Editor's Note

William J. Sieber, PhD
Some terrifically informative articles this time around, including some very valuable experiences shared by seniors in the field in "Ask the Experts". Thanks to the “experts” who helped in these replies: Jim Sallis, Sherry Pagato, Amy Huebschmann, Rachel Shelton, and Heather Cole-Lewis.
- What leadership roles should a mid-career faculty member pursue for career development and advancement? How does one decide if asked by a senior colleague to take on a leadership role in an activity in which one does not see value (e.g., improving work-life balance for faculty)?
Leadership roles that provide national visibility and leadership potential, and involve other senior leaders for support/advice would be seen as good opportunities. Examples might include opportunities at professional societies (e.g. SIG chair), Associate Editor at a journal, and associate director at a center. I think it depends on the timing and opportunity as to whether to take it, and the type of setting-- e.g. in going up for tenure at that time point, will you benefit more from grant-writing/pubs or national visibility. And recommend taking 1-2 leadership opportunities at a time.
SBM provides a number of leadership roles that I believe provide much value to career development and advancement. Examples include chairing a SIG or Committee, running for Member Delegate or other elected positions. Within an institution, I would look for roles that add value to your work. I co-led a K award writing group when I was midcareer and it was instrumental to my receiving a midcareer K24 mentoring award.
If asked by a senior person to take on a role where the value isn’t apparent to you, the first step may be in asking them what they see as the value for you. When I was junior, I didn’t always understand the value of certain roles until I participated or asked for more information. In cases where it is clear that there is no value, politely declining is best.
These can be challenging professional situations— it is important to avoid taking on more responsibilities than you can fulfill. To avoid that problem, keep in mind that you don’t need to accept these types of requests immediately. Instead, ask for more information about the opportunity so that you know better whether you can and should pursue it. Our ETCD council suggests you consider multiple factors in these decisions. First, who is asking you to take on this role? If it is your Dean or boss, it is much more difficult to say “no” than if it is a senior colleague who is not in your direct chain of command. Second, how much time commitment is required? Can you add that commitment to your existing workload or do you need to offload something else to others in order to take this on. Third, how does it align with your professional interests? In academics, we are all expected to provide some service to the university, and if you can carve that out as an area that you personally value that is ideal. In this specific instance, you note that you do not see value in the activity, so that should influence your decision. Fourth, if you take this on, is there a service activity you are already doing that you could pass on to others? In certain circumstances, you may be able to negotiate the ability to give up a separate commitment that you are now doing in exchange for doing this new opportunity. Another important factor is that if you’re going to say no, you should ideally offer some assistance such as finding another person who is interested and available, or offering to help “behind the scenes”.
Consult with your department chair because you need to make sure you are investing your time in ways that will be valued and appreciated for promotion purposes. If you don’t see value in the activity, just say no. Life is too short to take on meaningless work. Our jobs involve enough distress from rejections, funding rates, etc. – you need to enjoy what you are doing to survive, so politely decline uninteresting opportunities.
- When you have met a colleague at a meeting who has research interests that align with yours, how do you decide whether or not to develop a research collaboration together?
One consideration is whether the relationship will be mutually beneficial. I am particularly keen to connect with potential collaborators that add a unique expertise that is lacking on my team. Another consideration is whether the individual has similar goals and work styles. For example, when I’m asked to collaborate on a grant proposal that is due in a couple of weeks, I often have to decline because I find that I’m the type who has to plan way ahead for grants and spend a lot of time thinking about the project in advance. Other folks thrive on the pressure of last minute, but that just stresses me out. Neither work style is right or wrong, but I find the best projects come out of compatible work styles. How much time is available factors in as well. I have some phases where I’m just buried and cannot jump into anything new. In this case I politely decline and mention possibly connecting at a later date. There is no sense in jumping into something when you are spread too thin already.
I usually start with something small (brief report, abstract for conference, lit review) to get a sense of whether the collaboration is worthwhile. I also have a discussion about timeline and goals, since those are critical considerations to make sure we are aligned on.
To collaborate or not to collaborate – that is the question. Professional networking is important to be aware of others in our field, but it is yet another step in a professional relationship to start collaborating with a new colleague. A good rule of thumb is that a collaboration will work well when all parties benefit. For example, if you have a research program you have only tested in a population of undergraduate students and you meet a colleague who works with a clinically diseased population, it may be advantageous to work together to test this method in a new population. One way to identify potential areas of mutual benefit can be looking at their curriculum vitae for the areas where they have published and the method expertise they identify. Even if there is the potential for mutual benefit, this may not be a good time for you or your colleague to collaborate in terms of your current research priorities – that is also important to consider. In addition to clarifying the potential for mutual benefit from collaboration, it is important to determine if your respective work styles fit well together. This latter issue can be one of the most challenging to determine. One way to go forward can be setting up some “professional first dates”, so to speak. For example, ask them to consult on a small aspect of a current grant with regard to their methodologic expertise, and use those interactions to determine if bigger collaborations are going to be mutually worthwhile. You can also “phone a friend” – if they have published with a close colleague of yours, you can ask that colleague for input on their collaborative experiences together. Yet another “professional first date” option would be to develop a paper idea together and see how your interactions are on that writing project. Another opportunity is to simply meet with them to identify areas of shared interest and to decide if there are any simple ways to collaborate. If this is a potential mentoring relationship, it is important to identify whether the mentor has enough time to take on the mentee, whether the area of mentoring is strategically important to both the mentor’s/mentee’s main area of research, and what are the time commitments required for this mentorship.
I love meeting colleagues with similar interests, but there is a danger of getting caught in an echo chamber if you’re too like-minded. One of my first department heads advised me to collaborate with people who are different and to avoid redundancy. Collaborations that bring together members of different communities lead to more intellectual cross-pollination and can help to create more impact. So, to answer your question, if a colleague shares a general research interest, I look for differences that could make a collaboration interesting and rewarding for both of us.
- How does one go about finding job opportunities outside academic medicine?
Networking and conferences like SBM are great places to start. Introductions through people who have taken non-traditional paths, Linked In, etc. and asking for informal interviews are good avenues.
I think a first step is to reach out to colleagues who have jobs outside of academic medicine and find out what experiences and skills are necessary and which conferences are great for networking with industry. A number of SBM members have positions outside of academic medicine---reaching out to them will be valuable. I find that having a social media presence (e.g., LinkedIn, Twitter) that showcases your skills can help with career networking---industry folks regularly use social tools for networking. LinkedIn will also send emails with job announcements that fit your profile so keep it up to date!
When I have had opportunities outside of academia come up (typically for consulting), they have generally come up because somebody read a piece in the popular press about my work.
-- William J.Sieber, PhD
President's Message Extending Our Reach
Gary Bennett, PhD, SBM President

Gary Bennett, PhD
SBM President
On November 13 this year, millions of Americans instantly developed hypertension. This time, it wasn't because of political news, but because the American Heart Association which changed the diagnostic threshold for hypertension from 140/90 to 130/80. The move was motivated by an increasing amount of empirical evidence demonstrating that we could produce even greater reductions in cardiovascular disease risk by pushing blood pressure below the previous threshold. The new guidelines, Association leaders argued, might help providers more quickly identify and treat those who would benefit from blood pressure lowering therapy. In response to the announcement, pharmaceutical company stock prices jumped almost immediately. For investors, the updated guidelines forecasted a potentially massive increase in prescriptions for antihypertensive medications. While that may happen, medications aren’t the only — or likely even the best — treatment for patients with hypertension, particularly for those with blood pressure levels near the new threshold.
