

Bonnie Spring, PhD
PRESIDENT'S MESSAGE
On Doing It All
It is a great honor to serve as your President and a genuine pleasure to work with our talented membership. The Society of Behavioral Medicine celebrates its 30th birthday in 2009. We are old enough to have learned a thing or two, yet energetic and idealistic enough to act as a force for good. As SBM approaches this next developmental milestone, it behooves us to reflect on its history and future aspirations. In this column, I will offer my perspective. Let me also extend an open invitation to share yours.
Past
The NIH Roadmap has ushered in an exciting era of translation between research and practice. I am fond of a model of the roadmap published by Westfall, Mold and Fagnan (2007) and reprinted below. I like this particular depiction because it reminds me of SBM's history. Since I began attending annual meetings, the membership's modal research focus has rotated through each major element of Westfall et al's translational cycle. In late 1970s and early 1980s, our founding figures built a strong basic science foundation for the field. The prevailing emphasis at annual meetings was on biopsychosocial mechanisms that underlay behavior and disease.
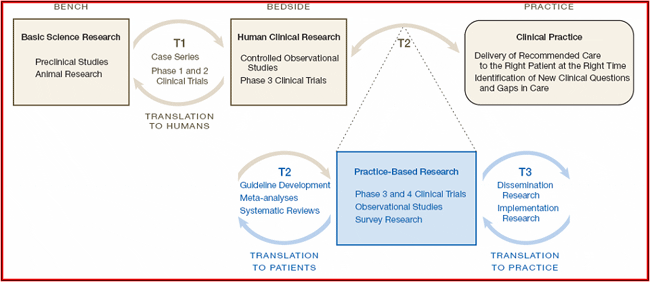
Westfall, JM, Mold, J, & Fagnan, L (2007) Practice-Based Research: “Blue Highways” on the NIH Roadmap. JAMA, 297: 403-406. Copyright© 2007 American Medical Association. All rights reserved.
In the later 1980s and early 1990s, a strong T1 translational interest began to emerge. Conference attendees were treated to new research that established parallel biobehavioral processes across animal and human studies. The Trans-Institute NIH Behavioral Medicine study section of the mid- to late 1990s pressed forward the T1 translational curve. Reviewing both basic research and applied clinical trials, the Review Group evolved a shared point of view. A core premise was that the intervention trials of greatest lasting value would be those that lay bare a theoretical understanding of biopsychosocial mechanisms.
By 2000, the T1 interest in early phase intervention development had given way to an emphasis on more formalized phase III trials, first of efficacy and then of effectiveness. Many of us had easily transferred the methods of basic science experimentation to intervention development. Now we scrambled to learn a new science of clinical trials methodology. Basic science presentations at the annual meeting became fewer in number. Emphasis shifted subtly to which interventions work and how to learn them.
Also around the turn of the century, a strong interest in public health models gathered momentum at SBM. On the one hand, our membership rejoiced that many intensive behavioral medicine interventions show strong efficacy. On the other hand, we grappled with the realization that penetration into the population at greatest need of intervention remains modest. There arose great concern about extending behavioral medicine's reach to have broader population impact, especially among the underserved. A productive outcome was full-scale embrace of ecological models that endorse intervening synergistically at multiple levels (individual, interpersonal, organizational, community, and public policy) in order to magnify and sustain healthful change.
Release of the Institute of Medicine's report on health care quality (IOM, 2001) was a sentinel event that marked the beginning of the current decade. As the report aptly stated, "Between the health care we have and the care we could have lies not just a gap, but a chasm (p.1)." To address the translational gap, SBM formed two standing committees: Evidence Based Behavioral Medicine (EBBM) and Health Policy. Dividing up the ecological space, EBBM focused chiefly on interventions targeted at the individual and interpersonal levels, whereas Health Policy emphasized intervention at the community and public policy levels. Both Committees took steps towards T2 translation. EBBM endorsed comprehensive, transparent reporting of clinical trials and increased engagement in research synthesis. Health Policy crafted policy briefs that give legislators a pithy, user-friendly overview of evidence and action recommendations for such pressing health problems as childhood obesity.
Crossing the boundary between individual and population outreach in such a manner was sheer cutting edge brilliance on SBM's part. Few institutions have tried to harmonize individual clinical and public health approaches, especially across the multiple disciplines that comprise SBM. Although abundantly worthwhile, the task is challenging. Misunderstandings abound. They are a natural part of the process of recognizing differences, understanding and respecting them, and moving forward.
Present
We often describe SBM as a "big tent." The citizenry in our tent hails from 17 different primary professions and claims topical interests represented by 15 SIGs. Our heterogeneity generates exciting cross-talk that draws members to annual meetings. Maintaining SBM's balanced portfolio of interests and approaches is vitally important. Diversity in discipline, specialty, and approach is a large part of what invigorates the Society.
Our members' engagement in all phases of Westfall et al's (2007) translational cycle conveys particular richness. No phase is optional: discontinuing any step jeopardizes the entire enterprise of behavioral medicine research and practice. Of late, we are especially keen to undertake T3 translation, whereby we disseminate, implement, and adapt (but do not enervate) effective treatments to new contexts. We aspire also to grow more adroit at the reciprocal translation processes of practice-based research. But we cannot amputate the vital pipeline of basic research and new treatment development. Doing so would eventually consign us to a dark age of stagnant science and outmoded treatment. In a nutshell, we need to do it all because we are interdependent. Our game is not a zero sum one. We succeed not by crowding out our neighbor, but rather by making the tent, the funding pot, and the job market big enough to support us all.
