living. It is essential to understand the issues that older adults face physically and cognitively and to establish solutions to the challenges encountered in this age group. Such work has an impact on every American directly as we are all aging, and indirectly as each of us are or will be a caregiver at some point in our adult lives.
Through research we have been able to establish innovative approaches to care for frail individuals and those with multiple co-morbidities. This work has helped lead the way toward decreasing disability associated with aging and optimizing quality of life. Future research in aging is geared toward such things as:
- increasing the understanding of Alzheimer's disease, changes in memory and cognition, and other degenerative diseases of the nervous system, and developing interventions to prevent, diagnose early, and treat these conditions;
- increasing our understanding of cardiovascular disease, cancer, and diabetes and considering personalized approaches to prevent and manage these diseases across the lifespan;
- helping older adults with vision, hearing, and other sensory disorders;
- addressing common bone, muscle, skin, joint, and movement disorders;
- understanding the impact of nutrition and exercise;
- optimizing surgical interventions;
- establishing new biological and technological interventions to optimize life quality for older individuals; and
- expanding our understanding of the physical, psychological, psychiatric, and social changes that occur. Without additional resources allocated to the NIA, this critical work cannot be done. Halting our discovery of knowledge in these areas at a time when greater understanding is needed to manage the aging of the baby boomers would be devastating to those of us aging as well as to the children and grandchildren who will be forced to provide care without sufficient information or direction.
Sincerely,
Barbara Resnick, PhD, CRNP, FAAN, FAANP
University of Maryland School of Nursing
Department of Epidemiology and Preventive Medicine
University of Maryland School of Medicine