No, there’s another suite of treatment solutions that are incredibly powerful, impact blood pressure in a manner similar to medications, with fewer side effects, have significant spillover benefits for overall health, and can reduce the risk of diabetes, sudden death, cancer, and even Alzheimer’s disease.
That solution is behavioral medicine.
Indeed, our field knows a great deal about the impact of behavioral and psychosocial factors on blood pressure. Increasing activity, improving diet, reducing weight, adopting the DASH dietary pattern, and reducing chronic stress can each independently reduce blood pressure, not to mention their potential synergistic effects.
None of this is likely surprising to SBM members. But the challenge facing our field is how to move important findings like these beyond the bounds of our community. This year’s theme, “Extending Our Reach,” is intended to facilitate exploration of this question. As Rachel Shelton and I recently argued, if we want behavioral medicine innovations to meaningfully influence policy, practice, and programs then we must extend our reach to a range of stakeholders; particularly those who are unfamiliar, unready, and unused to working with us. Rachel and her team have curated an amazing lineup of annual meeting speakers, who will tackle this issue from a wide range of perspectives. We've also used the theme to shape our slate of activities this year. I’d like to update you on our progress since my last message.
Impacting policymakers
It has become tradition that at our fall meeting in Washington, D.C., Executive Board members take time to visit their congressional representatives. These Hill visits are an important way for the SBM leadership to share our ongoing initiatives, empirical findings, and policy perspectives with federal policymakers. This year, we had an unbelievable response from our Board; almost all of our members visited the Hill. We also decided to greatly expand the roster of Hill visitors beyond the Board. We ultimately brought 30 SBM members to the Hill, which allowed us not only to reach many new congressional offices, but to ensure coverage on both sides of the aisle. We spent the day shuttling from office to office, in teams of 4, led by a local constituent. This allowed members and their staff to hear from a local resident and to benefit from the groups’ diverse experiences. We also shared the fantastic policy briefs, created by our Health Policy Committee and ratified by the Board. As you might expect, congressional staff were particularly interested in our recommendations about policy solutions to contend with the opioid epidemic. We have received excellent feedback and follow-up responses from the congressional offices, which supports our strategy to develop and cultivate relationships on the Hill.
Influencing industry
The Society is rapidly attracting members who work in nonacademic settings. These SBM members are designing, testing, and disseminating products, grounded in behavioral science theory and evidence. This shouldn't be surprising, as industry has long been a leading adopter and disseminator of scientific innovations. We think there are opportunities for SBM to increasingly engage industry in a responsible manner that has the potential for bi-directional benefit. In particular, we have been exploring the creation of a one-day meeting that will expose industry leaders to the fundamentals of behavioral medicine science. This is an ideal time for such an engagement. Behavior change features prominently in the commercial market, across a range of sectors. There is increasing industry interest in adopting evidence-based behavior change approaches and using our methodologies to evaluate product outcomes. SBM is well positioned to fill this gap. If successful, this meeting presents an opportunity for us to disseminate behavioral medicine science, learn more about adoption considerations, and raise additional resources to support the Society's work. We will provide an update about these activities at the annual meeting.
Telling our story
How do you describe behavioral medicine to your family, friends, or even colleagues? Our field is so inherently interdisciplinary and broad reaching, that it defies easy description. Our efforts to accelerate SBMs impact motivated the Board to embark on a “branding” exercise that will help us better communicate our mission, our programs, and discover areas of potential opportunity. To help us in this effort, we engaged Infinia Group, a New York City-based brand strategy and design consultancy. Over the last few months, dozens of SBM leaders and members have contributed their thoughts about the Society’s history, culture, and potential for impact. Our Board devoted significant time to the effort in our fall meeting; our work will continue through the next year. That said, I can't wait to show you the first pieces of our work ... at this year's annual meeting.
Talking science
As you can tell by the number of times I’ve teased it, I’m pretty excited about the upcoming annual meeting. Our Program Committee, under the leadership of Rachael Shelton, have delivered a fantastic program. The meeting is on track to be the biggest in our history; we’ve had the largest number of abstract submissions ever. This will also be one of the most selective of our meetings. We have a full lineup of speakers, who we’ll be announcing over the next several weeks. Also, please remember that this year‘s meeting will be held on the same weekend as the French Quarter Festival, just steps away from our hotel. So, bring the entire family and make a weekend of it!
Thank you
The holiday season is a wonderful time to reflect on all of those things for which we are grateful. I appreciate the help, guidance, and suggestions that so many of you have offered this year. I am especially proud that we have been able to engage large numbers of members from outside of our leadership ranks. That could only happen because so many of you have been very gracious with your time and creativity. Thank you. I hope that you have a wonderful, safe, moderately gluttonous, and family-filled holiday season.
Deeds Not Words: SBM Needs your Active Engagement in Our Elections Process
Monica Baskin, PhD, Society of Behavioral Medicine (SBM) Member delegate

Monica Baskin, PhD
A few days before I started writing this article, I had the pleasure of watching my oldest daughter perform in her high school’s award-winning, original one-act play, “Deeds Not Words.” The student-written and produced play presents the story of Lady Constance Lytton, an English aristocrat who in the early 1900’s masqueraded as a working class woman in order to participate in the women’s suffrage movement in Britain. In fact, Lady Lytton joined the most militant group of suffragettes at that time, the Women’s Social and Political Union (WSPU). The WSPU, founded by Emmeline Pankhurst (brilliantly portrayed by my daughter), very publically brought attention to the fact that all citizens had a right and obligation to vote in public elections. The play and ongoing displays of civic engagement all over the world this past year led me to reflect on the responsibility that I have to make sure that my voice is heard and counted in all organizations and groups in which I am a member.
You may be all too familiar with the fact that the US voter turnout for national elections ranks among the lowest of developed counties (61% of eligible voters cast ballots in the 2016 presidential election according to the US Census ). You may also know that on average, only one in five voters cast their ballots in local elections among larger US cities. However, the number of eligible voters for SBM who actually cast a ballot each year is also woefully low. In fact, over the past four years only 29% of SBM members eligible to vote did so.
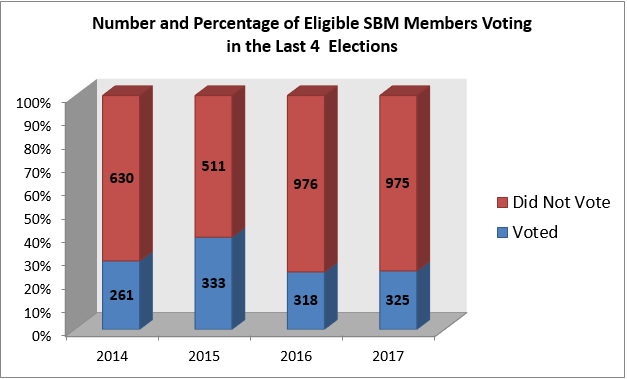
While there are likely a multitude of reasons for low voter participation, the key factors are usually summarized as: (1) barriers to registering to vote, (2) limited information, and (3) apathy. Since the Society of Behavioral Medicine (SBM) already makes voting as painless as possible (automatic registration as a dues paid member, electronic voting with a direct link to the ballot delivered in your email box, 24/7 voting over the course of one month), the Board has more recently decided to implement three approaches to increase member engagement in the voting process for the 2018 elections.