Our 2007 annual meeting featured a debate on the question: what kind of evidence is most needed to advance behavioral medicine? My answer is: many different kinds. According to the philosophy of evidence-based practice, the kind of evidence best suited to answer a question depends upon the type of question being asked. Trying to use the same research design to answer every important practical question would be like trying to function as a carpenter using only one tool. To answer prognostic questions about risk or protective factors or developmental course, we need observational cohort studies. To learn whether a new treatment improves outcomes compared to an alternative treatment, a well-conducted randomized controlled trial (RCT) is ideal. But it will not always be feasible to conduct an RCT, and well-implemented quasi-experimental studies may offer more compelling insight than a poorly conducted RCT. It is particularly hard to conduct RCTs to test policy interventions. Just try to imagine the state legislature that would agree to have its policies randomly assigned! To answer some questions, an RCT is at best inefficient and at worst inappropriate. For example, when trying to gauge a treatment's acceptability to an unfamiliar population, initial qualitative methods are much more informative.
Importantly, we cannot wait for the perfect evidence before taking action to address urgent public health problems. Following the evidence-based practice process, we and those affected by the decision, need to select an initial action course based upon the best evidence available, integrated with consideration of contextual characteristics and resources. Having chosen an initial intervention, the equally important next steps are to collect and analyze context-specific data on processes and outcome, and then adjust course based on the new practice-based evidence (Council on Evidence-Based Behavioral Practice, 2008).
Future
At its post-conference strategic planning meeting in San Diego, SBM's Board discussed several new initiatives. Their intent is to increase the Society's engagement in translational activities and its impact on practice and policy. A further aim is to enhance the infusion of new talent into SBM leadership by creating additional opportunities for members to interface with the Board. All SBM members received an invitation to participate in four new working groups, each of which evaluates a potential new undertaking for SBM. The first working group, headed by Paul Jacobsen, PhD, is considering whether SBM should undertake preparation of practice guidelines. The second group, chaired by Jeff Goodie, PhD, examines SBM's potential involvement in practice based research networks. The third, chaired by Barbara Resnick, PhD, CRNP, evaluates whether SBM wishes to undertake a new journal addressing the needs of behavioral medicine clinicians and public health practitioners. The fourth group, headed by Amanda Graham, PhD, examines where consumers currently turn to find information about evidence-based behavioral medicine practices and how SBM might engage with those resources.
Also to increase the Society's engagement in policy and practice, SBM formally endorsed a clinical practice guideline: USPHS's Treating Tobacco Use and Dependence: 2008 Update, released on May 7, 2008. Based upon review of 8,700 research articles, the USPHS Tobacco guideline draws important new conclusions. For the first time, the guidelines panel found the evidence sufficient to conclude that the combination of counseling and medication is more effective than either alone. Many SBM members participated in crafting the 2008 guideline, either as panelists or reviewers. The ability to create, evaluate and endorse treatment guidelines represents the culmination of many years of hard work. The accomplishment reflects SBM members' increased experience in conducting systematic reviews and guidelines evaluation, as well as increased collaboration between the EBBM and Policy Committees. In its endorsement, SBM enjoys the excellent company of 57 other professional organizations, including the American Medical Association, American Cancer Society, American Lung Association, American Heart Association, and American Public Health Association.
To enhance its policy involvement further, SBM joined forces with two important organizations: COSSA and Partnership for Prevention. COSSA, a consortium of more than 100 professional associations, is an advocacy organization that promotes attention to and Federal funding for the social and behavioral sciences. Partnership for Prevention is a national membership organization dedicated to building evidence of sound disease prevention and health promotion policies and practices, and advocating their adoption by public and private sectors. An article about Partnership for Prevention, prepared by the Society and Professional Liaison Council, will appear in the next issue of Outlook.
We face exciting times. SBM's founding vision remains as astute today as it was 30 years ago. A small number of behavioral risk factors that are amenable to intervention now account for a third of the global chronic disease burden and half of all deaths from chronic disease (Ezzati & Lopez, 2004). The psychosocial needs associated with chronic diseases are becoming recognized (Institute of Medicine, 2008). SBM members are united in their commitment to understand and intervene upon biopsychosocial pathogens in a manner that improves public health. The journey ahead will be an adventure; I look forward to sharing it with you.
Best wishes for a joyful, restorative summer season.

Bonnie Spring, PhD
President, Society of Behavioral Medicine
References
Council on Training in Evidence-Based Behavioral Practice (March, 2008). White paper on Definition and Competencies for Evidence-Based Behavioral Practice. http://www.ebbp.org/documents/EBBP_Competencies_Mar2008_Web.pdf
Fiore, M.C. et al (2008) Treating tobacco use and dependence: 2008 Update. USPHS. http://www.surgeongeneral.gov/tobacco/
Institute of Medicine. (2001) Crossing the quality chasm a new health system for the 21st century. Washington, D.C.: National Academy Press
Institute of Medicine (2008) Cancer Care for the Whole Patient: Meeting Psychosocial Health Needs. Washington, DC: National Academies Press
Westfall, JM, Mold, J, & Fagnan, L (2007) Practice-Based Research: "Blue Highways" on the NIH Roadmap. JAMA, 297: 403-406