First, the candidates will be asked to record a series of one minute videos in response to specific questions aimed at helping the membership get to know the candidate and their positions on issues relevant to SBM. These videos will be distributed to the membership throughout the election period. It is the hope of the Board that these recordings along with the candidate personal statements will help voters with informed decision-making. Second, the final week of voting of the month-long voting period will be designated as “voting week.” The SBM office will encourage more members to vote using reminder emails. Finally, Special Interest Groups (SIGs) will be asked to encourage members to vote (though not specifically endorsing any specific candidate) on their listservs. If the Chair of the SIG is running in the election, that Chair will not be allowed to communicate through the listserv, but another member of the SIG leadership will take on this task. To further motivate SIG members to vote, an incentive will be offered whereby the SIG with the highest percentage of members voting receives a waived administration fee from SBM for a future pre-conference session. The percentage of voting SIG members will be included in all emails prompting members to vote. Given that key leadership roles of the Society are often decided by only a few votes, we are hoping that all of our members will recognize just how much their active participation can count in shaping the direction of the organization.
On behalf of the Board, we certainly hope that you will make sure that your voice is counted this upcoming election season.
Partnership is Key to Progress: How the Scientific and Professional Liaison Council Helps Extend our Reach
Amy Janke, PhD, Scientific and Professional Liaison Council (SPLC) chair
The Society of Behavioral Medicine (SBM) increasingly partners with professional and scientific organizations who share our vision and goals. The SPLC is the internal leadership group tasked with initiating, developing, and maintaining SBM’s interdisciplinary activities with other scientific and professional organizations.
Benefits of partnering
Partnering extends our reach as an organization. Our liaisons expand professional networks, create new opportunities, and enhance communication beyond the resources available within SBM. These relationships also allow SBM to amplify our message of advocacy as we partner on policy endorsements and briefs.
What makes a good partnership?
The key to a successful relationship is mutual benefit. When forming a new liaison, it is important that both partners collaborate in a way that capitalizes on their respective strengths. The SPLC aims to cultivate partnerships that serve the needs of our membership and the strategic goals of our organization.
What liaison activities has the SPLC fostered with partner organizations?
Partner activities include both one-time events and ongoing work, as long as the activity is deemed to benefit the society and our membership. Preparing joint programming for SBM's Annual Meetings is a regular and ongoing activity of the SPLC with its partners, as is collaboration on policy work and the coordination of journal articles or special issues. We also facilitate information sharing, shared services, common resources, and joint membership.
How are new liaisons formed?
Any member of SBM can propose a new liaison by submitting a brief description of the organization, their mission, and the proposed relationship using our liaison proposal form to the SPLC Chair. If the liaison is considered strategic by the SPLC chair and council, the SPLC chair will bring it forward to the Board of Directors and Executive Committee.
Who are our current partners and council members?
Our liaisons include a range of organizations from large, international groups with diverse, multidisciplinary memberships to smaller societies with a focused membership roster. A full list of current liaisons can be found on the SPLC website, along with the current roster of council members.
How can I help participate in extending our reach?
You likely have many collaborations that extend to scientific or professional societies outside of SBM. These relationships are often how our partners first interact with SBM, and are critical to extending our reach even if a formal liaison between organizations never develops.
If you have an idea for a new liaison based upon your existing relationships, a good first step is to discuss the idea with your Special Interest Group colleagues. Some questions to consider: Do others have an interest in forming a liaison? What are likely shared activities/goals? Is there an SBM member to lead the liaison? The next step is to make outreach to the SPLC chair to propose the liaison. We look forward to your ideas, and thank you for being the society’s best ambassador as we work to extend our reach!
Insights Into a Career in Family Health and Obesity Prevention: An interview with Dr. Kirsten Davison
April Bowling, ScD and Rebeccah Sokol, MSPH; Child and Family Health Special Interest Group (CFH SIG) Outlook Liaisons

Kirsten Davison, PhD
The CFH SIG interviewed Dr. Kirsten Davison to learn more about her career in family and child health and obesity prevention. Dr. Davison, the Donald and Sue Pritzker Associate Professor of Nutrition at the Harvard Chan School of Public Health, has made substantial contributions to family-centered interventions for obesity prevention. Dr. Davison is the creator of the Family Ecological Model and most recent awardee of the 7th Annual Alice Hamilton Award from the Committee on the Advancement of Women Faculty at Harvard.
CFH SIG: What drew you to the field of family-based interventions?
Dr. Davison: Pursuing the field of child development grew from my parents running childcare centers. I worked in those settings from an early age and through college, so I knew that my work would involve children—and with children come families.
CFH SIG: You are well-known as the creator of the Family Ecological Model. What led you to writing that seminal paper?
Dr. Davison: My original training was in human development, where theory is central to all research. That background led to training in applying and adapting existing theoretical frameworks to interventions. I took a class from Nancy Downing, a mentee of Bronfenbrenner, and found her approach to theory helpful. Moving into research on childhood obesity was uncommon for a researcher in human development. Given this direction, I needed to make sense of a multitude of cross-disciplinary literature, and using a theoretical framework was my way to connect dots. To some extent I find using theory is an uphill fight in public health nutrition. It is becoming more common, but it isn’t instinctive, and I think that impacts translational value. For that reason, I have worked to revise the public health nutrition curriculum at Harvard’s Chan School of Public Health to include core coursework in theory and its application.
CFH SIG: What advice would you give to current doctoral students interested in child and family health research?
Dr. Davison: It is advantageous to have some training in human development. Even if you are doing research in nutrition or another field, knowledge of human development allows you to be comfortable with literature regarding family structure and family impacts on health; this helps you find levers for change in child health.
CFH SIG: You have invested significant time and energy into academic mentorship. What made you decide to focus on mentorship, and what advice would you give post-docs and junior faculty seeking mentorship?
Dr. Davison: I’m not sure if it was a conscious decision. I think it was already part of my schema of what it means to be a faculty member, born out of my graduate experience with my own mentor, Dr. Leann Birch. I’ve modeled the culture of my own lab on hers, and she remains a collaborative and guiding force. You may have unique barriers to mentorship at your institution, so sometimes you need to look outside. Take advantage of conferences and research societies – the Society of Behavioral Medicine offers mentorship opportunities. Reach out to people whose work you admire; right before conferences is a great time because then you can meet for coffee in person.
CFH SIG: You have a diverse ongoing research portfolio. What avenues are you currently most excited about?
Dr. Davison: I am energized to take on research with fathers. We are preparing for a large study on how fathers affect children’s health behaviors. I am currently working on funding for this research; it is hard because the perception is that mothers are what matters. But the cultural context of fatherhood has changed in the last couple of decades, and we need to understand fathers’ roles in family health. I am also excited about implementation science. It helps us move beyond randomized controlled trials by giving us generalizable interventions. I’m excited that implementation science is opening a new set of theories and methodologies that reach across disciplines. That’s going to propel childhood obesity research forward into new directions.
Training the Next Generation of Behavior Scientists for Digital Health Research
Cynthia Castro-Sweet, PhD, Digital Health Council (DHC) Member; Heather Cole-Lewis, PhD, DHC chair
The Society of Behavioral Medicine’s (SBM) DHC recently interviewed Dr. Carly Goldstein, Assistant Professor, Warren Alpert Medical School of Brown University; Dr. Danielle Jake-Schoffman, Postdoctoral Research Fellow, UMass Medical School; and Stephanie Goldstein, Doctoral Student, Drexel University, about their perspectives on training for the future of digital health research.
DHC: What do you see as current gaps in digital health training?
Dr. Jake-Schoffman: While many people discuss the value of “team science”, there are few opportunities to practice this in training. Courses or research opportunities where behavioral scientists can gain practical experience on interdisciplinary teams, and more courses in emerging study designs such as optimization frameworks (e.g., Specific, Measureable, Achievable, Results-focused, Time-bound (SMART), multiphase optimization strategy (MOST)) would be valuable.
DHC: What resources have you found particularly useful?
Dr. Goldstein: I attend every digital health talk I can at SBM’s 39th Annual Meeting & Scientific Sessions and Obesity Week. Our field gets hyper-focused on a single health condition when our work should be more translational. I sought out expert mentors at my institution and elsewhere to shape my training and development. Their mentorship has been critical to my career!
DHC: How have professional connections added value to your training?
Stephanie Goldstein: Professional relationships are especially important as the landscapes of technologies and research methods change so quickly. It is helpful to receive guidance from multiple individuals on a particular research or professional issue. They can help facilitate cross-disciplinary contacts for students who may be in programs that are siloed.
DHC: What advice would you offer to trainees in digital health?
Dr. Goldstein: 1) identify numerous mentors to guide your career; 2) apply for grants that allow collaboration with industry like dissertation awards and Small Business Innovation Research/Small Business Technology Transfer (SBIR/STTR); 3) develop relationships with industry partners and collaborators within and outside your field; 4) think critically about the technology you use and the technology that is marketed to you; 5) concentrate on doing good science rather than following the most exciting new development.
Stephanie Goldstein: Trainees must be incredibly self-motivated and confident in their goals/needs. Until more integrated programs are developed, folks will likely have to train in a piecemeal fashion. Build a path that contains teams of mentors/collaborators (rather than any one individual). If desired training is unavailable, reach out to your network (or create a network!) to advocate for your needs and see how you can make it a reality. The field greatly benefits from individuals realizing there is an unmet need and rising to meet it.
DHC: Are there any pitfalls to avoid?
Dr. Goldstein: Many digital health collaborators have just as little experience working with academics as we have with them; it is critical to choose your collaborators wisely.
Dr. Jake-Schoffman: Continue to pursue diverse training, even if your specific interests lie in technologies.
Stephanie Goldstein: The fear of taking the time to learn something new can be a major pitfall. A goal of mine is to find the right balance between feasibility (e.g., what I have the time/resources to learn) and challenge.
DHC: How can SBM advance training in digital health?
Dr. Jake-Schoffman: There is still a large training gap for professionals who what to pursue careers outside of academia. It will be critical to continue to offer trainings and panel discussions to explore the best way to bridge this gap, and perhaps offer a formal mentoring program to match industry professionals with behavior science trainees.
Look Ahead: Interview with Paul Jacobsen, Associate Director of the NCI Division of Cancer Control and Population Science’s Healthcare Delivery Research Program
Marlena Ryba, PhD, Cancer Special Interest Group (SIG) member

Paul Jacobsen, PhD
Cancer SIG: You made many important empirical contributions to the field of psychosocial oncology and it is very important to have someone with your research experience and contributions at the National Cancer Institute (NCI). What about the step to NCI seemed attractive to you?
Dr. Jacobsen: I joined NCI because of the many opportunities that exist to contribute to cancer research through government service. I recommend an article by Barbara Rimer in which she wrote eloquently about government service as a “public and personal good” (Health Education and Behavior, 2016). In my case, I saw an opportunity through work at NCI to help shape the agenda and develop new resources for cancer-related healthcare delivery research.
Cancer SIG: Much of your research included RCTs to test interventions to improve psychological outcomes. Is that research to be a focus at NCI? What might you see to be the directions for psychological intervention research?
Dr. Jacobsen: NCI is already funding numerous studies that test interventions to improve quality of life outcomes in people with cancer and I expect this trend to continue. Among the interesting new directions is the expansion of the populations and the outcomes that are the targets of intervention research. Along these lines, NCI recently issued a funding opportunity announcement seeking applications that test interventions for caregivers of people with cancer (PARs 16-317 and 16-318). Another recent announcement includes a call for research on ways to improve adherence to the growing number of oral anticancer agents (PAs 17-060 and 17-061).
Cancer SIG: How would you describe the current state of cancer care delivery? How can we better address the needs of cancer patients?
Dr. Jacobsen: A National Academy of Medicine report characterized the cancer care delivery system as being in crisis due to the growing demand for care, rising costs, increasing complexity of treatment, and a shrinking workforce. Addressing these issues will require a broad-based approach that engages patients, providers, educators, researchers, payors, and policy makers and encourages them to work together toward common goals.
Cancer SIG: What changes would you like to see in the next 5 to 10 years?
Dr. Jacobsen: I would like to see sustained progress in delivering high-quality cancer care, which has been defined as care that is safe, effective, patient-centered, timely, efficient, and equitable. Healthcare delivery research is likely to play a central role in achieving this goal. In particular, there is a need for research that translates existing knowledge about problems with care delivery into intervention strategies that can have a meaningful impact on clinical practice and population health. Such problems include: disparities in the receipt of curative treatments related to factors such as race, ethnicity, sexual identity, age, socioeconomic status, and geographic region; poorly coordinated survivorship care; underuse of palliative and supportive care measures; and the overuse of screening and surveillance procedures for which evidence is lacking. Addressing these complex issues will likely require multilevel intervention strategies that would be implemented at the individual, provider, practice, organizational, and/or community level.
Cancer SIG: Do you think it’s possible to close the gap between research and practice? If so, how? What advice do you have for researchers and clinicians to achieve that?
Dr. Jacobsen: Since joining NCI, I have greatly enjoyed interacting with members of the Division of Cancer Control and Population Sciences’ Implementation Science Team. My interactions have strengthened my views about the importance of conducting research based on implementation science principles in order to successfully bridge the gap between research and practice. I strongly encourage researchers and clinicians interested in changing practice to become familiar with methodology and findings in this field. If you want to learn more, this is a good place to start.
Cancer SIG: Where do you see the future of the field? Research agenda?
Dr. Jacobsen: I am very pleased to see the research agenda in behavioral and psychosocial aspects of cancer expand to include all phases of translational research. While we still need early phase research focusing on mechanisms and candidate interventions, there are many existing findings that need to be disseminated and implemented. For example, advances in symptom monitoring and management have reached the point where we now need to find ways to incorporate collection of patient-reported outcomes as part of routine clinical practice and provide clinicians and patients with the information and resources to manage identified symptoms according to evidence-based guidelines. This topic is one that will be addressed in a soon-to-be-issued funding announcement developed as part of NCI’s response to the Cancer MoonshotSM Blue Ribbon Panel recommendations.
Cancer SIG: What advice do you have for early career professionals?
Dr. Jacobsen: I think it is most important to connect with mentors who can provide sound advice and guidance about scientific issues as well as professional development. I have benefited greatly from having excellent mentors at every stage of my career.
Cancer SIG: And finally, just for fun, if you didn’t work in cancer, what field would you work in?
Dr. Jacobsen: I think I would have gravitated to investigative journalism. It melds my interests in current events with activities I find myself drawn to (collecting new information, analyzing it, and writing it up for publication).
Research and Training Opportunities in Hospice and Palliative Care
Neha P. Gothe, PhD and Amanda N. Szabo-Reed, PhD; Aging Special Interest Group (SIG) Co-Chairs
Hospice care involves a team-oriented approach to expert medical care, pain management, and emotional and spiritual support tailored to caring for people facing a life-limiting illness or injury. The model is focused on quality of care and life and takes into account the patient's needs and wishes. A detailed history about hospice care is outlined on the National Hospice and Palliative Care Organization page.
National Statistics and Surveys
National Study of Long-Term Care Providers (NSLTCP) is a new initiative by the National Center for Health Statistics (NCHS) to provide reliable, accurate, relevant and timely statistical information to support and inform long-term care services policy, research and practice. The main goals of NSLTCP are to: (1) estimate the supply and use of paid, regulated long-term care services providers, (2) estimate key policy-relevant characteristics and practices, (3) produce national and state-level estimates, where feasible, (4) compare among sectors, and (5) monitor trends over time. NSLTCP is a biennial study of adult day services centers, residential care communities, nursing homes, home health agencies, and hospice agencies. NSLTCP uses administrative data for home health and hospice agencies obtained from the Centers for Medicare & Medicaid Services (CMS).
It is estimated that there are 4000 hospice care agencies in the United States (2014). The number of patients was 1.3 million in 2013. For more data and statistics, visit the NCHS website.
The National Hospice and Palliative Care Organization also provides an annual overview of hospice care delivery. Their annual report can be accessed here.
Research Opportunities
The National Institutes of Health has a number of Funding Opportunities pertinent to hospice and palliative care needs for individuals with rare diseases as well as their caregivers. Below are some currently active announcements (as of November 2017):
Palliative Care Needs of Individuals with Rare Advanced Diseases and Their Family Caregivers (R21)
Advancing the Science of Geriatric Palliative Care (R01)
Research on Informal and Formal Caregiving for Alzheimer's Disease (R01)
Training Opportunities - Becoming a Hospice or Palliative Care Specialist
There are a variety of formal training programs, certificate programs and research training opportunities available in hospice or palliative care. These programs include formalized curriculum to help individuals become a specialist in hospice or palliative care.
Graduate Studies in Hospice and Palliative Care
University of Colorado Denver, Interprofessional Master of Science in Palliative Care
University of Maryland, Master of Science in Palliative Care
Drexel University, Holistic Hospice and Palliative Care Certificate
University of South Florida, Hospice, Palliative Care and End of Life Studies
Post-Docs in Hospice and Palliative Care
Palliative Care Post-Doctoral Research Fellowship Programs
Hospice & Palliative Medicine Fellowship program at University of Rochester
Gerontology, Geriatrics and Palliative Care at University of Alabama at Birmingham
Palliative Care at the University of Texas Health Science Center San Antonio
Other Opportunities for Training
Athena Institute Hospice Volunteer Program
Why Then, Why Now: Interview With Founding Women’s Health SIG Chair, Dr. Helen L. Coons
Kaitlin Roke, WH SIG member; Abbey Kruper, WH SIG member; Emily Mailey, WH SIG Co-chair; and Pamela Geller, WH SIG Co-chair

Helen L. Coons, PhD, ABPP
“The time is now to galvanize support and research around women’s health.”
–Helen L. Coons, PhD, ABPP
In a recent interview with Helen L. Coons, Ph.D., ABPP, the invited founding chair of the Society of Behavioral Medicine's (SBM's) Women’s Health Special Interest Group (WH SIG), she discussed the state of women’s health across the professional spectrum. Dr. Coons is President and Clinical Director, Health Psychology Solutions in Denver and Boulder, Colorado. Also the founder of American Psychological Association’s (APA) Leadership Institute for Women in Psychology, Coons has been extensively involved in women’s health clinical practice, advocacy and leadership development throughout her notable career.
Prior to founding the WH SIG in 2001, Coons chaired the APA Division of Health Psychology Committee on Women’s Health from 1989-1992 and 1998-1999. “This timing was especially critical,” says Coons, because in 1990 there was federal legislature -- The Women’s Health Equity Act -- which began to significantly shift the conversation on women’s health. The history of the WH SIG corresponds to the history of the political movements focused on inclusion of women and persons of color in research, and the recognition of important gender and racial differences in symptom presentation, access to care and treatment.
Women’s health should be a priority.
“While we have witnessed invaluable research on women’s health in the past three decades, we have pressing work to do in any number of areas,” Coons said. She spoke to ongoing disparities in women’s health care and effective translation of research in diverse populations of women across the life span. Women are the primary drivers of healthcare for themselves and within their households; thus, it is clear that keeping women healthy also keeps their families and communities healthy.
Coons believes that a focus on women’s health is not only about working with female patients and their families, but also about elevating the status of women in behavioral medicine. Coons is a staunch supporter of women as professional leaders, especially in a field with the number of women growing exponentially. She believes the WH SIG is a forum to ensure women obtain and succeed in leader roles, have effective negotiating skills, and are able to navigate the diverse challenges related to being a woman in academic and academic medical settings.
The Women’s Health SIG can facilitate inter-professional research, training, and care.
One area where all fields of science have classically struggled is in the translation of high level research to clinical practice. Coons feels strongly that our field continues to lack good translational science in a broad range of women’s health areas. This prevents state of the art assessment, prevention, and treatment of women in all health diversities. To this point, Coons stated, “whether I am in the clinical setting or presenting a continuing education… at least two times a week I have to say that, “I just don’t have good science to tell you where to go here.”
“Some of the most interesting conversations I have are when we are able to bring together researchers and clinicians – and discuss a women’s health issue from both perspectives…” Coons says that the WH SIG can be an inter-professional group that facilitates timely conversations between different healthcare specialists. Such communication can accelerate the translation of research findings to impact individuals, families, communities, health systems, and especially policies. These points highlight Coons’s visions for increased translation, transfer, and application of research that can be uniquely facilitated by active participation in SBM’s WH SIG.
Sleep SIG: Promoting Students’ Sleep and Pre-Conference Course on Using Actigraphs
Brian D. Gonzalez, PhD and Natasha J. Williams, EdD, MPH; Sleep Special Interest Group (SIG) Co-Chairs
Policy Brief on School Start Times
The Society of Behavioral Medicine (SBM) recently released a policy brief urging policymakers to set middle and high school start times to no earlier than 8:30 AM. The brief is grounded in research showing that biological mechanisms regulating sleep change in adolescence resulting in a later natural sleep time for teenagers. Despite this growing body of empirical evidence, most schools today start at a time that’s too early. As a result, most adolescents are not getting the recommended nine to 10 hours of sleep at night and are sleepy during the school day.
Starting school at or after 8:30 AM has been associated with improvements in numerous academic and health outcomes. For example, teenagers with later school start times show better alertness, mood, attendance, and academic achievement compared to those with an earlier school start time. Some barriers should be noted. Changing school start times can be disruptive to families’ schedules, can impact students’ ability to participate in after-school activities, and can cause logistical challenges for school districts, including transportation. Fortunately, these barriers are surmountable, and seem minor in comparison to the overwhelming benefits to students’ academic success and health.
We are hopeful that the policy brief will prompt SBM members to contact their local school boards and federal representatives to develop a strategy to enact this policy that would benefit their community. In conversations with policymakers, it may be helpful to note the endorsement of several key stakeholders, including parents’ groups, sleep-focused scientific societies, the National Parent Teacher Association, and the National Education Association, a national teacher’s union with over 3 million members.
SBM 2018 Annual Meeting Events
We are excited about the caliber of oral and poster presentations on the topic of sleep and circadian health that will be presented at the Annual Meeting. The Sleep SIG will also sponsor a pre-conference course titled “Actigraphy for Sleep and Physical Activity Research: Nuts & Bolts.” This course is intended to provide a how-to for researchers interested in using actigraphs (accelerometers) to study sleep, circadian rhythms, or physical activity. We plan to discuss the entire process, beginning with how to choose a device all the way through a live demonstration of how to interpret actigraphy data. We encourage you to sign up during Annual Meeting registration if you’re interested. Lastly, the SIG will be hosting a business meeting and has plans in the works for an exciting social event. Please stay tuned for additional details in an e-mail to the Sleep SIG listserv. As a reminder, if you haven’t already, please select the “sleep” SIG in your registration and consider joining the Sleep SIG by selecting it in your member profile.
Balancing Pursuit of Your Own Interests with Pursuit of Public Health Goals: Insights from SBM 2018 Debate Participants
Austin Baldwin, PhD, Theories and Techniques of Behavior Change Intervention Special Interest Group (TTBCI SIG) chair and Susan Czajkowsk, PhD, TTBCI SIG co-chair
During the upcoming Society of Behavioral Medicine's (SBM's) Annual Meeting & Scientific Sessions in New Orleans, the Theories and Techniques of Behavior Change Interventions Special Interest Group (TTBCI SIG) will again be sponsoring a debate on a topic of broad interest to the behavioral medicine community. Our SBM 2018 debate topic, “Should behavioral medicine be more solution-oriented than it is currently?” is based on a recent article published in Nature Human Behavior by Duncan Watts, entitled “Should Social Science Be More Solution-Oriented?”
As with past debates, we hope the session will stimulate discussion and consideration of an issue we believe to be at the heart of behavioral medicine’s progress: namely, whether behavioral medicine should adopt a more solution-oriented approach with precise, targeted objectives to address pressing public health problems, or whether it is best to “let a thousand flowers bloom”, with encouragement of researchers to pursue their own interests and “passions”, first and foremost. This topic is not only central to our identity and progress as a field, but is faced by individual behavioral medicine researchers as they pursue their own careers. Of course, there is always a balance, with the ultimate goal being to improve the public health, but we can take different paths, and at times, must choose to emphasize one of these goals more than the other. Hopefully, the two goals converge, but often this is not the case.
To stimulate thinking about this issue and how it relates to individual researchers’ own goals and research trajectories, we asked our four SBM debaters to address the following question:
How can one best balance pursuit of one’s own passions and interests with pursuit of public health goals?
Here are their responses:
Angela Bryan, PhD
Dr. Bryan is a Professor of Psychology and Neuroscience at the University of Colorado Boulder and co-director of the CU Change Lab.
In some ways, this question doesn’t actually arouse any tension for me because from the moment I got interested in pursuing research, it was with the intent of learning the answers to important questions in the domain of public health. From the time I took a course in social psychology as a sophomore at the University of California, Los Angeles, I was taken with Lewin’s notion that there was nothing so practical as a good theory. Though my research interests have expanded to a range of different health and risk behaviors (exercise, eating, substance use) and a wide range of the determinants of those behaviors (genetics, epigenetics, neurocognitive structure and function), the same theme continues to animate my research. I use and build on social psychological theories of behavior to understand what drives health behavior and how we might use that information to encourage that behavior. So I don’t feel the need to “balance” my passions in the research domain with the pursuit of public health goals because they are part and parcel of the same passion.
Ken Freedland, PhD
Dr. Freedland is a Professor of Psychiatry and Psychology at the Washington University School of Medicine in St. Louis.
Scientists in several different fields of experimental and observational research have recently confirmed decades-old predictions based on the standard model of particle physics, Einstein’s General Theory of Relativity, and the Big Bang theory of the origin of the universe. Behavioral medicine researchers engaged in the basic science of human behavior have their own theories, and many are devoted to testing the predictions that flow from them. But they are not theories about the fabric of spacetime or the mysterious nature of quantum entanglement. They are theories about why our grandparents do or don’t take their medications as prescribed, or why men with HIV do or don’t wear condoms, or why kids would rather play video games than go out and get some exercise. These theories bring us no closer to the ultimate truth and beauty of the universe, but that’s okay because they may tell us something useful about some very consequential health behaviors and what we can do to modify them. Our own basic science has meaning, purpose, and value, but only to the extent that it contributes to our applied science and to practical health-related applications of what we are able to learn through our research. So please do pursue your passions and interests, if they happen to be in the basic science of behavioral medicine, but always pursue them with the goal of improving the health of people who need our help. We owe them that, and nothing less.
Elva Arredondo, PhD
Dr. Arredondo is an Associate Professor in the Graduate School of Public Health at San Diego State University.
The pursuits of my research align with public health goals. My program of research involves developing health promotion programs that address poor health outcomes evident in underserved communities. As such, I develop community trials that aim to improve the health status of underserved communities. This research includes understanding the underlying biological and behavioral mechanisms in which public health programs impact health behaviors and outcomes. The rationale for understanding the pathways are not only of scientific interest and value, but align well with public health goals. For example, to inform the development of behavioral intervention programs that are effective, sustainable and scalable, it is important to understand which behavioral change strategies are the strongest determinants of physical activity changes and at the same time to explore moderating factors that facilitate implementation and dissemination of program activities.
Donald Edmondson, PhD
Dr. Edmondson is an Associate Professor of Behavioral Medicine and the Director of the Center for Behavioral Cardiovascular Health at Columbia University Department of Medicine.
The shared public health goals that our field could address are so many, with so much left to do, that almost every individual passion could be pursued in a way that helps the field to address at least one shared goal. For example, there are many basic scientists interested in how an individual’s attention allocation reflects and shapes emotion regulation. Although this relatively specific interest may seem unconnected to broader public health goals, I know scientists that are currently working on incorporating such work into efforts to improve medication adherence in survivors of acute cardiovascular events. The perceived gap between the passions of individual scientists and needs of the field are largely due to a lack of a unified culture of behavioral medicine. Efforts such as the National Institues of Health Science of Behavior Change initiative as well as groups like the Open Science Foundation are beginning to make the connections between subfields more clear. Once we collectively see the connections between our individual efforts and the common goals of our field, it will be rare to find a scientist who chooses to do their work in isolation. Even those working on very early phase projects will have a sense of where their work will likely contribute.
Leveraging Technology for Behavioral Weight Loss Interventions
Valerie J. Silfee, PhD, Obesity and Eating Disorders SIG Outlook liaison

Technology usage in the United States has skyrocketed over the past few decades. According to data from the Pew Research Center, 88% of Americans currently use the Internet, 77% own a smartphone, and 68% use Facebook.1 These rates are also similar across gender, race/ethnicity, and age groups.1 Given this near ubiquity of technology, a considerable amount of research has been dedicated to understanding how we can deliver behavioral weight loss interventions via technology.
What are some of the current delivery modalities?
Researchers have used a variety of mobile health (mHealth) technologies to deliver behavioral weight loss interventions. Common mHealth modalities include short messaging service (SMS) or text messaging, smartphone applications or ‘apps’, and social media. Below are definitions of each technology type with relevant examples of weight loss interventions for each.
- SMS Messaging: SMS messaging allows researchers to deliver short messages directly and instantaneously to individuals at any time, place or setting. These messages can be individually tailored and include daily or weekly tips, encouragement, and feedback for weight loss.2
- Mobile Apps: Mobile apps are programs designed to run on a mobile device such as a smartphone or tablet. Researchers can either use commercial available health apps (e.g. MyFitnessPal)3 or develop and test their own apps for intervention delivery.4
- Social Media: Social media includes online sites such as Facebook, Twitter and Instagram that allow individuals to participate in social networking by connecting and interacting with one another. Social media has been used both as the primary intervention delivery mode5 as well as in conjunction with other modalities (e.g. in-person sessions, mobile apps, print materials).6
What resources are out there for researchers looking to leverage technology?
If you are looking for resources to help you increase the utilization of technology in your work, below are a few resources that may be helpful to you:
- SBM BIT SIG: Collaborate within SBM and follow the Behavioral Informatics & Technology (BIT) Special Interest Group @SBMDigitalHealth.
- Journal of Medical Internet Research (JMIR): JMIR is a leading journal for published articles on digital health with a high impact factor (5.175). Check out JMIR mHealth and uHealth for studies focused on mobile apps, computer technologies, and wearable technology.
- mHealth Evidence Database: Developed in coordination with the World Health Organization, this is a databases that brings together published literature on mHealth to help you stay up-to-date on the current state of the evidence.
References
- Internet/Broadband Fact Sheet. January 12, 2017; http://www.pewinternet.org/fact-sheet/internet-broadband/#. Accessed January 20, 2017.
- Patrick K, Raab F, Adams MA, et al. A text message–based intervention for weight loss: randomized controlled trial. Journal of medical Internet research. 2009;11(1).
- Laing BY, Mangione CM, Tseng C-H, et al. Effectiveness of a smartphone application for weight loss compared with usual Care in Overweight Primary Care PatientsA randomized, controlled TrialSmartphone application for weight loss in overweight primary care patients. Annals of internal medicine. 2014;161(10_Supplement):S5-S12.
- Carter MC, Burley VJ, Nykjaer C, Cade JE. Adherence to a smartphone application for weight loss compared to website and paper diary: pilot randomized controlled trial. Journal of medical Internet research. 2013;15(4).
- Valle CG, Tate DF, Mayer DK, Allicock M, Cai J. A randomized trial of a Facebook-based physical activity intervention for young adult cancer survivors. Journal of Cancer Survivorship. 2013;7(3):355-368.
- Herring SJ, Cruice JF, Bennett GG, Davey A, Foster GD. Using technology to promote postpartum weight loss in urban, low-income mothers: a pilot randomized controlled trial. Journal of nutrition education and behavior. Nov-Dec 2014;46(6):610-615.
How to Engage Students With Your Course Syllabus and Content
Education, Training, and Career Development (ETCD) Council corner
Amy G. Huebschmann, MD, MS, ETCD Council chair
In each issue of Outlook, look to the ETCD Council corner for information related to our mission, which is to provide SBM members with opportunities and support to enhance their training and career development throughout all phases of their careers in behavioral medicine. The focus of this ETCD Corner segment is on effective teaching strategies, including how and why teachers should develop a good syllabus. I interviewed a panel of members from our ETCD council to get their insights. This topic is timely as the ETCD council is currently working with the Society for the Teaching of Psychology (STP) to connect SBM members with the resources that STP maintains on their website.
ETCD Council panelists:
- Jamie Bodenlos, PhD, Department of Psychology, Hobart and William Smith Colleges
- Vicki DiLillo, PhD, Department of Psychology, Ohio Wesleyan University
- Barbara Stetson, PhD, Department of Psychological and Brain Sciences, University of Louisville
ETCD Council: Why is it important to create a good syllabus?
Summary of panelists’ responses: The panelists agreed that a good syllabus is very important for numerous reasons. Each commented that it serves as a roadmap for students to understand the expectations and pacing of the course. In addition, they noted that planning a syllabus has several potential benefits for the instructor, including engaging students with the material and mapping learning goals with assignments. Here are some of their specific comments on the importance of a good syllabus:
Dr. Bodenlos: As the instructor, a good syllabus helps me to formulate my plan to the course. I make sure that my assignments and course plan line up with the learning goals. The syllabus also communicates expectations for the course to my students. It is our map for the semester which is why it is critical for it to be well thought out. It is the most important document for the course.
Dr. DiLillo: My overarching goal for a syllabus is to let students know very specific course expectations, including learning objectives; course content, assignments, assessments, and evaluations; classroom behavior expectations; as well as responsibilities for me as an instructor. I strive to be explicit at the outset to avoid any later misunderstandings.
Dr. Stetson: A highly organized syllabus up front makes the actual delivery of content and development of assignments and exams much easier for the instructor. A good syllabus also sets the tone for the class. By conveying enthusiasm for the topic and the relevance of the material, student engagement may be enhanced. Up to date syllabi are also critical to keep up with changes in the field, current events and even accreditation standards for programs (e.g., American Psychological Association site visitors review all course syllabi and comment on depth, breadth and timeliness of graduate level syllabi readings).
ETCD Council: What are some challenges you have experienced when developing a syllabus for a course that you are going to teach for the first time? What advice do you have for others who are developing a syllabus for a new course?
Summary of responses: The panelists agreed that there are many challenges when developing a course —each panelist commented that predicting the optimal pace of a new course is particularly difficult, as it is difficult to accurately judge how long it will take to cover a particular topic. In terms of advice to address these challenges, most panelists suggested reviewing an example syllabus from colleagues who teach a similar course, as this provides a starting point on what is typical for the learners at this level in terms of course content, assignments, and pacing. The need to tailor the pacing of the class to the level of the learners was another common theme. Each panelist also comments on some specific challenges and potential strategies to address them:
Dr. Bodenlos: The learning goals are always challenging when developing a course for the first time. Go over your learning goals and assignments with a colleague or someone in your teaching and learning office to get some feedback. It’s often helpful to put multiple course assignments on a large calendar to take a look at when assignments and exams are to spread out grading.
Dr. DiLillo: The first time I teach a course, my biggest challenge is predicting the pace. To address this, even when I’ve taught a course several times, I build in one or two catch-up days during the semester to allow some built-in flexibility.
Dr. Stetson: Two other challenges include: a) keeping large classes continuously engaged while also covering core content; b) teaching undergraduate courses with enrollees who have a wide range of backgrounds and skill levels. By getting to know the student populations, these challenges may be met with a range of assignments, such as letting students choose between assignments (in some cases), and assignment exam options that play to the strengths of various students. To keep learners engaged, it helps to use interactive approaches during class. Encourage attendance and emphasize the importance of critically thinking about the content in each class, as learners will otherwise tend to simply focus on exams. Be sure to clarify how students will be evaluated and policies on accepting assignments.
ETCD Council: Going beyond the syllabus, what advice do you have about developing a course?
Summary of responses: The panelists agreed that educators should not expect to “nail it” the first time they teach a course. Rather, they all recommended adapting the course to student feedback. The panelists also shared insightful recommendations on some specific ways to track and incorporate students’ feedback, and other tips on developing an outstanding course:
Dr. Bodenlos: I always save a copy of my syllabus labeled “future classes” and keep notes/comments throughout the document to remind myself of what worked, what didn’t, and what I want to change the next time I teach the course. Also, make material relevant for your students, whether you have them monitor their own health behaviors or you bring in guest speakers from the field. When students reflect on how the material relates to their life and their own behaviors, that is often just as helpful as real world case examples, and it’s more personal.
Dr. DiLillo: In my opinion, it’s critical to know both your goals for the course and your student audience. For example, teaching health psychology to first and second year pre-physical therapy students in a large lecture course is very different from teaching health psychology to more advanced psychology majors in a seminar format. I find it helpful to go to the teaching and learning literature to identify any particular pedagogical strategies that are particularly well suited for the course I’m developing. Furthermore, I always view my courses as works in progress. In particular, I see my first iteration of a class as a bit of an experiment. I make my best educated decision about content, pacing, assessments and assignments, and modify subsequent versions of the course based on student feedback and course-related data I collect during the semester.
Dr. Stetson: Consider using a blend of existing textbooks and curated journal articles. Online resources such as TED Talks and YouTube© videos can be immensely helpful for anchoring readings and engaging students. It is useful to gather student feedback about course content throughout the course. For example, administering open-ended fill-in/short answer recall items at the end of class, is a helpful way to ascertain the degree to which students understand what was actually covered, and whether the content you are covering is at the appropriate level. For undergraduate teaching, this can also supplement the class participation evaluation. I also advise instructors to be very clear about course policies and encourage students to be proactive in their instructor communication (e.g., during class, before and after class, during office hours, email).
New Articles from Annals of Behavioral Medicine and Translational Behavioral Medicine
SBM's two journals, Annals of Behavioral Medicine and Translational Behavioral Medicine: Practice, Policy, Research (TBM), continuously publish online articles, many of which become available before issues are printed. Three recently published Annals online articles are listed below. There are no new TBM online articles to share.
SBM members who have paid their 2016 membership dues are able to access the full text of all Annals and TBM online articles via the SBM website by following the steps below.
- Go to the Members Only section of the SBM website (http://www.sbm.org/membership/members).
- Log in with your username and password.
- Click on the Journals link (listed third in the list of member benefits).
- Click on the title of the journal which you would like to electronically access.
To check if you are a current SBM member, or if you are having trouble accessing the journals online, please contact the SBM national office at info@sbm.org or (414) 918-3156.
Annals of Behavioral Medicine
Honors and Awards
Congratulations to the following Society of Behavioral Medicine (SBM) members who recently received awards or were otherwise honored. To have your honor or award featured in the next issue of Outlook, please email ahahn@sbm.org.
Rachel Shelton, ScD, MPH
Dr. Rachel Shelton, assistant professor of sociomedical sciences at the Mailman School of Public Health, has received a four-year research scholar grant from The American Cancer Society to conduct one of the first studies on sustaining and adapting a nationally disseminated program for addressing cancer disparities in community settings.
Stacy Ogbeide, PsyD
Dr. Ogbeide and colleagues received a Health Resources and Service Administration Behavioral Health Workforce Education and Training program grant. This grant will help to support their Program for the Integrated Training of Counselors in Behavioral Healthcare.
Brie Turner-McGrievy, PhD, RD
Dr. Turner-McGrievy associate professor of health promotion, education, and behavior (HPEB), has received the Excellence in Weight Management Outcomes Research Award from the weight management dietetic practice group of the Academy of Nutrition and Dietetics, which supports the professional practice of preventing and treating overweight status and obesity. She was honored with this award at a ceremony held during the 2017 Food & Nutrition Conference & Expo in Chicago.
Bradford W. Hesse, PhD; David K. Ahern, PhD; Ellen Beckjord, PhD, MPH
The book “Oncology Informatics: Using Health Information Technology to Improve Processes and Outcomes in Cancer,” edited by SBM members Bradford W. Hesse, David K. Ahern, and Ellen Beckjord received a PROSE (Professional and Scholarly Publishing) award for “Best Text in Clinical Medicine: 2017 by the Association of American Publishers. The same book received a “Highly Commended” recognition by the British Medical Association.
Lisa G. Bandong, MPH
On October 8, 2017, Ms. Bandong received the 2017 San Diego County Breastfeeding Coalition’s Breastfeeding Champion Award, an annual leadership advocacy award to promote breastfeeding as a public health priority. She has been a breastfeeding advocate in her personal and professional life having been both a breastfeeding student and employee through the California State University system. Her work has allowed her the opportunity to see firsthand the varying degree of support and accommodation available to breastfeeding students and employees on campuses across California.
Barbara Andersen, PhD
Dr. Andersen recieved the 2018 American Psychosocial Oncology Society Outstanding Education and Training Award. The award was established to recognize a leader who has enhanced the field of psychosocial oncology through the education and training of new investigators and clinicians.
Carla Miller, PhD, RD
Dr. Miller received a National Institute of Diabetes and Digestive Kidney Diseases grant for her project, "Impact of Augmented Care at the Worksite for Diabetes Prevention." This is a 5-year trial to evaluate the impact of augmented care on weight loss compared to a standard behavioral weight loss lifestyle intervention.
Steven N. Blair, PED, FACSM
Dr. Blair received an honorary doctorate degree of doctor medicinae honoris causa (dr.med.h.c.) from Southern Denmark University.
Kim L. Lavoie, PhD and Simon Bacon, PhD, FTOS, FCCS
Drs. Lavoie and Bacon were elected to the Academy of Behavioral Medicine Research.
Belinda Borrelli, PhD
Dr. Borelli received the 2017 Boston University-Evans Center Institute for Biomedical Research Excellent Research Collaborator of the Year Award. This award is given to individuals who have made outstanding contributions to research collaboration at Boston University. After accepting nominations from peers, awards are determined by a special committee with support from the administration. Dr. Borrelli launched the Boston University Mobile and Electronic Health Affinity ARC (ME-ARC) in January of 2016 and serves as the Director. She is Professor and Director of Division of Behavioral Science Research at Boston University.
Rebecca Krukowski, PhD
Dr. Krukowsi and her team were awarded a $3.3 million, five year, National Institutes of Health grant to test promising approaches to help individuals in the Memphis area manage their weight when they quit smoking with their project, Fit and Quit.
Members in the News
The following Society of Behavioral Medicine (SBM) members and their research were recently featured in news articles, videos, or journals. To have your news spot featured in the next issue of Outlook, please email ahahn@sbm.org.
Alicia Dahl, MS; Caroline Dunn, MS, RD/LDN, Alycia Boutte, MPH; and Brie Turner-McGrievy, PhD, RD
Alicia Dahl, Caroline Dunn, Alycia Boutte, and Dr. Brie Turner-McGrievy recently had their article titled, "Mobilizing mHealth for Moms: A Review of Mobile Apps for Tracking Gestational Weight Gain," published in the Journal of Technology in Behavioral Science.
Alicia Dahl, MS and Brie Turner-McGrievy, PhD, RD
Alicia Dahl and Dr. Turner McGrievy recently had their article titled, "Characterizing Diabetes, Diet, Exercise, and Obesity on Twitter," in the International Journal of Information Management.
Elena Salmoirago-Blotcher, MD, PhD
Dr. Salmoirago-Blotcher had paper titled, "Tai Chi Is a Promising Exercise Option for patients With Coronary Heart Disease Declining Cardiac Rehabilitation" published in the Journal of the American Heart Association. She has also been featured on the CBS Evening News, in Time Magazine, Daily Mail, China Global Television Network, Science Daily, Medpage Today, and Medical News Today.
Kimlin T. Ashing, PhD
Dr. Ashings book, Detecting & Living with Breast Cancer for Dummies was featured on City of Hope's website. The book is meant to give survivors a handheld practical guide for hopeful living, with information and resources to help them get optimal care and live their healthiest life possible after this illness and its treatments.
Belinda Borrelli, PhD
Dr. Borelli was featured on 12 NPR stations during their Public Health Minute, talking about her work targeting underserved populations such as those with low income, inner city youth and adults, Latinos, people with mobility impairments, medically ill populations, older adults, and Native-Americans.
Visit the SBM Job Opportunities page for additional positions.
